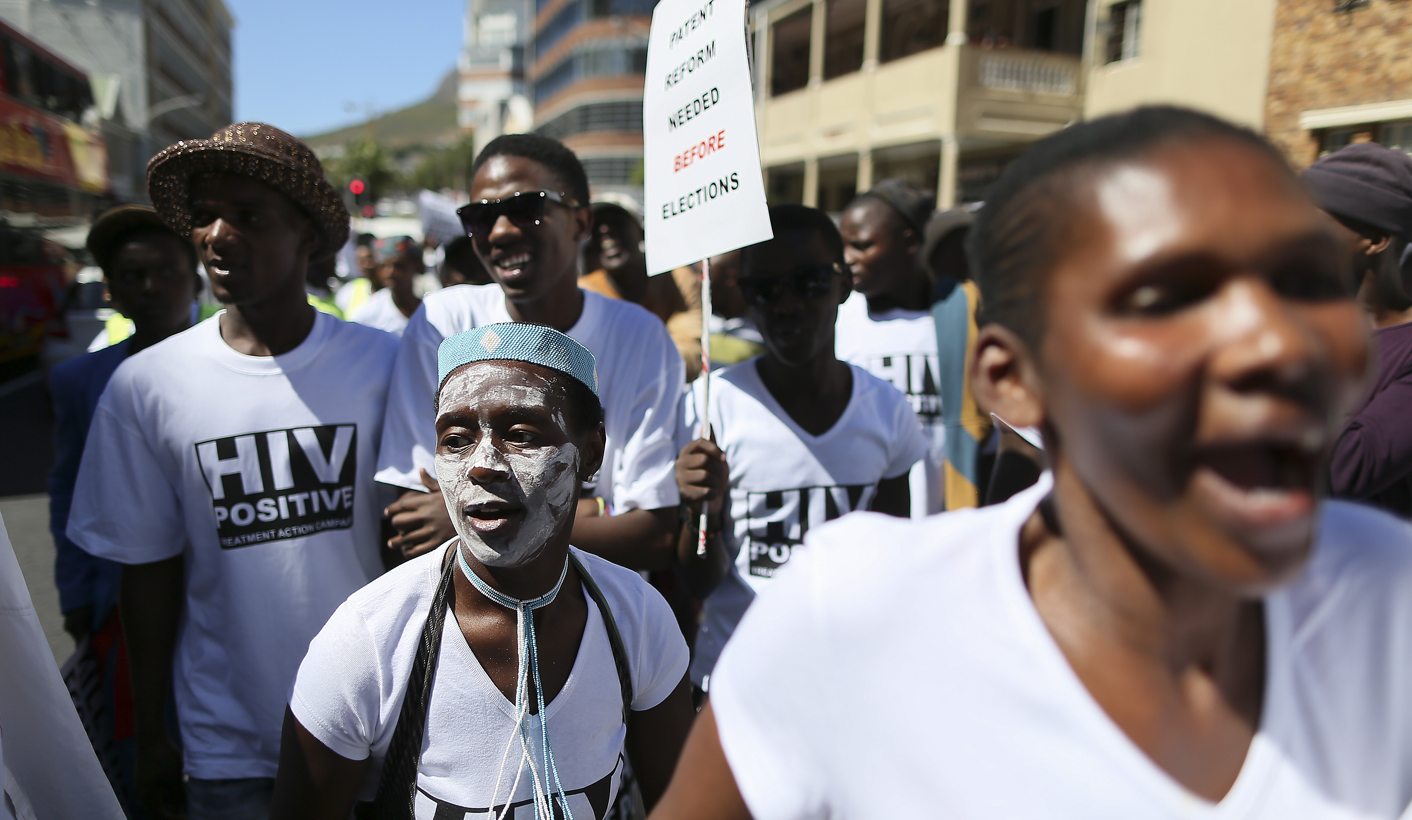If you want to paint the picture in the simplest possible terms, South Africa has made enormous strides in some aspects of HIV/Aids prevention and treatment, but as we celebrate our victories, a slightly more sinister trend has developed alongside: complacency.
Mark Heywood, director of the Aids Law Project, explains: “On some fronts we have covered enormous distance. We have three million people on ARV treatment; we have reduced mother-to-child transmission. We have rolled out significant medical male circumcision programmes. All these things have changed the landscape of HIV. But this does not mean everything is okay.
