My run happened to be the same morning that Minister of Health Zweli Mkhize’s statement on the “misdemeanours” of Professor Glenda Grey was doing the rounds on WhatsApp. It had been released at 10:30pm on Wednesday, the night before. By the time I got home, social media was ablaze.
The hullabaloo that has followed, which has now led a large segment of the scientific and medical community to denounce the actions of a government that only a few weeks ago it was foursquare behind, is well known. But while it is right to uphold Gray’s right to freedom of speech, we should be concerned that some of the underlying issues Gray and other health experts were raising are not getting the same attention.
One of these is access to sufficient food and nutrition, hunger, and its impact on health and inequality.
Malnutrition is stalking the land
One of Gray’s 'sins' was to have had an outburst on the issue of severe acute malnutrition (SAM) in children. She claimed, wrongly, that SAM was being seen again “after decades” at Chris Hani Baragwanath (CHB) hospital as a result of the prolongation of the lockdown.
But why would Gray, a paediatrician who knows all about SAM, make these claims? Are they pure fiction?
South Africa is categorised as a middle-income country. But tragically, food insecurity was epidemic in our country well before the lockdown. So too is malnutrition in children.
According to the best data we have, pooled annually by the Children’s Institute (CI) at the University of Cape Town in their annual Child Gauge (a high-quality publication with a foreword this year by First Lady Doctor Tshepo Motsepe), in South Africa, unlike neighbouring countries, while “there is enough food to cater for the majority of the country’s population … distribution and accessibility constraints, coupled with higher rates of poverty and inequality, mean that a substantial portion of the country’s population is food insecure”.
As a result, the Child Gauge records, in 2018, 11% of children lived in households that reported child hunger and, linked to this, a shocking 27% of all children under five are stunted (defined as a medical condition that arises from prolonged under-nutrition and which affects physical and brain development).
For these well-known reasons, in the middle of March 2020, as the National Command Council, and the president’s special adviser on social policy Professor Olive Shisana, made preparations to institute a lockdown, ensuring food security for children should have been a flashing red light; the president and his Cabinet should have foreseen the need to commence programmes for food relief for the poor as soon as the lockdown started.
On the morning of 23 March, I was in a meeting with Minister Mkhize and more than 40 health experts. In a discussion about the risks and benefits of a possible lockdown, I heard Professor Shabir Madhi and others advise the government that the success of a lockdown depended on effective measures to mitigate its negative impact on the poor and that time should be taken to put these measures in place.
But their advice was not heeded. The lockdown was announced by President Cyril Ramphosa at 7pm that same evening.
However, measures to relieve the poor were not announced until 21 April, a month later. Food relief came very late, initially in the form of food parcels (whose caloric content is insufficient ) which even today some families have still not received. Although the Child Support Grant was increased in May, it was per adult beneficiary rather than per child.
In many cases, it fell to communities and volunteers to step up and meet the needs of children.
These measures have done a little, but not enough, to assuage the hunger. Millions of people, including children who have an inflexible constitutional right to “basic nutrition” which the state should provide for, still lack sufficient food.
And this claim is not anecdotal.
Since the start of the lockdown, survey after survey has reported increases in hunger.
For example, according to a University of Johannesburg/ Human Sciences Research Council (HSRC) survey, 34% of the people surveyed between 18 to 27 April reported that they had gone to bed hungry (up by 6% from an earlier survey). An open-ended question asking respondents to report “the worst thing about the lockdown” included the following heart-rending responses:
“I am an unemployed mother of three kids and I don’t know where my next meal is coming from.”
“Staying indoors with an empty stomach, and feeling helpless and breastfeeding a small child and not be [sic] able to pay rent.”
This should not have been surprising. A larger survey of nearly 20,000 people (released by Minister Blade Nzimande on 26 April), also by the HSRC, had already set the alarm bells ringing. On “access to food” it found that:
“Just under a quarter (24%) of residents had no money to buy food. More than half (55%) of informal settlement residents had no money for food. About two-thirds of residents from townships also had no money for food.”
