Between April 2022 and March 2023, 17 under-fives died from moderate acute malnutrition and 98 children succumbed to severe acute malnutrition. These numbers refer only to deaths in health facilities.
Meanwhile, a third-quarter performance report tabled in the Free State legislature in March showed that six out of 37 patients (children under five years) admitted to tertiary hospitals in the Free State for severe acute malnutrition had died. “Included in the deaths were severe acute malnutrition with oedema, severe acute malnutrition admitted with diarrhoea, and severe acute malnutrition with congenital cyanotic heart lesion as well as pulmonary HPT,” the report states.
The health department had missed several of its targets set to address malnutrition in the province in the third quarter of the 2022/23 financial year. In 2022, Spotlight reported that there was an increase in deaths of children under five – mostly due to severe acute malnutrition from 2020/21 to 2021/22. Mvambi told Spotlight at the time: “Of all the children admitted to the province’s hospitals for acute malnutrition, 48 died in 2020/21 and 86 in 2021/22.”
Additionally, results from a survey by the Grow Great Campaign – an organisation committed to reducing the number of children suffering from stunting – released last month showed that two out of every 10 children in the Free State’s Thabo Mofutsanyana District suffer from stunting.
/file/dailymaverick/wp-content/uploads/2023/07/MC-Spotlight-stunting-malnutrition-2.jpeg)
Dr Chantell Witten, dietitian and researcher in the Community Paediatrics Division at the University of the Witwatersrand, called this and the number of children with malnutrition a national crisis. She says often stunting is an indicator of chronic malnutrition.
The survey results were released last month at an imbizo on stunting in Bethlehem held by the Grow Great Campaign.
According to Professor Corina Walsh, who specialises in nutrition and dietetics at the University of the Free State, malnutrition takes many forms, including underweight (low weight for age), stunting (low height for age), wasting (low weight for height) and hidden hunger (micronutrient deficiencies). Wasting is an indicator of recent severe malnutrition and is referred to as severe acute malnutrition, while stunting is an indicator of long-term chronic malnutrition.
Dying of hunger
The Grow Great findings come as no surprise, as the provincial health department itself has expressed concern over an increase in the number of under-fives with severe acute malnutrition.
The campaign survey looked at children under five years from 455 households in the Thabo Mofutsanyana District. It found that 17% of the surveyed children suffer from stunting. This is a rural district with a population of about 700,000, where 52% live below the lower poverty line while 32% are unemployed.
Mothers start giving formula to babies right from the start while they are in our facilities. I have witnessed this even in facilities that are said to be child-friendly.
Grow Great also found that 15% of surveyed children are obese, 3% are underweight, 6% are wasted and 1% have acute malnutrition.
Thirteen percent had a low birth weight (under 2.5kg), 62% had vitamin A supplements on track, 61% had deworming on track, 39% had adequate dietary diversity, and 65% were exclusively breastfed. Only 27% had access to early learning centres and 84% relied on child support grants.
/file/dailymaverick/wp-content/uploads/2023/07/MC-Spotlight-stunting-malnutrition-3.jpeg)
Small reflection of the burden
When asked if the survey results are a true reflection of what is happening in the district, the Thabo Mofutsanyana District nutrition manager for the Department of Health, Dineo Mopeli, says the survey results are just a small reflection of how much the district is burdened with acute malnutrition.
“I wish I knew about this survey earlier,” she says. “When looking at the results… I would say 1% is suffering from severe acute malnutrition and 6% from moderate acute malnutrition. This is the picture that we have, but remember, we conduct surveys differently. As the department, we measure what is coming to the clinic, so there is a possibility that our statistics will differ. But the facts are: we do have a high rate of severe acute malnutrition and the infant deaths are high, especially during the times of Covid-19 and now.”
Read more in Daily Maverick: Malnutrition and hunger take hold in SA – a land of plenty where political will is lacking
Mopeli also worries about the low numbers for access to early learning centres. “I was not aware that it was so low. My other issue is the exclusive breastfeeding rate. In my view, this is not a true reflection. Children who are exclusively breastfed are definitely lower than that. Mothers start giving formula to babies right from the start while they are in our facilities. I have witnessed this even in facilities that are said to be child-friendly. But we are going to correct that as the department. Exclusive breastfeeding numbers must at least stand at 80%.”
Reflections on the ground
“Daily I deal with a child that is suffering from malnutrition,” says Majabulile Mapoteng, a professional nurse who specialises in child health and who works at Mphohadi Clinic in Bethlehem.
/file/dailymaverick/wp-content/uploads/2023/07/MC-Spotlight-stunting-malnutrition-4.jpeg)
“As nurses, we try our best to avoid children dying of acute malnutrition, so we help to the best of our ability. We see about 30 children under five years per day at our clinic and from the total number I will get [about] five children who are either underweight or too short for their age. When we come across this kind of problem, we help the mothers at clinic level by referring them to a dietitian in order for them to receive education on the types of nutritious food a child needs to eat. We also give them a nutritional supplement of soft porridge such as Jikelele, which helps in giving the child the nutritional support they need, and if the child is still an infant we give them baby formula.”
