The Singapore government has to date covered the full costs of medical treatment of Covid-19 patients, in order “to avoid financial considerations adding to public uncertainty and concern when Covid-19 was an emergent and unfamiliar disease”.
However, the government has announced that from 8 December 2021 those who are “unvaccinated by choice” will have to start paying for their own Covid-19 treatment on the grounds that “unvaccinated persons make up a sizeable majority of those who require intensive inpatient care, and disproportionately contribute to the strain on our healthcare resources.”
Why should it be considered for South Africa?
While Covid-19 infection rates in South Africa are currently low, Minister of Health Dr Joe Phaahla has warned of a fourth wave starting in December and urged people to take the vaccine, describing this as the only hope of long-term success in containing the Coronavirus. The Department of Health has set a target of vaccinating at least 70–90% of the adult population (18 and over) by December.
However, by 13 November only 13.4 million (33.5%) of the total target population of 39.8-million adults had been vaccinated. South Africa has the capacity to vaccinate more than 300,000 people a day but daily vaccination rates have fallen well below targets. Besides the immediate health care concerns, the low vaccination rates raise broader economic concerns for the country. As Finance Minister Enoch Godongwana highlighted in his Medium-Term Budget Policy Statement, “getting more South Africans vaccinated would put the country in a better position to respond effectively to the economic impact brought about by the pandemic.”
Various approaches to increasing the vaccination rate are being considered with mandatory vaccination featuring prominently. Business for South Africa has argued that “in our view, a combination of mandatory vaccination policies, as well as incentives, are going to be necessary alongside the demand generation communications and mobilisation campaign to get as many people as possible vaccinated.”
The Department of Public Service and Administration (DPSA), is also considering mandatory vaccinations for government workers. The Department of Employment and Labour has published a directive that will allow businesses to introduce mandatory vaccinations, subject to certain requirements.
However, there are concerns about the legislative basis for mandatory vaccination and the legal firm Webber Wentzel has concluded that “there is currently no legislation that requires all South African citizens to be vaccinated and that vaccination is still a choice and is not mandatory.”
There are also concerns that vaccine mandates by employers will have relatively little impact in a country with an official unemployment rate of more than 34%, where many depend on informal work for their livelihoods.
Given the low vaccination rates and concerns about mandatory vaccination, should South Africa consider the Singaporean approach of not covering the medical costs of unvaccinated Covid-19 patients in order to encourage vaccination take-up and at the same time internalise the cost of non-vaccination?
The Singaporean approach requires those “unvaccinated by choice” to pay for their own Covid-19 treatment. Three key questions need to be addressed in considering whether the approach is suitable for the South African context: (1) What is the evidence demonstrating that full vaccination reduces the risk of Covid-19 related morbidity and treatment requirements? (2) With what level of certainty can we distinguish between those “unvaccinated by choice” and those “unvaccinated by circumstance”; and (3) is the case for making the “unvaccinated by choice” pay for their own treatment fair and justifiable?
There is a growing body of evidence confirming that full vaccination significantly reduces the risk of Covid-19 related morbidity and consequently of treatment requirements. For instance, a large Centers for Disease Control and Prevention study in the US showed vaccines to be 84% to 96% effective in preventing Covid-19 related hospitalisation. A similar picture emerges from trends in the United Kingdom.
Locally, Discovery Health, South Africa’s largest medical scheme, has reported that the Pfizer vaccine is 92% effective in reducing the risk of hospital admission for Covid-19 and 94% effective in preventing the risk of Covid-19 death. Of 156 Covid-19 patients admitted to Groote Schuur Hospital on 6 September 2021, 153 (98%) were not vaccinated, and none of the 66 patients requiring ICU care or the 32 patients requiring ventilators on that day were vaccinated.
The second and third questions must be examined separately for those with and without private medical cover, considering the huge disparities between these groups.