This, I believe, is the context in which we should understand the comments made by Professor Gray and colleagues, calling for the relaxing of certain aspects of the lockdown and the scaling up of others and evaluate the government’s angry response to them.
The interview that caused all the trouble
In the interview with News24 that caused all the trouble, Gray was reported to have said that:
“We are seeing children with malnutrition for the first time [at Chris Hani Baragwanath Academic Hospital]. We have not seen malnutrition for decades and so we are seeing it for the first time in the hospital.”
She later corrected this to say:
“Concerns were raised in the first week of May 2020 regarding the number of admissions for acute malnutrition, which appeared to be on the increase.
“The Chris Hani Baragwanath Hospital still sees admissions for malnutrition. The increase in the cases seen in the first week of May needs to be closely monitored.”
Gray’s assertions on malnutrition drew the particular ire of the Minister of Health and his acting DG, Anban Pillay. In their statement of 20 May (benignly titled “Response to media queries”) they singled out this claim and roundly refuted it stating that:
“There has been a reduction in the number of cases of malnutrition that have been seen at Chris Hani Baragwanath Hospital POPD and the total admissions during the month of March and April 2020, when compared to the previous 4 years. To illustrate this, in April 2019 there were 2,885 patients seen and 500 admissions. However, in April 2020 there were 834 patients seen and 146 admissions.”
Gray was relying on anecdotes, they said, and therefore causing “unnecessary sensationalism” and “unnecessary anxiety to our citizens”. For this reason, she was publicly reprimanded. Predictably, the Minister’s statement won the support of the likes of EFF deputy leader, Floyd Shivambu, who tweeted:
“Well done for dismissing imposters, who are evidently singing for supper! Opportunism must always be nipped in the bud, and am sure it’s clear what should happen next.”
Another Twitter troll commented:
“Prof. Gray must be charged for spreading fake news. If a Minister can receive sanction for breaking the lockdown regulations, why not this industry apologist masquerading as a scientist?”
As if taking his lead from Shivambu, on the next day, 21 May, Pillay wrote to the Chairperson of the Board of the Medical Research Council (MRC) complaining about Gray’s “false allegations against government” and requesting that her “conduct” be investigated “given the harm it has caused to South Africa’s COVID response.” It seems the MRC Board is obsequiously ready to agree.
Case closed.
Has malnutrition increased?
The case, however, is clearly not closed in the court of constitutionally recognised human rights and public opinion. More than 300 senior academics have now signed a “statement of support for Professor Gray and the Principle of Academic Freedom of Speech”. On Sunday night a statement was issued by the prestigious Academy of Science for South Africa.
These statements are important. But, once again, there is something in the substance of Gray’s comments that risks being overlooked. To try to plug this hole I interviewed several of South Africa’s leading paediatric specialists and child-health researchers, to better understand what Gray had been getting at.
“Was she crying wolf?” I asked.
Their unanimous response was that, although it is not yet reflected in patient numbers or records, there will be a significant increase in child malnutrition as a consequence of Covid-19 and food insecurity following the lockdown.
According to Lori Lake, one of the editors of the Child Gauge:
“It’s difficult to put together any meaningful numbers simply because admissions and hospital attendance are down because of lockdown… the logic is clear that given the increase in the food basket price, given the increased number of people in need of income support, that children are going to be bearing the brunt of this and are particularly vulnerable.”
Professor Haroon Saloojee, Professor and the head of the Division of Community Paediatrics at Wits, (who was kindly asked to answer my questions by Professor Sithembiso Velaphi, the head of paediatrics at CHB) was able to provide more detail. He confirmed that paediatric admissions at CHB in April 2020 were down 66% from January to March but that this was due to the lockdown: “Like everyone else, we’ve reduced non-emergency admissions.”
The fate of Dr Gray is in the balance. It seems likely that she will soon be suspended as President of the SAMRC. The Board is doing as it was bid. Fortunately, Gray has lawyers, strong public support and justice on her side.
Before Covid-19, CHB admitted 15-25 cases of SAM a month, said Saloojee. However, in the first week of May “we did see a spike of eight cases”, which raised alarm, but this has not persisted through the rest of the month.
