Simphiwe found out he was living with HIV in 2011. On finding out about his status, he reflects, “I tried to commit suicide, simply because I was afraid of disclosing to my family, to my colleagues, and to my friends. I was so scared that I was HIV-positive.” Fortunately, Simphiwe’s suicide attempt failed – although he did spend about three weeks in hospital for a pills overdose.
The fact that men are scared to test for HIV is not unique to Simphiwe. According to 2017 estimates from UNAIDS, just 26% of men in southern and eastern Africa have received an HIV test in the past 12 months and know their results, compared to 34% for women. This poses a huge problem to the HIV response. When a man does not know his HIV status he will not be able to access antiretroviral treatment, which when effectively suppresses the amount of HIV in the blood (the viral load), which does two things. First, it shortens life expectancy for the person living with HIV. This is bad for men – according to UNAIDS 2017 statistics, they are 70% more likely to die of AIDS-related causes than women. Second, it increases the likelihood of transmitting HIV when having sex without a condom. This is bad for young women and girls. Research has shown that the disproportionately high number of HIV infections among young women and girls in eastern and southern Africa – a primarily heterosexual epidemic – are from men on average 8.7 years their senior and then as they get older they transmit HIV to their sexual partners who are of similar age. As Dr Quarraisha Abdool Karim from the Centre for the Aids Programme of Research in South Africa says, “We’ve largely been dealing with one half of the equation. In order to be successful and effective, we need to be talking to both men and women.”
So why are men not accessing HIV services?
HIV services are primarily provided within health facilities and men do not use health services as much as women. “Women go if they are pregnant for antenatal care, for family planning services, take their children for immunisation etcetera,” points out Karim, “But most of the time, men don’t, particularly if you are thinking about young, healthy people.”
Dumisani Rebombo, Community Education and Mobilisation Manager for Sonke Gender Justice, adds, “It doesn’t mean the healthcare facility is more friendly to women, it is just that she has to go there… and by virtue of going through that door, you then have to test for HIV.” Simply because women are more likely to attend a health facility, they are more likely to get tested for HIV.
However, this is not the whole reason, and notions about what a “real man” is does come into play. “Hospitals are associated as a place for women,” says Simphiwe. “So if I go to hospital I will show that I am weak.” He is not the only one who thinks this. According to the International Men and Gender Equality Survey (Images) carried out in dozens of countries, there is evidence that men who hold rigid and inequitable norms are less likely to use HIV services. This means that men tend to be diagnosed with HIV very late, greatly increasing the likelihood of dying due to an AIDS-related illness.
What does this mean for young women and girls?
Current gender norms and roles are having a very negative impact on young women and girls because of the ways in which they grant men power over women and make it difficult for women to negotiate how or whether sex takes place. At present 60% of new HIV infections in eastern and southern Africa are among young women and girls aged 15-24 years, despite them only comprising 10% of the population. Rightly there has been increased emphasis over the past few years to address this urgently – but interventions have tended to primarily focus on empowering young women and girls. Karim says, “If we’re going to use treatment as prevention, just treating the women, getting women virally suppressed is not going to do it. We also need to prevent HIV infection in men.”
Malenga Constance Kganakga, Executive Manager of the National Strategic Plan at the South African AIDS Council, also highlights the problems of gender inequality, patriarchy and gender-based violence and the implications these have on HIV. She says, “The challenge is that women don’t have the power to decide […,] the use of condoms becomes a choice for men and not for the person who wants to protect themselves. And of course we know that forced sex is a problem.”
One group that is particularly at risk and vulnerable to this is sex workers. Men are the majority of clients in the sex industry and sometimes pay more for not using a condom. “Sex workers are often not able to negotiate to practise safer sex and even when they get raped they aren’t able to report these cases,” says Duduzile from Sisonke. “It puts sex workers at high risk.”
What are the solutions?
It is clear that business as usual is not working – urgent action is needed on two fronts. The first is challenging and transforming harmful gender and social norms that discourage men from seeking health services, and behaviours – such as violence and not using condoms – that increase the likelihood of HIV transmission to women and girls. Kganakga suggests, “We need to support boys from a younger age. We are not going to deal with the issues of gender-based violence if we leave the boys behind. They need to be nurtured the same way that we nurture the girls, so that they grow up being responsible young adults, responsible husbands, and so that they can look after the very women that we are preparing.” As peers are more likely to be listened to, peer support and discussion groups are an effective way of changing these gender norms.
The second is to ensure that health systems in general, and health service delivery specifically, are designed in a way that will meet men where they are with HIV-related services. To do this, the question needs to be changed from “how do we get men to come to HIV services” to “how to we take HIV-services to men”. One such example of this is Tsima, a randomised control trial in Bushbuckridge in rural Mpumalanga implemented by Sonke Gender Justice, University of North Carolina at Chapel Hill, the University of Witwatersand and the University of California, San Francisco, which aims to test whether community mobilisation can increase use of treatment as prevention.
According to Rebombo, “In the past few weeks we have decided to take HIV testing services to men, 22 men tested out of the 90 that we have recruited in two and a half weeks… whereas, for the past two years, we have been talking to the same men and asking them to go to a public health facility and they didn’t.”
HIV testing needs to be taken to men in the places they tend to congregate such as their workplaces, sports places and drinking places. The best place to reach men will vary from place to place and the local community should be involved from the beginning, says Karim. “People who live in the community will be best placed to tell you where to find men and reach them.”