For those without private cover, it is difficult to make a case for the Singaporean approach. Because of their socioeconomic profile, geographical distribution and other population characteristics, the risk of being “unvaccinated by circumstances” is high in this population and it would be difficult to identify with certainty those who are “unvaccinated by choice”. Implementing the Singaporean approach would therefore carry a high risk of unnecessarily and unfairly burdening those who are unvaccinated as a result of circumstances.
For the population with private cover, the case for adopting the Singaporean approach is much stronger. Based on the profile of the insured population, the accessibility of vaccines is less of an issue and the risk of being “unvaccinated by circumstances” consequently low. It would be reasonable to assume that the vast majority of the unvaccinated in this population, with some exceptions, are “unvaccinated by choice”.
The question is whether requiring them to pay for their Covid-19 related treatment is fair and justifiable. At the onset of the pandemic, the Council for Medical Schemes issued Circular 25 of 2020 declaring Covid-19 a Prescribed Minimum Benefit (PMB) condition, and requiring all medical schemes to fund all Covid-19 related costs for consultations, tests, medication, hospitalisation and rehabilitation in full. In terms of this regulation, medical schemes have to cover the costs regardless of vaccination status. Inherent in this arrangement is a substantial cross-subsidy from those who are vaccinated to those who are not vaccinated.
While cross-subsidisation by the healthy of the less healthy is a central social solidarity principle of all health insurances, it is questionable whether it is fair and justifiable to cross-subsidise people who knowingly chose to remain high risk, thus abandoning the broader social solidarity principle of protecting others from avoidable harm.
In summary, the Covid-19 vaccine substantially reduces the risk of Covid-19 related morbidity and treatment requirements. The case for implementing the Singaporean approach for the South African population without medical cover is weak as it carries a high risk of unnecessarily and unfairly burdening those who are unvaccinated as a result of circumstances. The case for implementing the approach for the population with medical cover is much stronger as there is a far higher probability that the unvaccinated in this group remain “unvaccinated by choice” and the burden of cross-subsidy burden on the vaccinated is unfair and not justifiable.
The Singaporean approach could be relatively easily implemented for this population by a review of the Covid-19 PMB. The Council for Medical Schemes could make an adjustment in terms of which the benefit is prescribed only for individuals who have been vaccinated. The change would mandate medical schemes to cover Covid-19 related costs of vaccinated individuals, but allow schemes discretion as to the level of cover provided for non-vaccinated individuals (as for any other non-prescribed benefit).
Those unvaccinated by choice would then be obliged to cover any shortfall in their medical costs. While such a measure may impact on a relatively small number of members, it would send a strong signal of government commitment to vaccination to achieve the levels necessary to protect the population. DM
Geetesh Solanki is Specialist Scientist at the Health Systems Research Unit, SA Medical Research Council (SAMRC); an Honorary Research Associate in the Health Economics Unit, University of Cape Town and Principal Consultant at NMG Consultants and Actuaries.
Vishal Brijlal is a Senior Director at the Clinton Health Access Initiative.
Reno Morar is the Chief Operating Officer, University of Cape Town.
Judith Cornell was the Director of Institutional Development and Planning (now retired) at the Nelson Mandela School of Public Governance, University of Cape Town, South Africa.
The opinions expressed are those of the authors and do not necessarily reflect the views of their institutions.