“On other fronts there has been little to no progress, namely in behaviour change for HIV prevention. Most of the prevention we have achieved is in the biomedical area.”
Heywood credits Minister Aaron Motsoaledi with having driven a significant turnaround since coming into office; South Africa, despite its high prevalence, is no longer regarded as the kind of disaster area it was under Manto Tshabalala-Msimang. In June 2015, Deputy President Cyril Ramaphosa opened the seventh South African Aids Conference by saying South Africa was turning the tide on the Aids epidemic.
“It is an undeniable fact,” he said. “The advances we have made, have been made together. Many emanate from public programmes, but still others have been made by grassroots activists, many of whom are present.”
He added: "We have the right policies in place and the political will to see them implemented. South Africa has the biggest HIV treatment programme in the world, with more than 3 million people on life-saving antiretrovirals, moving on to five million… we now know that the fight against Aids and TB can be won.”
According to Ramaphosa, South Africa was recognised by UNAIDS and other international bodies as a global leader in the fight against both HIV and TB.
But, says Heywood, government policy and civil society might not be reaching far enough to achieve Motsoaledi’s goal of a zero infection rate by 2030; or UNAIDS’ target of ‘90-90-90’: By 2020, 90% of all people living with HIV should know their HIV status, 90% of all people with diagnosed HIV infection should receive sustained antiretroviral therapy, and 90% of all people receiving antiretroviral therapy should have viral suppression.
“If there was behaviour change in terms of condom use or sex with fewer partners, for example, that is now being reversed,” says Heywood. “Knowledge and awareness is in fact declining. For me, what that points to is that Motsoaledi has done his job well. But when we talk about political commitment to HIV, it must be across government departments, whose conduct has direct bearing on whether we get on top of this epidemic.” Sex education in schools is a primary example, says Heywood, where standardisation on the quality of teaching has never been finalised, and the accessibility of condoms for teens remains a policy that “rattles around in hallways” without conclusion. Another example is medication stock-outs, which Heywood noted as a critical example and which Doctors Without Borders’ Ryan Fortune called the “not-so-small elephant in the room”.
“Nothing really changes at the coalface,” Heywood says, “especially the coalface of young women’s risk.” The result? A dramatically higher infection rate among adolescents – as reported on by Simon Allison.
So, although the numbers look promising on a macro level, there are concerning trends once one begins to examine the data in more detail.
Speaking to Daily Maverick, Heywood stressed that behavioural change – although it was the lengthier route towards HIV/Aids eradication – was a crucial component to intervention.
“I wouldn’t say I’m feeling pessimistic, but if you don’t get society mobilised around HIV and TB, we will find ourselves in trouble before too long. If you look at the crisis of organisations like TAC, you’ll find political commitment never came of its own accord – it was forced. If civil society loses the commitment to keep politicians on their toes, we will go backwards. We still have a thousand infections a day and three hundred deaths a day in South Africa.”
The Human Sciences Research Council (HSRC)’s recent South African household survey, released in March 2014 and conducted amongst 15,000 households, showed that there was serious need for behavioural intervention. In a nutshell, it found that South Africans were using condoms less often, having more sexual partners, and becoming more ignorant about HIV/Aids.
According to the survey, 67.5% of men aged 15 – 24 reported using condoms at their last sexual encounter, down from 85.2% in 2008.
The HSRC has also reported worrying trends among adolescents in their research; in 2014 they found there was little improvement in adolescent behaviour since 2010. More than one in 10 boys and one in seven girls had had sex by the time they turned 15. Amongst the youngest, ranging from pre-teens to 14-year-olds, nearly 11% of boys and 14.5% of girls had had sex.
Over 25% of girls had had sex with older male partners, which the report noted placed them at a greater risk of contracting HIV because “older male partners were more likely to be HIV positive”. Among boys who were sexually active in the 15- to 18-year-old group, a third had had more than two sexual partners in the last year.