Addressing malnutrition requires a multidimensional approach that considers social and economic factors and improvements in healthcare and education.
Spotlight also spoke to a community healthcare worker in Bethlehem, Nthabeleng Moloi, who is based at the Bakenpark Clinic. She too says there is a serious problem with malnutrition in the community. Moloi says her responsibility is to ensure that the well-being of children who are suffering from malnutrition comes first. She says that in her seven years as a community healthcare worker she has seen many children who are suffering from malnutrition in the community.
“We receive the names of these children from the clinic. Then we visit their homes. When we get there we connect them with the hospital dietitian and if the situation is very bad at home, we coordinate with a social worker who will ensure that the family receives food parcels. I will then have to visit the home very often until the child is healthy again,” says Moloi.
/file/dailymaverick/wp-content/uploads/2023/07/MC-Spotlight-stunting-malnutrition-5.jpeg)
Numbers increasing
When Spotlight spoke to Mvambi about the survey results, he said the department found that the recorded number of children suffering from malnutrition in the province increased by 470 from 3,284 to 3,754 between April 2022 and April 2023.
According to Mvambi, the department continues to run educational programmes for pregnant mothers, encouraging them to follow exclusive breastfeeding for up to six months. “We also encourage mothers to familiarise themselves with the road-to-health booklet they receive upon the birth of children.”
Read more in Daily Maverick: How a child’s body responds to hunger — and the lifelong consequences of malnutrition
But Witten says the underlying causes of malnutrition are the high levels of poverty and the high rate of unemployment. “This means that many households in the district depend on a child support grant and the old age pension grant. The Free State has more than 700,000 beneficiaries of the child support grant, which was increased from R480 in 2022 to R500 this year. “We all know that the child support grant is not sufficient to buy good-quality food for children.”
A national crisis
Witten points out that nationally 27% of children are thought to be stunted, according to Statistics South Africa. The numbers from the Thabo Mofutsanyana District are lower than that, but still high.
“The low birth weight is in line with the national statistics of 15%. We are not surprised by the high levels of malnutrition in South Africa, also in the Free State, because it is a rural province where many of the households are paid below the poverty line. We know that many families have sent their working members to work in provinces such as Gauteng and children are taken care of by old members who also need to be taken care of themselves. So, this is a complex problem for the Free State and, more particularly, it is a national crisis. So, child health and child nutrition are in a crisis,” Witten says.
She says that researchers involved in the annual Child Gauge, a publication of the University of Cape Town, made several recommendations to address the child nutrition crisis. “Among these were for a subsidised food basket or micro policy interventions where we control the prices of important products for children such as eggs, full-cream milk, soya products and VAT-free meat products, especially for children who are receiving the child support grant.”
/file/dailymaverick/wp-content/uploads/2023/07/MC-Spotlight-stunting-malnutrition-6.jpeg)
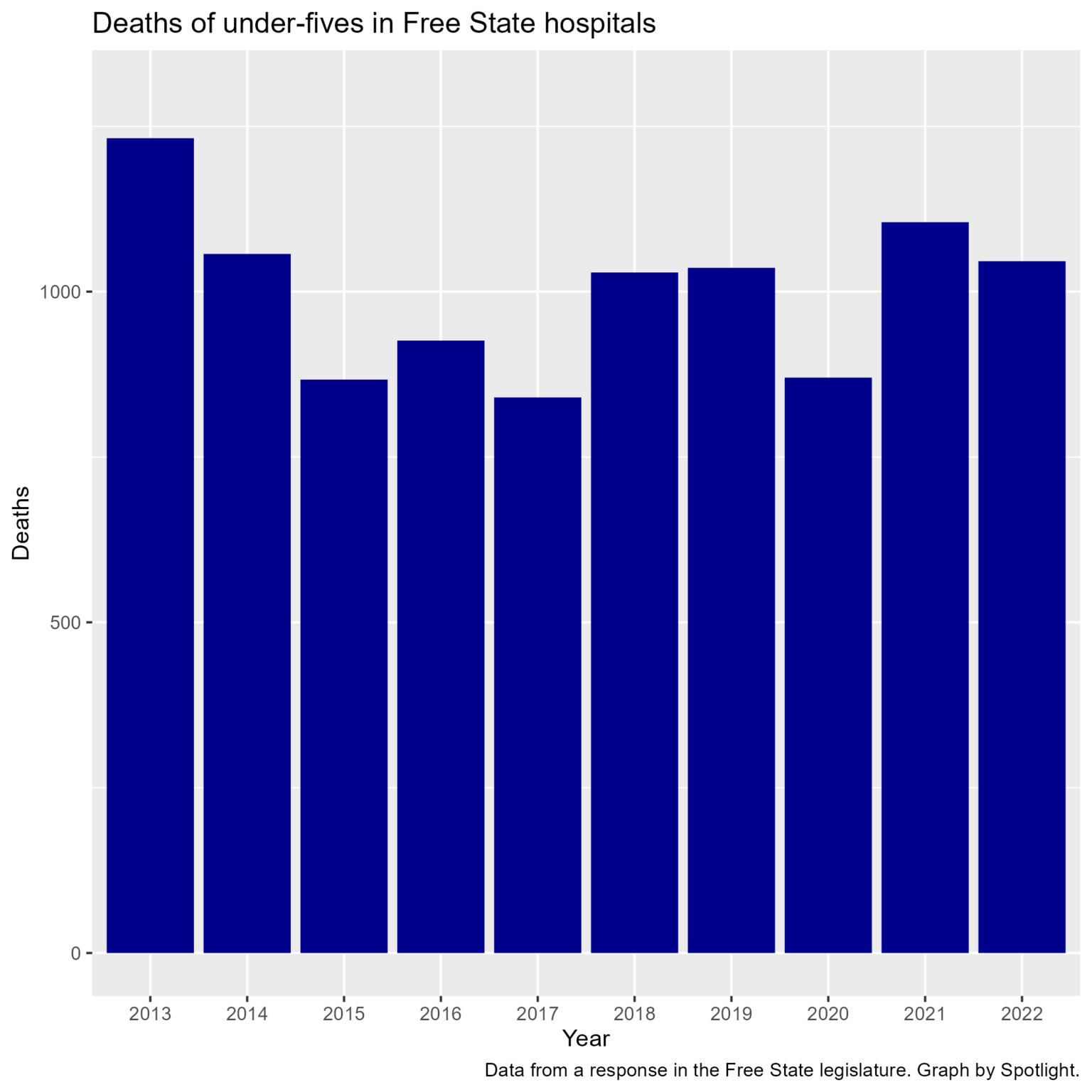
In response to a question in the provincial legislature about under-five deaths in health facilities, by DA MPL and health spokesperson in the Free State Mariette Pittaway, numbers provided by health MEC Mmathabo Leeto showed that more than 10,000 children had died in health facilities from 2013 to 2022. These deaths had been due to acute malnutrition, pneumonia, diarrhoea and preterm birth complications.