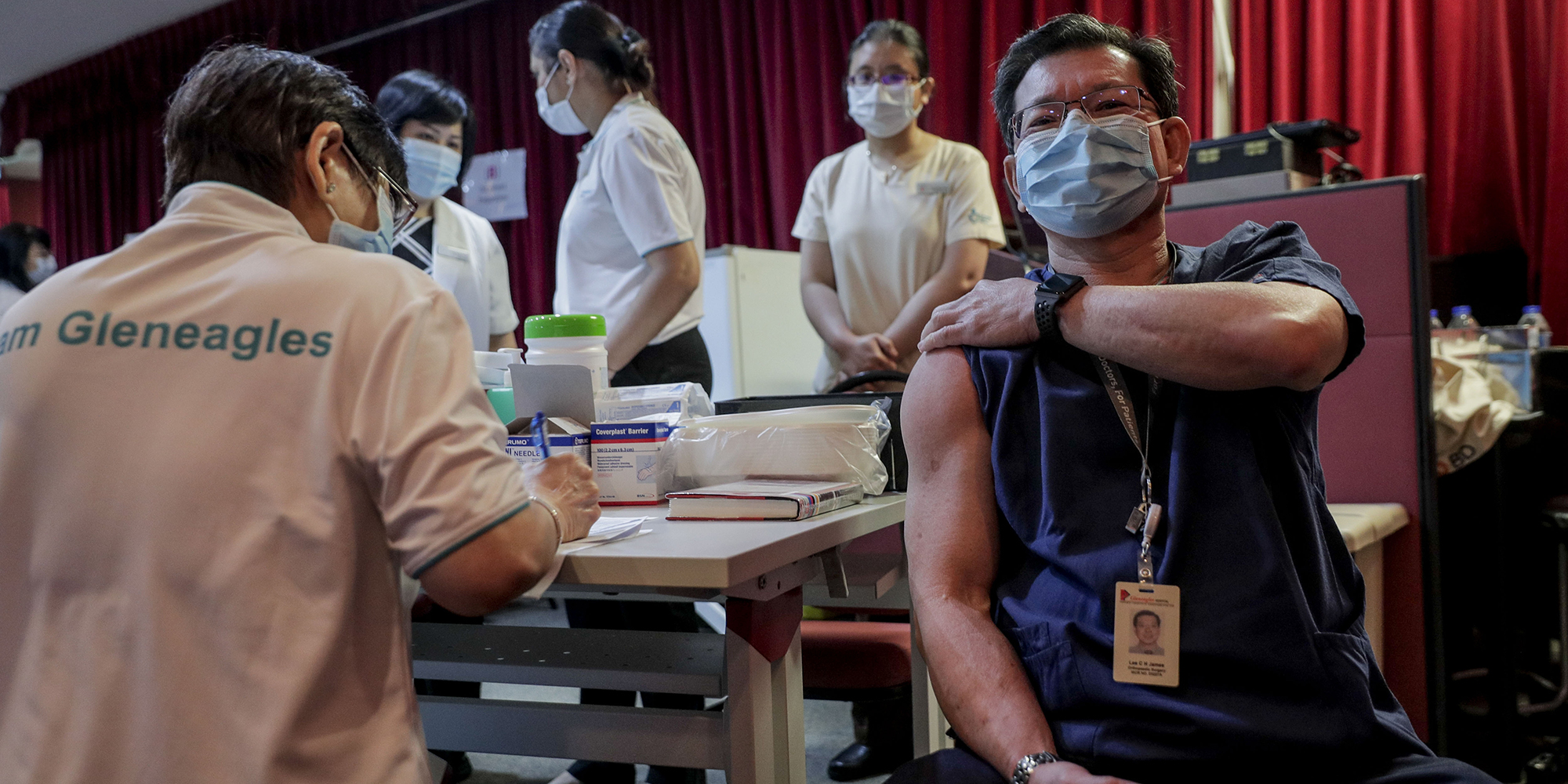 A healthcare worker (R) prepares to receive a dose of the Pfizer-BioNtech Covid-19 vaccine at a vaccination centre for healthcare workers in Singapore, 19 January 2021. The government of Singapore has said that from 8 December 2021 those who are ‘unvaccinated by choice’ will have to start paying for their own Covid-19 treatment. (Photo: EPA-EFE/WALLACE WOON)
A healthcare worker (R) prepares to receive a dose of the Pfizer-BioNtech Covid-19 vaccine at a vaccination centre for healthcare workers in Singapore, 19 January 2021. The government of Singapore has said that from 8 December 2021 those who are ‘unvaccinated by choice’ will have to start paying for their own Covid-19 treatment. (Photo: EPA-EFE/WALLACE WOON)