However, Saloojee stressed that the picture was far from complete. Asked whether there are likely to be cases of SAM in the pipeline:
“My answer is clear: we know that there will be an increase in food insecurity and hunger will impact on children’s nutritional status and higher rates of SAM can be expected across the country.”
“Hospitals, such as Bara, are a poor proxy of the real situation. There is a real possibility that malnourished children and others with other conditions are dying at home during the lockdown. We will only know the truth when we examine mortality statistics much later.”
This seems to be confirmed by a Maverick Citizen’s journalist in the Eastern Cape who reports that:
“The senior pediatric nurses are all confirming they are seeing the first cases of SAM... The problem is that the DOH has not called their stats-keepers back to the office yet — so there are no official stats. And they know they are wrong because they are required to keep SAM stats up to date.”
Saloojee points out that Gray was wrong in claiming that SAM was new. He says that while in the late 1990s they saw very little SAM at CHB, this changed with the advent of HIV when it rose as high as 13% of all admissions before, in the era of Antiretroviral therapy (ART), reducing to a stubborn 5%.
Finally, Professor Ashraf Coovadia, the Head of Department of Paediatrics and Child Health at Rahima Moosa Mother and Child Hospital, responded that:
“In short, I believe she is right, we just don’t know the scale of the problem; but what’s complicating the picture is the low numbers coming into hospitals in the last two months as a result of the lockdown.”
And “low numbers” is arguably where we find the sleight of science contained in Minister Mkhize’s reprimand. An uninformed reader could mistakenly think that the drop in numbers at CHB is because child health and nutrition has miraculously improved.
Sadly, it is not.
The reason that numbers are down, something that has been experienced at all public hospitals and clinics, is because many people have been afraid to go to hospital or unable to travel during the lockdown. This has had a profoundly damaging effect on other essential health interventions, like HIV and TB. It is another thing that should have been foreseen and mitigated by the planners of the lockdown from the very outset.
So what is to be done?
The fate of Dr Gray is in the balance. It seems likely that she will soon be suspended as President of the SAMRC. The Board is doing as it was bid. Fortunately, Gray has lawyers, strong public support and justice on her side.
Also fortunately, she can take steps to protect herself.
The same cannot be said for poor and vulnerable children. It’s the children we should be worried about and actively plan to help.
Professor Coovadia explained to me that children between the ages of six months and five years are the most vulnerable to malnutrition, which will have a long-term impact on their intellectual and physical development. He added that when children start to be admitted for severe acute malnutrition “it’s the tip of the iceberg”. Sadly, kids are a weathervane for deeper malnutrition among adults.
Professor Coovadia said that what was needed “yesterday” was a “proper surveillance system to assess the levels of food insecurity on health”. He suggested that this surveillance was most needed outside hospital settings and that community health workers already doing screening for Covid-19 would be ideal to do this.
“[To detect wasting] All you need is a tape to measure their mid upper arm circumference. It’s cheap, easy, quick, reliable and validated. It’s also recommended by the WHO.”
Follow the leader
Last night in his address to the nation President Cyril Ramaphosa again stated that “We appreciate the diverse and sometimes challenging views of the scientists and health professionals in our country, which stimulate public debate and enrich our response.” There can be no doubt this was a reference to the dispute on the MAC.
President Ramaphosa also recognised the problem the lockdown and the preparation of health facilities “to meet the expected surge of coronavirus cases” has inadvertently created for other health services. He said:
“We must make sure that we do not create the space for the emergence of other health crises.
“Routine health services should therefore be fully opened and continue to provide services with attention to childhood immunisation, contraceptive services, antenatal care, diagnosis and treatment of tuberculosis and HIV, management of chronic diseases and support for survivors of gender-based violence.”
We couldn’t agree more, except we would add malnutrition to his list.
Unfortunately, it seems that some of the president’s ministers and their advisers do not feel the same way. Getting over this spat by scaling up humanitarian relief and a health programme to end child malnutrition would be a more unifying response to Dr Gray’s claims than a divisive witch hunt.
It’s not too late for the government to change tack and repair the damage. But it might need the president to step in before the divisions become too deep.
