Anele Yawa is the General Secretary of the Treatment Action Campaign (TAC). Lotti Rutter is with Health GAP. Both work on the Ritshidze project.
The growing crisis in many of South Africa’s clinics has reached a point where patient care is being compromised. There is a deepening worry that people living with HIV are being pushed out of treatment.
Allowing people living with HIV to collect their medication refills outside of the clinic can improve this experience and reduce the risk of people disengaging from care. Decentralising medication refills — together with longer ARV refills — can reduce how often people living with HIV actually have to go to the clinic — reducing time spent in long queues, interacting with rude staff, or having their status involuntarily disclosed, as often reported through community-led monitoring, of the kind we do as part of the Ritshidze project.
“The staff – from the security guard to the clerks and even some of the nurses – they are not hungry for their jobs, you can see that. They shout at you, they leave the clinic to go buy magwinya (vetkoek) and cold drinks even when the queues are long and they take their time. They also lose our files and don’t care for our privacy.”
Repeat prescription collection strategies, as they are known in South Africa, can simplify and adapt HIV services in ways that both serve the needs of people living with HIV better and reduce unnecessary burdens on the health system. They should be much simpler and quicker systems than waiting in long clinic queues.
There are three different types of repeat prescription collection strategies, the availability of which varies across provinces. People living with HIV can use facility pick-up points such as a fast lane or parcel collection room at a clinic. They can use an external pick-up point, which varies from place to place, including collection through Clicks or Dischem or other venues in the community such as a Pelebox or locker with a code sent to their phone. Others may opt for an Adherence Club, which meets in a health facility or a community venue and offers additional peer support and treatment literacy education.
“There is always a high volume of people when I go there on Thursdays. And people are waiting outside and it’s dusty or cold. There are not enough chairs for everyone. They don’t have your file ready and it’s the security guard who takes our appointment cards and goes to find the files. And he is harsh, he screams at us and there’s no confidentiality — everyone knows you are there because you are HIV positive because he is shouting at us to stand in different queues.”
Of the 381 clinics monitored through Ritshidze, our data shows that the following options are available:
- 366 clinics reported offering facility pick-up points (CCMDD parcel collection room, pharmacy, fast lane, fast track, Sha’p Left, ARV ATM, Pelebox/locker with code sent to phone);
- 331 clinics reported offering external pick-up points (pharmacy e.g. Clicks or Dischem or independent pharmacist, community venue e.g. church/library/other, from a mobile van, Sha’p Left, ARV ATM, Pelebox/locker with code sent to phone, Post Office);
- 108 clinics reported offering adherence clubs in the facility; and
- 74 clinics reported offering adherence clubs in the community.
The graphs below provide a breakdown of the types of facility pick-up points and community pick-up points available by province through our monitoring. It is clear that the range of options needs to be expanded and made available nationally, not only in certain densely populated provinces like Gauteng.
/file/dailymaverick/wp-content/uploads/2021/05/MC-Oped-Lotti-Graph1_1.jpg)
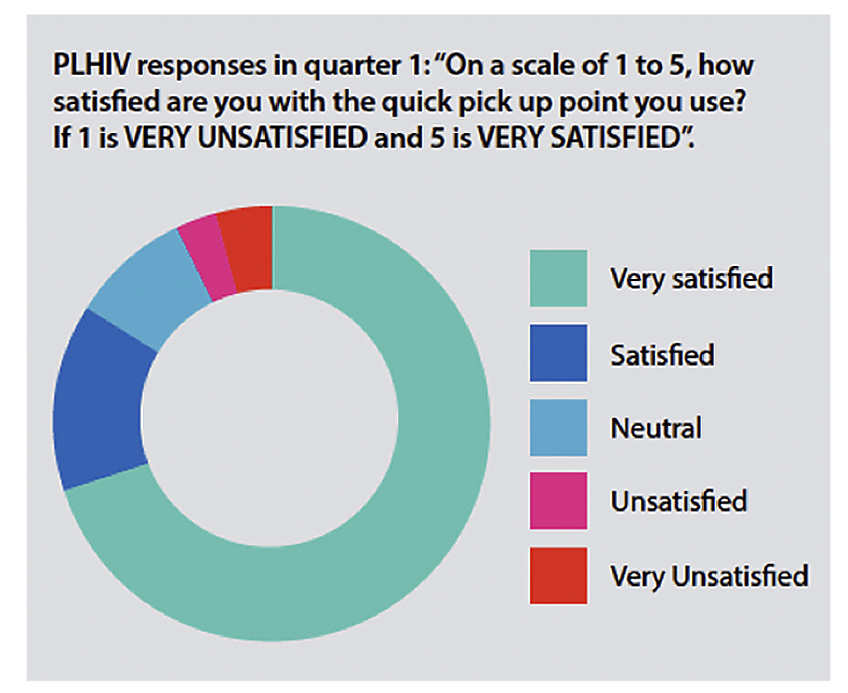
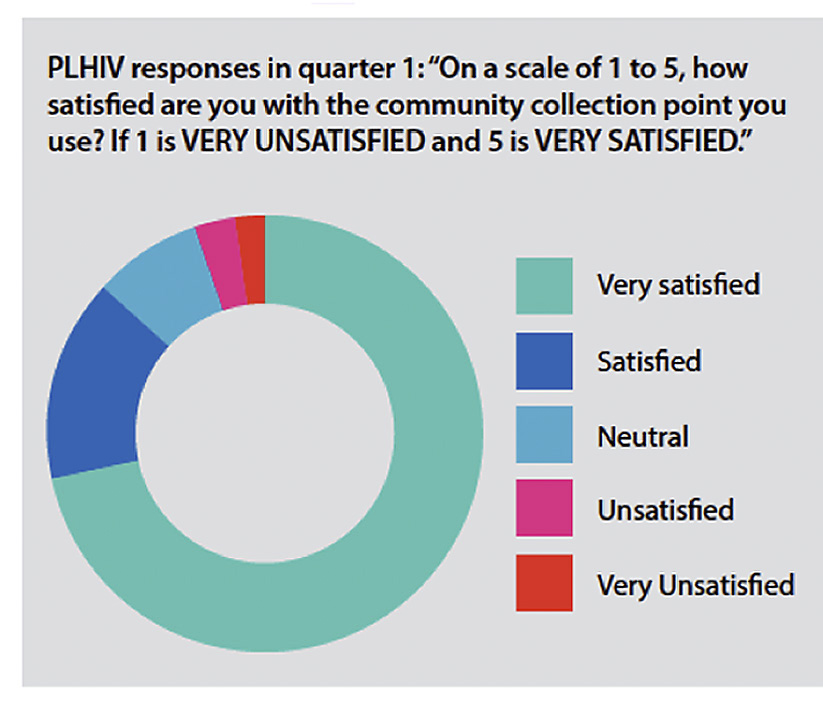