Simply providing HIV testing is not sufficient. It is important also to build upon other prevention programmes that are taking place, in particular voluntary medical male circumcision (VMMC). “VMMC… presents an opportunity for governments, countries and communities to respond better to HIV,” says Obrian Nyamucherera, an academic focusing on expanding research on VMMC. This is because, if run well, a VMMC programme provides a unique opportunity to engage with men with a broad range of HIV prevention issues all at the same time, such as HIV testing, and education and changing harmful norms and attitudes around condom use, gender-based violence and health-seeking behaviour.
For Simphiwe, attending a support group and being able to get together with other men to talk about these issues and support each other made the difference in coming to terms with living with HIV. This led to acceptance and overcame the self-imposed stigma and shame of living with HIV. “For me what was so important about it was the fact that I accepted that I’m HIV positive,” says Simphiwe. If only the millions of other men who are living with HIV in eastern and southern Africa who don’t know their HIV status would be able to say the same. Then we would begin seeing real successes in preventing HIV both among men and also women, especially young women and girls.
Fortunately, a new initiative spearheaded by UNAIDS, Sonke Gender Justice and the International Planned Parenthood Federation provides room for optimism. Together they launched the Global Platform for Action on Men and HIV and are now rolling this out across some of the most affected countries in Africa. The Platform for Action provides ministries of health and national AIDS councils with vital tools, information and technical support to develop policies and programmes to engage men better, including to advance gender equality and to get HIV services to men and women in communities and workplaces across the region. A range of United Nations agencies have now committed to implementing the platform for action and many countries across the region are beginning to commission studies and policy reviews as an important step towards full implementation of the platform.
Hopefully, men like Simphiwe will soon begin to receive the services they need. DM
Jonathan Hopkins and Dean Peacock represent Sonke Gender Justice
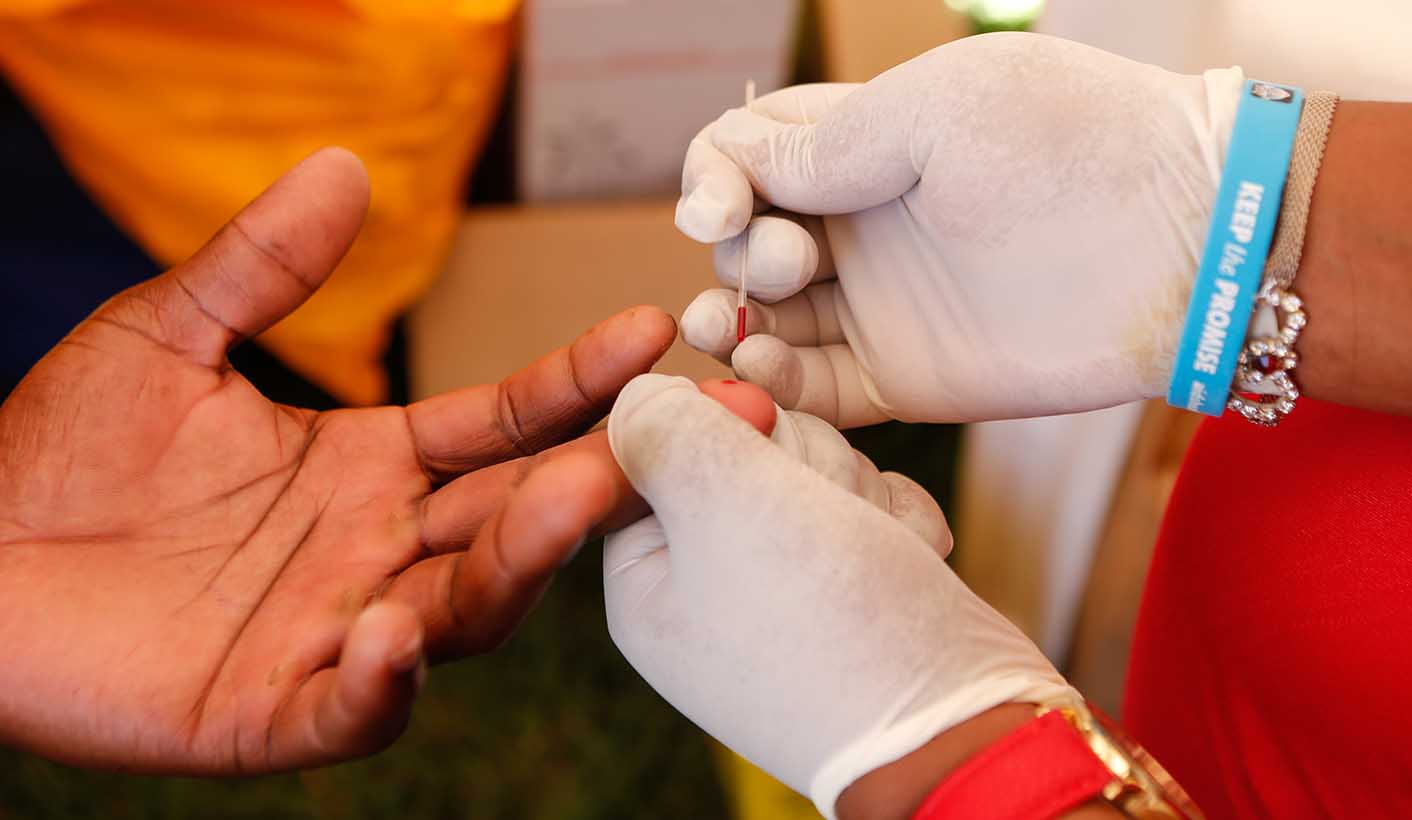
Photo: A man gets his blood taken for HIV testing at a free testing booth during an event organised by Kenya’s National AIDS Control Council and other organisations to mark World AIDS Day at the University of Nairobi in Nairobi, Kenya, 01 December 2017. EPA-EFE/DANIEL IRUNGU