Several African countries — including Botswana, Eswatini, Rwanda, Tanzania and Zimbabwe — are close to ensuring that 95% of their populations living with HIV know their HIV status, 95% of persons familiar with their HIV status are on treatment and 95% of the people on treatment are virally suppressed by 2025 — the “95-95-95” target.
That’s according to UNAids Executive Director, Winnie Byanyima, who was speaking during the roundtable discussion for the launch of UNAids’ Global Aids Update 2023 and report, The Path That Ends Aids, at the Palais des Nations in Geneva, in Switzerland last Thursday.
Those five African countries are in addition to 16 other countries said to be “on the path” to attain the “95-95-95” targets for 2025 and to “end Aids as a public health threat” by 2030, according to Byanyima. The 16 countries include eight in sub-Saharan Africa, a region with 65% of the 39 million people living with HIV across the globe.
/file/dailymaverick/wp-content/uploads/2023/07/MC-UNAIDS-Update.jpg)
Those targets present a “possible dream that is not possible” with the current set of challenges, said Sibongile Tshabalala, national chairperson of the Treatment Action Campaign (TAC), South Africa’s leading HIV/Aids activist organisation.
Tshabalala expressed concern about governments who are redirecting funding from HIV programmes to other health responsibilities; healthcare systems’ discriminatory behaviour towards those living with HIV; the slow uptake of PrEP (pre-exposure prophylaxis), and the high levels of infections among females between the ages of 14 to 24 in South Africa.
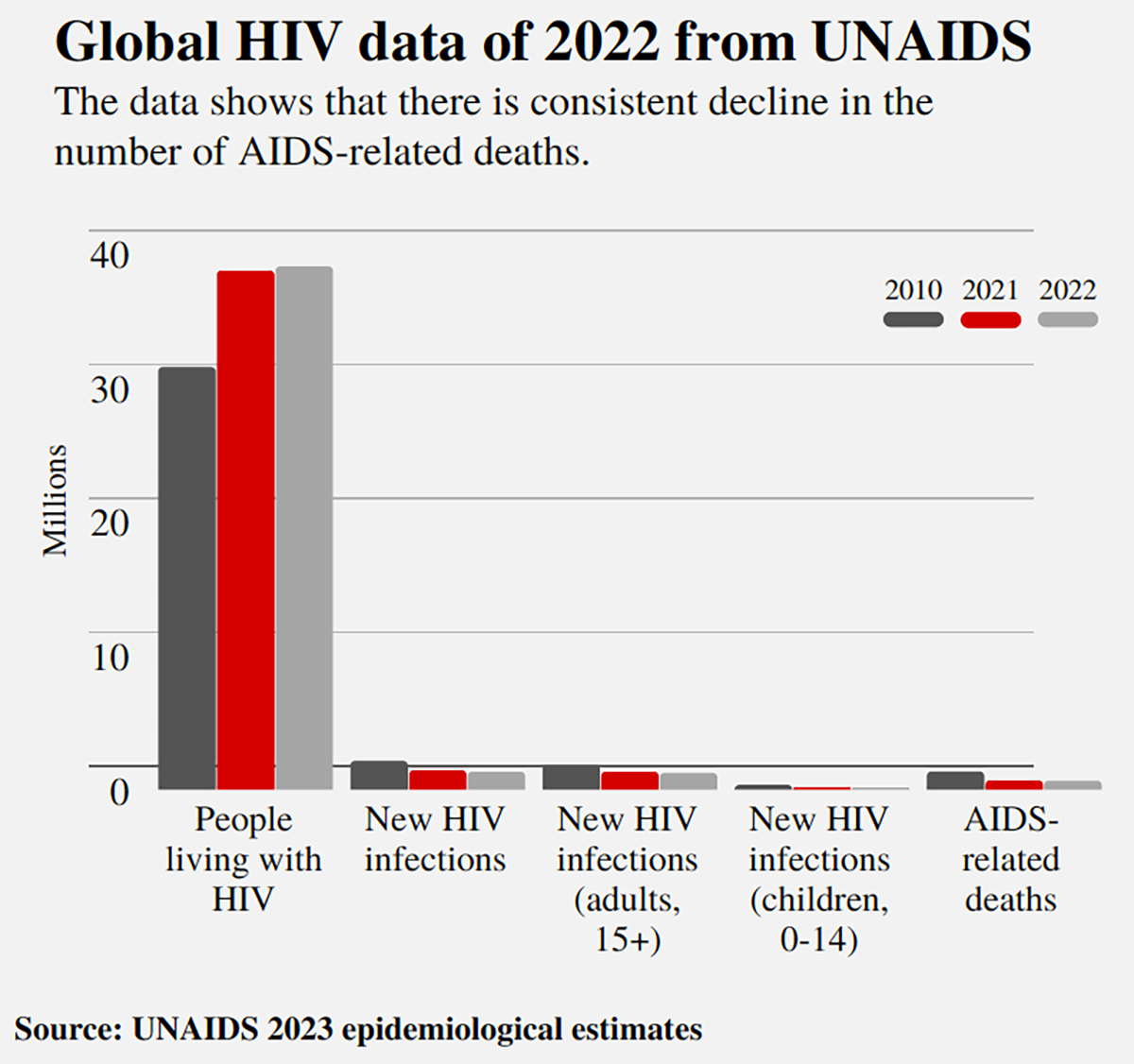