Your move, Mr President. DM/MC





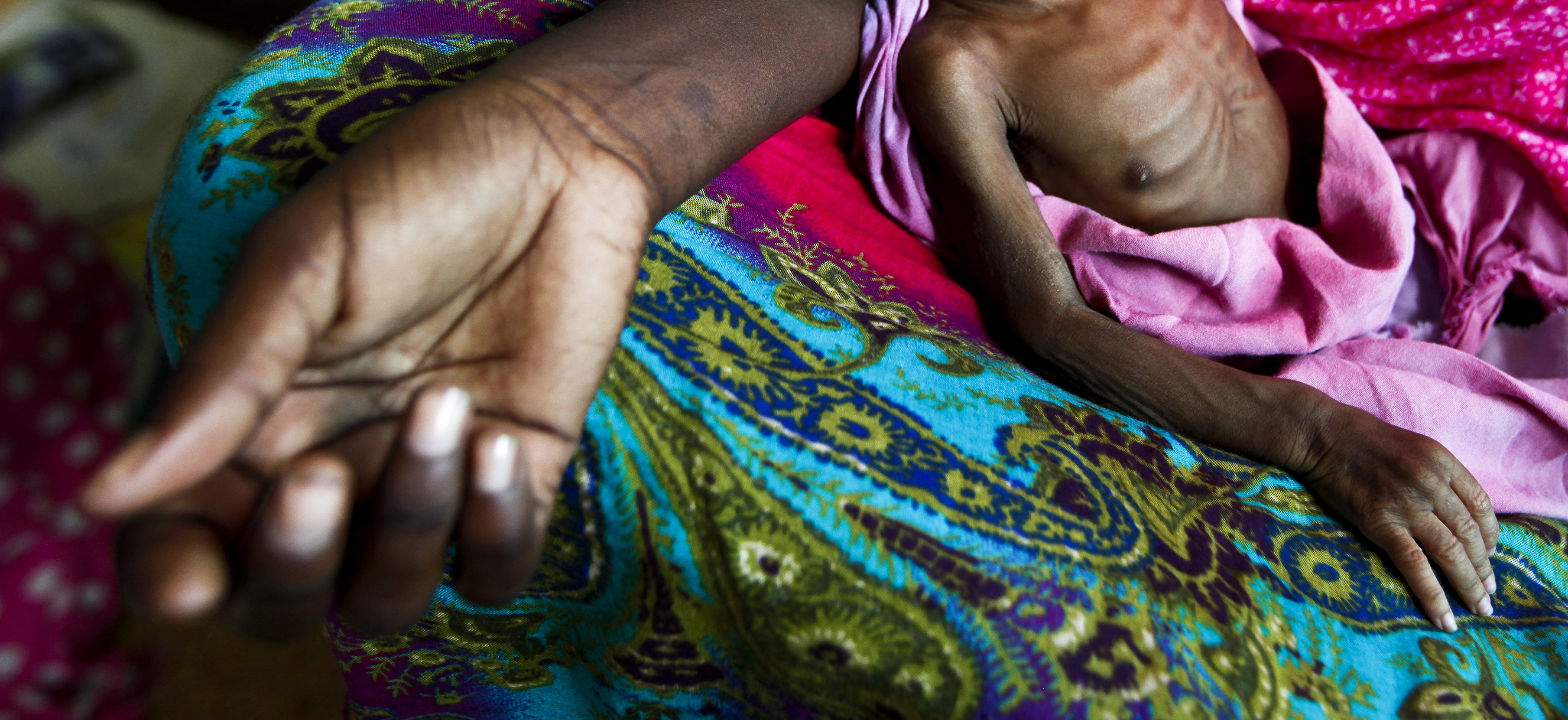 Children between the ages of six months and five years are the most vulnerable to malnutrition, which will have a long-term impact on their intellectual and physical development. (Photo: EPA / Dai Kurokawa)
Children between the ages of six months and five years are the most vulnerable to malnutrition, which will have a long-term impact on their intellectual and physical development. (Photo: EPA / Dai Kurokawa)