Jenn Warren, communications manager for Grassroot Soccer – which runs life skills programmes for young people in South African townships as well as elsewhere in Africa – says there is a definite need for more interventions targeted at behavioural change. “In South Africa, the consequences of harmful gender norms are severe, particularly for girls,” she says. “These power imbalances result in widespread acceptance of violence against women, and low self-esteem, early exposure to sex and increased risk of HIV. In Khayelitsha alone, a reported 15.1% of girls aged 16 to 18 have dropped out of school, for reasons including poverty, family commitment, poor performance, disability and illness, and teenage pregnancy.” One in four new infections in SA occur among young women and girls between the ages of 15 and 24.
Biomedical programmes are crucial as an immediate intervention, but it’s important not to let them replace behavioural change, which is the only long-term solution, she told Daily Maverick.
HIV/tuberculosis unit coordinator at the Southern Africa Medical Unit, Dr Eric Goemaere, told Daily Maverick the same after the World Health Organisation updated its treatment guidelines earlier this year, which could make pre-exposure prophylaxis (PrEP) available in South Africa in due course. “It’s linked to adherence,” he pointed out. Even prophylaxis, he said, has been effective to a limited degree where patients have for whatever reason not adhered to a treatment or prevention programme.
"We need a massive HIV prevention campaign that begins with the promotion of condom use and the reduction of multiple concurrent partnerships, but that also addresses sexual coercion, transactional sex, intergenerational sex, risky sex linked to the use of alcohol and drugs, lack of access to work for young women, ignorance, powerlessness and poverty," Deputy President Ramaphosa summed it up.
MSF (Doctors Without Borders) spoke to Daily Maverick last week, expressing a need for more high-quality public awareness programmes aimed at behavioural change. Referencing the abovementioned HSRC report, media liaison Kate Ribet said, “South Africa has 6.4 million people – 10% of our population – living with HIV. Half are on treatment. Each year this figure grows by 350,000, mainly young women aged 15-30. It’s the highest number of new infections of any country in the world.
“From our 20 years of experience of delivering HIV care in Khayelitsha, MSF believes that a much more hands on, community driven approach is needed.” MSF recently launched a new public awareness campaign, #lifebeyondHIV.
Ribet said the organisation wasn’t under illusions as to the impact one campaign could have, but that it was a start; after all, a number of public awareness campaigns surrounding Ebola did, ultimately, make a difference to the base of public knowledge.
“[From surveys and focus groups held] we’ve noticed a general apathy from many young people towards standard HIV messaging - posters, T-shirts, billboards, etc,” she said. “We’ve also noticed a real reduction in recent years of public information campaigns around HIV – getting people to ‘test and treat’ for example.
“A large number of young South Africans seem to accept the risks of unprotected sex.
“Either young people now see HIV as a ‘safe’ and treatable condition, or the messaging isn’t being adapted for them. We’ve conceptualised our campaign towards a young audience – but the jury’s still out on what impact it has.”
Like Heywood, Ribet also spoke of a decline in will amongst South Africans of all flavours. Heywood worded this carefully; he was reluctant to speak of “fatigue”, saying that was a word used more often by potential donors or activists to excuse inactivity. Rather, one could speak of a climate in which life was devalued generally. “In an epidemic of alcoholism, unemployment, violence, and domestic violence, you can’t speak of HIV as if it exists in isolation – it doesn’t,” he said.
For MSF, the idea was to change the key message(s) for more current relevance. #lifebeyondHIV is a multi-pronged campaign, which began with a number of collaborative focus groups and creative interventions. MSF has been working in Khayelitsha for 20 years, so the first step was a series of workshops between local township artists, local hip-hop musician Phzo (the campaign track can be downloaded here) MSF’s HIV counsellors, TAC activists, and a number people living “productively and fearlessly” with HIV. Phzo said he was inspired to write the track by the people he met on the campaign.
Ribet’s colleague, field officer Ryan Fortune, added: “Because South Africa’s public health facilities are already extremely over-burdened, any hope of achieving 90-90-90 will depend on the extent to which testing can take place in community spaces (taxi ranks, door-to-door, mobile clinics, at schools) instead of waiting for, or expecting, people to walk into hospitals, clinics or health centres, and sit in long queues to get tested.
“Doctors Without Borders has been piloting exactly this kind of pro-active testing in Khayelitsha, Eshowe, and KZN.” Khayelitsha’s Community Adherence Club, which drives adherence-focused behaviour change, has been hugely successful, Fortune said. The model has been adopted by the Western Cape Health Department, and rolled out across the entire province.
