Maverick Life, South Africa
Saving lives: South Africa joins paired kidney exchange revolution
On March 6, 2015, South Africa’s first kidney exchange took place at the Donald Gordon Medical Centre in Johannesburg. After having been kept alive by dialysis for years, 24-year-old Vivek* and 60-year-old Allison Stevenson were both given a new lease on life. By ANDREA TEAGLE.
Allison Stevenson was one of roughly 1,000 South Africans on the waiting list for a kidney. Every second day, she would travel to a clinic so that, for four hours, a dialysis machine could do the job her failed kidneys couldn’t.
Then, in late August 2014, Sally Seccombe – a childhood friend of Stevenson’s daughter – came forward as a donor, determined to save Stevenson’s life. Unable to give her kidney to Stevenson due to blood incompatibility, Seccombe instead agreed to donate to another recipient with whom she matched: 24-year-old Vivek. Meanwhile, Vivek’s intended donor proved a match for Stevenson. Six months after Seccombe volunteered one of her kidneys to save Stevenson’s life, Stevenson woke up in a hospital bed with a working kidney.
This was South Africa’s first paired kidney exchange. And it happened almost by chance.
“This youngster in Port Elizabeth – his mother was so anxious about him, she phoned the transplant centre in Johannesburg … It was like the next week that I phoned up.” Stevenson recalls, “And there, Belinda (a transplant coordinator), had this file on her desk, where the aunt didn’t match the nephew. It just so happened that she matched me, and Sally matched Vivek.”
Stevenson counts herself as extraordinarily lucky. “It really has been life-changing,” she says, adding that Seccombe who, through the exchange, is still considered her donor, is “one in 10-million.”
South Africa relies primarily on deceased kidney donations. Of the 4,300 people on the waiting list for life saving, most are waiting for a kidney. There is only a small hope of getting one: just 0.2% of the population are registered as organ donors. And a host of medical requirements need to be satisfied for a match. The waiting list is like a mile long tightrope to life and many people never make it across.
The problem is not merely a shortage of supply from deceased donors.
It is not uncommon for a healthy person to volunteer to donate a kidney to a family member or friend who needs it, as was the case with Seccombe. Kidneys are, after all, a special case amongst organs. We’re born with two. We need only one. More than half the time, though, a donor will not match the intended recipient. The demand is there, the supply is there, but there is a deadly, biological incompatibility gulf in between.
This is an example of what economists call a mismatched market. And for at least one economist, Stanford Professor Alvin Roth, it posed an exciting challenge. Roth and his colleagues were able to apply a model to the problem they had initially built out of mathematical curiosity. In 2012, this work won him a joint Nobel Prize in Economics.
Roth’s matching program builds little bridges between supply and demand. The simplest case is a two-way exchange like Stevenson’s. By decoupling the donors from their intended (but incompatible) recipients, and recoupling them with compatible ones, long chains of transplants can take place that otherwise would have been impossible. Most of the donors in a chain agree to donate contingent on their intended recipient receiving a kidney from someone else. It is thus imperative that each donor follows through with her commitment; otherwise, the chain collapses.
To date, the longest donor chain is a 68-person chain completed in the US in April 2015 that saved 34 lives. Chain exchanges are typically “unlocked” by altruistic donors: people who have decided to donate kidneys to strangers.
Although the idea of kidney exchanges is simple, the maths behind it is enormously complicated. The longer the chain, the more complicated it becomes. The software must pit patient data against potentially thousands of living donors, rank matches according to their chances of success, and at the same time ensure that as many people are matched as possible. Some recipients – for example, those with universal blood type AB – will likely match with many donors; others will have a much slimmer chance of finding a match. When the donor pool is the entire national registry, the odds of matching are exponentially improved.
In South Africa this type of optimised matching is but a dream.
The National Health Act allows for living donors to donate to a blood relative or a spouse. If the donor is not a relative, he or she must apply for special permission from the Department of Health. In South Africa – as in every other country in the world with the exception of Iran – the sale of organs is illegal.