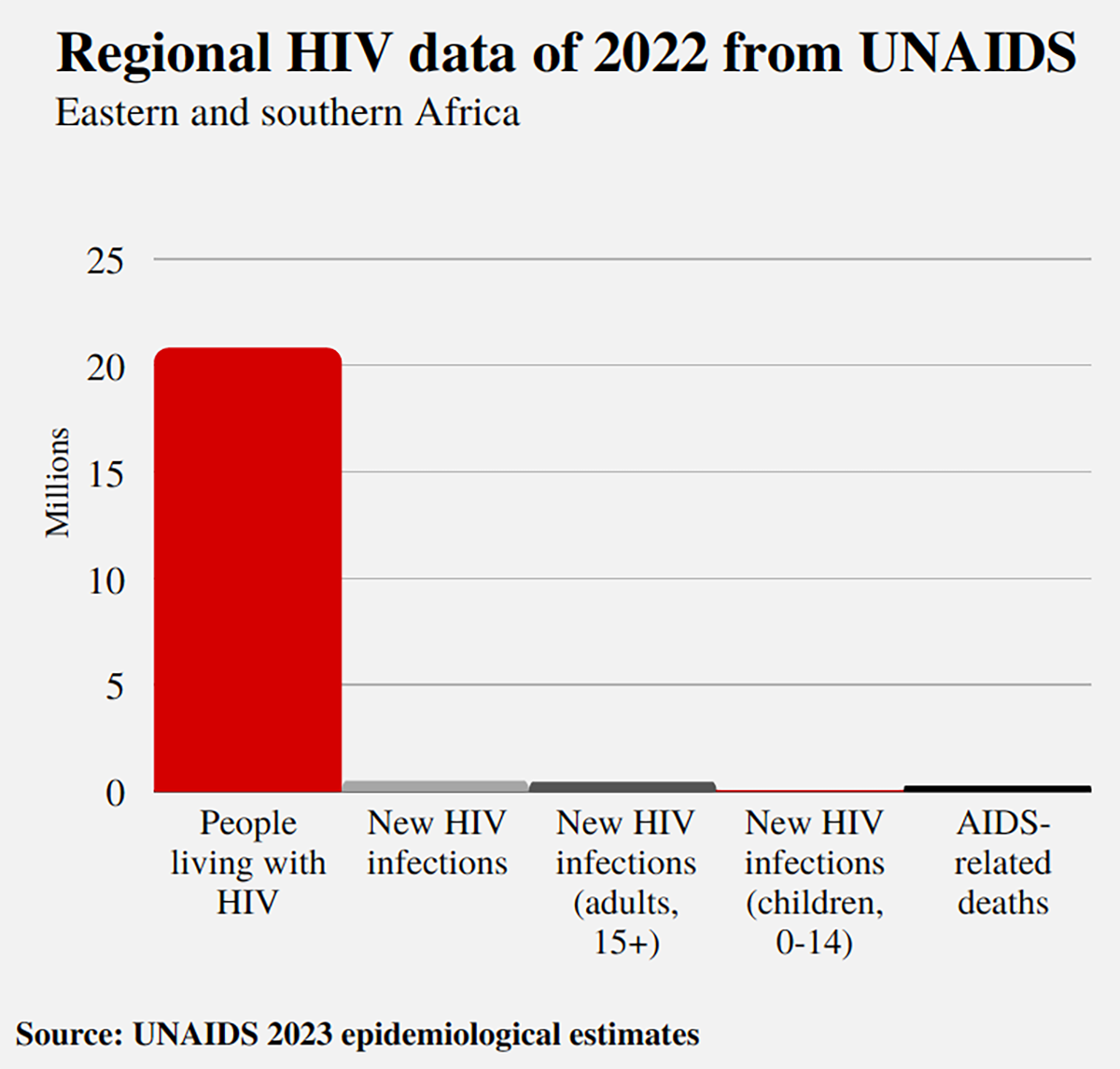
Significant progress, according to UNAids, can be found in countries with the most financial investments in HIV prevention and care. Those include countries in east and southern Africa which have witnessed a 57% decrease in infection from 2010. UNAids, however, remains concerned that globally about 9.2 million people are not on treatment, including 660,000 children living with HIV.
Also, progress is threatened by human rights violations evident in homophobic laws being adopted by several African countries such as Uganda, said Tshabalala. These laws encourage mistreatment of members of the LGBTQIA+ community, limiting their access to healthcare services and resources necessary for the prevention or treatment of HIV.
Read more in Daily Maverick: Death penalty imposed as Uganda passes law making it a crime to identify as LGBTQ
“I think this report did not dig deeper on what is really happening on the ground. They just spoke about the reports that are brought forward by the governments and scientists. The reality on the ground has not been really captured,” said Tshabalala.
Path to take
To get on the path to the 95-95-95 targets, four key issues need to guide the HIV response and form part of a strong political leadership because “when leaders ignore, isolate and criminalise people living with or at risk of HIV, progress in the Aids response is obstructed,” says UNAids in its statement.
Firstly, the decision-making processes needs to be based on data, science, and evidence; and secondly, they need to be coupled with measures to address inequalities that create vulnerable groups. The third and last issues are for leadership to enable “communities and civil society organisations in their vital role in the [HIV] response” and to ensure “sufficient and sustainable funding,” the statement adds.
Those priorities provide broad areas of focus to address prevailing challenges related to the transmission, testing, and treatment of HIV within specific contexts.
According to researchers, in South Africa’s context of an estimated 8.2 million people living with HIV in 2021, the prevailing challenges are still said to be a delay in treatment initiation and the lack of significant behaviour change evident through risky behaviours.
Risky behaviours include early sexual debuts and having a sexual partner who is five or more years older or younger, as well as having multiple sexual partnerships, which entails engaging with more than one sexual partner over a 12-month period.
The suggested solutions are targeted intervention programmes for more youth to test, gain access to antiretroviral treatment and to be better informed about the risky behaviours that carry a higher risk of HIV infection. DM




 A spaza shop outside the front entrance of the Ravensmead Clinic, Parow, Cape Town, on 2 December 2022. Food security is under threat and a lack of adequate nutrition poses particular risks for HIV patients needing to take antiretroviral (ARV) medication. (Photo: David Harrison)
A spaza shop outside the front entrance of the Ravensmead Clinic, Parow, Cape Town, on 2 December 2022. Food security is under threat and a lack of adequate nutrition poses particular risks for HIV patients needing to take antiretroviral (ARV) medication. (Photo: David Harrison)