“Malnutrition in children in the province is a severe problem and limited access to adequate healthcare such as prenatal and paediatric care, and poor water and sanitation infrastructure makes it very difficult for poor households to meet basic needs,” Pittaway says. “Addressing malnutrition requires a multidimensional approach that considers social and economic factors and improvements in healthcare and education.”
Reasons and planned interventions
There are several interventions listed in the department’s third-quarter report to address the severe acute malnutrition in-facility fatality rate, and explanations for why the department could not reach the targets it set itself.
In tertiary hospitals, for example, the department says these deaths were recorded due “to late referral from lower levels of care”, and “some children were critically ill and had other medical conditions”. The plan is to, among other things, “strengthen early detection and referral to high levels of care” and to persist with “continuous health education and promotion as a preventative measure”.
In regional hospitals, however, which also missed the target for the severe acute malnutrition fatality rate, the department lays the blame at the door of caregivers who “delay seeking healthcare”. Other reasons for missed targets included late referrals from lower levels of care and that mobile services often cannot reach some areas due to poor road infrastructure. The plan, says the department, is to “improve outreach services with social workers and dieticians”, and to have health promotion in communities on the “early danger signs and detection of malnutrition”, and to “advocate for caregivers to present earlier at health facilities for medical intervention”.
/file/dailymaverick/wp-content/uploads/2023/07/MC-Spotlight-stunting-malnutrition-8.jpeg)
The department performed poorest on targets set for district hospitals. The target set for the under-five severe acute malnutrition case fatality rate was 1.8% but the recorded rate was 8%. Among the reasons it gave for this are “poor feeding practices by caregivers” and “a delay by clinicians to do growth monitoring and management of growth faltering children”.
To address this, the department reported that it will train community healthcare workers to identify vulnerable children early and refer them to care timeously. It says it will also provide nutrition supplements and strengthen infant and young-child feeding. Another element of this plan is to work with other government departments in the social services cluster on the challenges of malnutrition and to advocate for support in addressing the social determinants of health.
Meanwhile, in an effort to improve child nutrition, the Flourish social programme initiated by the Grow Great Campaign offers support to vulnerable pregnant women through pre- and post-natal classes to encourage mothers to breastfeed their children exclusively for six months.
Read more in Daily Maverick: Chantell Witten: A champion for breastfeeding and early childhood nutrition
The organisation’s programme coach in the Free State, Dithoriso Mphuthi, says Flourish currently has franchises in two small towns in the province – Soutpan and Dealesville. “We have classes once a week at our branches where we see about 10 mothers each day for free. We empower pregnant women and ensure that they exclusively breastfeed their babies. We believe that it is important for babies to be breastfed to reduce malnutrition by 2030.”
This article was published by Spotlight – health journalism in the public interest.





 From April to June 2023, 21 children in the Free State died of severe acute malnutrition. (Photo: Black Star / Spotlight)
From April to June 2023, 21 children in the Free State died of severe acute malnutrition. (Photo: Black Star / Spotlight)