Representatives from NPOs, provincial health departments and international aid organisations gathered on Thursday in Witbank, Mpumalanga, to reflect on South Africa’s progress in addressing HIV and Aids over the past 20 years. They also discussed new challenges at the engagement event, hosted by healthcare consulting company BroadReach.
South Africa aims to meet the UN’s 95-95-95 goals: diagnosing 95% of all HIV-positive individuals, providing antiretroviral therapy to 95% of people who have HIV and achieving viral load suppression for 95% of those treated by 2030.
Speakers reflected on the progress the nation has made toward achieving those goals and discussed how to put lessons learned during the past 20 years into practice moving forward.
Twenty years of progress
Dhirisha Naidoo, BroadReach’s chief of party, started her career in healthcare 20 years ago at a small mission hospital in Durban where people from across the country came to seek care. At that time, many of those seeking care were on stretchers and wheelchairs and were often emaciated.
Things are very different now — treatment and healthcare options are more accessible, Naidoo said. Scientific breakthroughs, including the roll-out of antiretroviral therapy in South Africa in 2003, changed HIV from a death sentence to a viral infection that can be managed with a daily drug regimen.
A July 2022 press release from Health Minister Dr Joe Phaala said South Africa is currently at 94-78-89, meaning 94% of HIV-positive individuals have been diagnosed, 78% of those diagnosed are on ARVs, and 89% of those on ARVs have had their viral loads suppressed.
Naidoo credited the organisations in attendance, including Pepfar, the US President’s Emergency Plan for Aids Relief, and the United States Agency for International Development, for working together to help South Africa hit these benchmarks.
Addressing new challenges
Dr Ernest Darkoh, BroadReach’s co-founder, said the work was not going to get easier. From here on out, he said, the remaining HIV-positive individuals who are not on ARV therapy or have not yet been reached by healthcare systems are going to be more difficult to identify.
“You’re increasing the needle-in-a-haystackness of the whole situation,” he said, “because fewer of them are out there.”
Further, some of those who remain unreached belong to stigmatised populations, such as LGBTQ+ individuals and sex workers. Others may live in areas where traditional attitudes surrounding sex and treatment can make it more challenging to access care. Darkoh said health systems need to focus on building trust and partnerships with organisations run by members of these populations to reach them.
“We’ve gone into the hard zone,” he said. “Yes, it’s a great success, but these bits are exponentially harder than what we’ve done. And therefore… we require a lot more innovation, a lot more out-of-the-box thinking, a lot more willingness to embrace non-traditional partners.”
Using new systems and technologies to reach more people
At the same time, Darkoh said, “treatment fatigue” would be a pressing concern moving forward, as many HIV-positive individuals who have been on antiretroviral therapy for many years struggled to continue adhering to strict drug regimens.
Darkoh and other speakers said that to address treatment fatigue, health systems needed to make medication easier for patients to access and to adopt new treatment technologies.
Linda Dlamini, a director at KwaZulu-Natal’s Department of Health, said that during the past several years, the Covid-19 pandemic, social unrest and 2022’s flooding had pushed the department to think outside the box with its treatment delivery methods, including developing “pick-up points” and delivering medicine directly to people. These techniques were also applicable to getting HIV treatment to those who need it, she said.
Darkoh said that eventually injectable ARV medications, which would allow patients to receive an injection every one or two months rather than taking a pill every day, may make it easier for HIV-positive individuals to adhere to treatment regimens.
He said he also would like to see more energy devoted to developing an electronic medical record-keeping system in South Africa to replace the current paper-based record-keeping system. Now, when a patient moves from one clinic to another, a new paper-based record is opened for them without any of their health history from the previous clinic. This makes it difficult to track if people are keeping up with their treatment regimens, and to ensure HIV treatment statistics are accurate.
“We may be chasing targets that don’t exist, because… you’re counting them as not on treatment [at one clinic], but they’re on treatment [at another],” said Darkoh.
An electronic medical record-keeping system would solve this problem, Darkoh said, allowing health systems to more accurately gather HIV-related data and ensure that patients continue receiving the treatment they need when they move from one clinic to another.
The need for strong partnerships
Darkoh also emphasised that creating strong partnerships between the government, NPOs and private organisations was key to reaching the UN’s 95-95-95 goals and building sustainable HIV treatment infrastructure.
But ultimately, Darkoh said, international organisations like Pepfar need to work harder to ensure they are transferring skills to local systems and organisations, and building the capacity of the government to eventually take the reins of South Africa’s HIV response campaign.
He said this required having full-time paid staffers in the government who are responsible for fundraising, grant management and building partnerships with NPOs.