He added: “If the aim is to drastically scale up the numbers of HIV-positive people accessing and adhering to their anti-retroviral treatment, community-level interventions are again, in our experience, the best response. South Africa’s already over-burdened hospitals, clinics and health centres simply cannot be expected to accommodate millions of new patients queuing up every month to collect their ARVs.”
Motsoaledi is not disagreeing with these sentiments. The worry is that it should not come at the expense of biomedical support. “Changing people's behaviour is a very difficult thing. In South Africa people are already saying, 'You're becoming a nanny state. You must allow us to choose,’ he said previously. “In simple language they're saying, 'Allow me to get as sick as I can, and you fix me as a state.' Which is a very wrong phenomena…That's not how the world is. It's just a dream of people. They don't want to say, 'Look, I must also try my best not to get ill, especially when it comes to lifestyle diseases.'”
The minister is acutely aware of the terrible twosome of HIV and TB; TB is currently the leading cause of death in South Africa and, says Heywood, the actual death toll is in all likelihood much higher than the official statistics have it. Last month, the WHO reported in Washington that South Africans were contracting TB at a higher rate than in any other country but Lesotho, with an annual incidence rate of 834 per 100,000, while Lesotho’s stood at 852 per 100,000 for 2014.
That said, Motsoaledi in 2014 described the rapid TB diagnostic tool GeneXpert as a “game changer”, and earlier this year Yogan Pillay, the Department of Health’s head of HIV/Aids, TB, and maternal and child health, said that South Africa’s TB incidence rate was declining. The treatment success rate is 78% (WHO’s target is 85%). Heywood, however, points out that drug-resistant TB is an increasing challenge.
Going forward, government has promised an aggressive approach to TB, as well as to HIV/Aids. Motsoaledi, for one, appears committed to his 2030 goal.
“One of the weaknesses in South Africa [in the past] was a wrong HIV/AIDS policy…It's legendary,” he told a US journalist in September 2014. “That's why now our program is one of the biggest in the world… It's huge, but we're actually planning to double it in the next 24 months. Now it's got 2.4 million people on treatment. We want to raise it to 4.6 million people in the next 24 months."
He has also voiced concern about the increased infection rate among adolescents, and has promised to redouble efforts to change this. At the SA Aids Conference this year, he admitted (crucially) that this group had been “overlooked”. He’s since added that government-issue condoms are possibly perceived as boring or unappealing, and that these would be replaced with a "new type of condom that will bring excitement"; flavoured and coloured versions, it turns out.
South Africa is gaining on HIV, but if we don’t accelerate, we’re going to slide backwards. And the multi-billion dollar question, of course, is where the money to keep forging ahead will come from. An analysis released earlier in 2015, noted that the cost of sustaining South Africa’s HIV programme would more than double per year by 2033 – and that doesn’t include the expansions that Minister Motsoaledi has described. The report, led by Wits University health economist Dr Gesine Meyer-Rath, described the 18 most cost-effective ways to tackle the Aids epidemic and, wrote the authors, current budgets would only allow for South Africa to implement around two-thirds of these programmes at the levels needed to reach United National targets committed to by Motsoaledi last year.
“We are mid-stream now,” Heywood told Daily Maverick. “My concern is that swimming to the other side may be more difficult than it was getting to mid-stream.
“What will help for the next eight months is that the International Aids Conference will be in Durban next year, which will put the spotlight back on South Africa and what is happening in developing countries. Not just Motsoaledi, but the whole Cabinet will be anxious to show that it is doing the right thing. So we’ve got a little leverage.
“After that, I really don’t know.” DM
Photo: Thousands of health activists from thirteen organisations march in protest against the government in Cape Town, South Africa, 13 March 2014. EPA/NIC BOTHMA
Read more:
http://www.avert.org/professionals/hiv-around-world/sub-saharan-africa/overview
http://www.hsrc.ac.za/uploads/pageContent/4565/SABSSM%20IV%20LEO%20final.pdf
http://www.unaids.org/en/resources/campaigns/post2015
http://www.unaids.org/en/resources/campaigns/post2015/defeatingaidsadvancingglobalhealth