The hesitancy to implement paired matching, although the law does not in fact prohibit it, is likely partly due to fear of abuses through monetary exchange. (It is, however, lawful for the donor to be reimbursed for “reasonable costs” associated with the transplant.)
However, Stevenson’s case shows that paired exchanges can be subjected to the same careful scrutiny as direct donations. Only after establishing that neither donor had been coerced, misled or financially incentivised, did the Department of Health give the go-ahead. Further, the pairs were not allowed to meet or communicate prior to the operation, so Stevenson has never met her actual donor.
Belinda Rossi, one of the transplant coordinators at Donald Gordon, says of the exchange: “It was really the test case to see how the Department of Health would react to it.”
Four months later, all four of the donors and recipients involved have healthy, functioning kidneys.
The successful matching is an important step towards overcoming what surgeon Francis Delmonico, who was involved in the original matching program in the US, described as “the frustration of a biological obstacle to transplantation”. However, without a registry of living donors, finding a paired match will require hours of effort, and many will not be as lucky as Stevenson.
In the US, matching through the countrywide Kidney Paired Donation program takes between a month and two years. It is estimated that 1000-2000 additional kidney transplants can be performed annually through the program – which can be run on a single desktop computer.
Meanwhile, in South Africa, there may be hundreds of potential donors unable to donate, and patients desperate for kidneys who will die waiting. At the same time, the cost of dialysis for those on the waiting list puts strain on an already overburdened healthcare system. Patients with renal failure require dialysis two or three times a week just to stay alive. Limited resources mean not everybody can receive treatment: only about a third of South Africans who need it are receiving hemodialysis, a type of dialysis used to treat advanced renal failure.
Doctors are faced with the burden of telling patients that although there is a treatment that could save their lives, they cannot have it. A kidney exchange program would result in a shorter waiting list for kidneys, freeing up space at public hospitals for patients who need dialysis.
Of course, setting up a donor exchange database with enough donor information brings about its own costs and challenges. However, moving in this direction is surely less costly to the state than the current, apparently unmanageable, burden of dialysis and the years of lost productivity while patients wait for kidneys that may never come.
The constitution requires that the government take reasonable steps to realise the right to healthcare. Hopefully, for those with renal failure, South Africa’s landmark two-way exchange will be the first step in removing some of the current barriers to that right. DM
* not his real name.
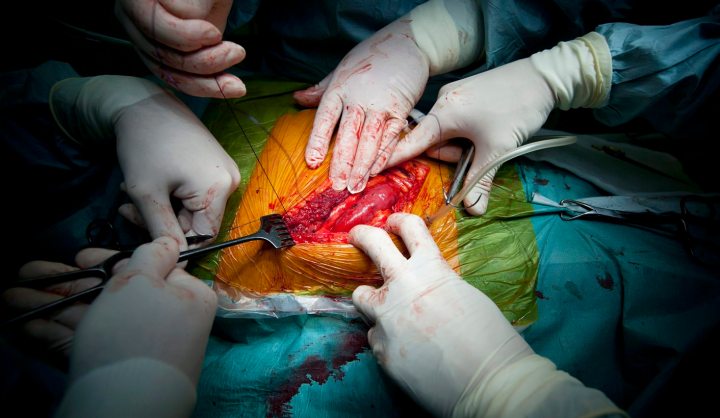
Photo: A picture made available on 01 December 2011 shows surgeons closing the wound as they complete a live donor kidney transplant operation at the transplantation clinic of the Semmelweis University Hospital in Budapest, Hungary, 30 November 2011. The kidney was donated by the patient’s wife. On 01 January 2012, Hungary joins Eurotransplant, an international non-profit organisation coordinating organ transplants and donors in its member countries. EPA/BALAZS MOHAI.



















 Become an Insider
Become an Insider