Overall, people living with HIV were positive and satisfied with models of medication pick-up — showing that more people living with HIV who are eligible should be allowed to use these options instead of going to the clinic. However, many eligible people living with HIV still do not use any of these options and continue to collect their refills at the clinic after review by a doctor or nurse.
/file/dailymaverick/wp-content/uploads/2021/05/MC-Oped-Lotti-Graph2_1.jpg)
Adherence clubs are also important.
We have long been pushing for enabling people living with HIV to join functional adherence clubs that not only make ARV collection quicker but also allow people living with HIV to join discussions as an opportunity to get the much-needed treatment literacy information and peer support they may require to support them to remain adherent. The data collected through Ritshidze shows mixed results around Adherence Clubs. 91% of adherence club members say they make it quicker than waiting at the clinic and overall, people living with HIV using clubs have a reasonably high satisfaction level.
However, 27% of adherence club members said that they did not get information about the importance of adherence, did not know, or only got information at the first meeting. 30% of people living with HIV reported that club meetings lasted less than 30 minutes — which also points to clubs being a pickup point rather than a space for discussion and peer support. Just over 25% of adherence club members do not get peer support from adherence clubs (18.6% state they do not get support and 6.7% state they do not know if they get support which points to a lack of peer support).
“I don’t default intentionally, but it costs me R24 to the clinic and R24 back for taxi, and it’s too far to walk. When you tell the clinic staff they don’t even care and they don’t try to help.”
We maintain that functional adherence clubs play an important role in providing adequate treatment literacy information to ensure people living with HIV stay on treatment and that these should not be simply cancelled in light of Covid-19. We need to work together to find safe solutions during the ongoing pandemic to ensure that people living with HIV can still gain the benefits from these options.
So, what can be done about this?
Get more people to use repeat prescription collection strategies. Scale up to reach 60% of all people living with HIV and ensure 25% are accessing treatment from a community-model and 20% from an adherence club.
Carry out an audit into the functionality of adherence clubs and urgently fix those that are not fulfilling their function properly (we outline the requirements for a functional adherence club in the People’s COP21). DM/MC
Data related to the Western Cape has not been included in the above since there are ongoing discussions with the Western Cape provincial department on allowing Ritshidze to proceed with monitoring. Until this negotiation has concluded, the Western Cape Department of Health has refused to allow Ritshidze to engage in monitoring or publish any findings.
This article was originally published by Ritshidze here. The dataset referred to was presented to an Operation Phuthuma meeting on 5th March 2020. You can view the full presentation here. For more updates from Ritshidze, follow them on Twitter, Facebook and Instagram or go to their website at www.ritshidze.org.za.
The Treatment Action campaign participates in the Ritshidze project. Spotlight is published by SECTION27 and the Treatment Action Campaign but is editorially independent, an independence that the editors guard jealously. The views expressed in this article are not the views of Spotlight.




 Long queues at Manzini Clinic in Mpumalanga. (Photo: Ritshidze / Spotlight)
Long queues at Manzini Clinic in Mpumalanga. (Photo: Ritshidze / Spotlight)