Dr Sandile Tshabalala, the head of KwaZulu-Natal’s Department of Health, also called on South Africa’s international partners to focus on transferring skills to local organisations.
“Do leave the skills, so that when you go back to… where you have come from, we have skills that we can use to ensure that whatever good value they have started does not go down,” Tshabalala said. DM/MC




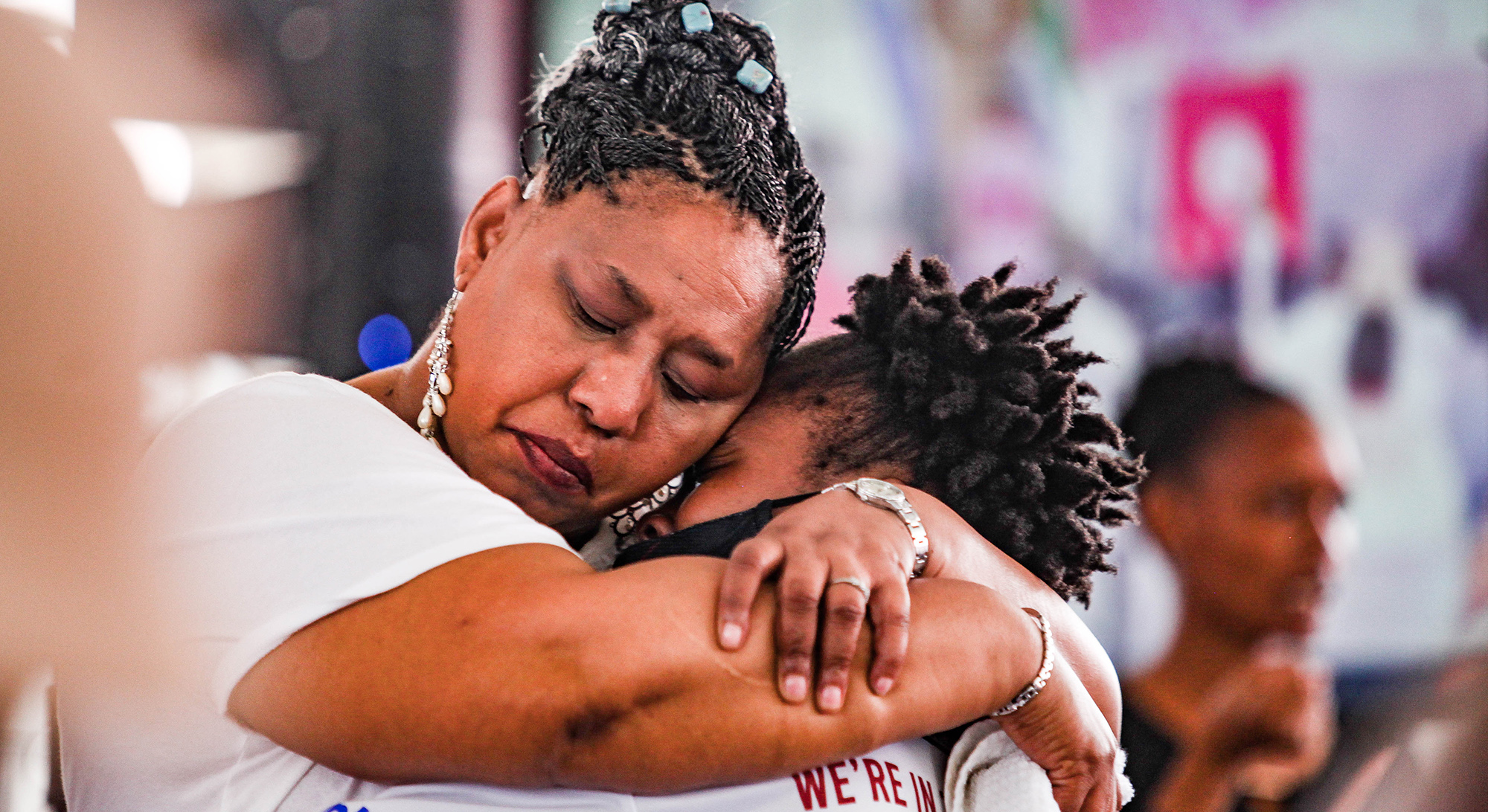 Minister Hendrietta Bogopane-Zulu hugs and comforts a young woman at the World Aids Day Commemoration on 1 December 2020 in Soweto, South Africa. (Photo: Gallo Images / Sharon Seretlo)
Minister Hendrietta Bogopane-Zulu hugs and comforts a young woman at the World Aids Day Commemoration on 1 December 2020 in Soweto, South Africa. (Photo: Gallo Images / Sharon Seretlo)