Presentations on the National Health Insurance (NHI) Bill heard by the Portfolio Committee on Health were collated by the Parliamentary Monitoring Group and analysed by researchers from the South African Medical Research Council, the Clinton Health Access Initiative and the universities of the Western Cape and Cape Town.
Everyone wants to know what benefits the NHI will cover.
Clause 25(4) of the bill provides for a benefits advisory committee to review the benefits and types of services that the NHI will cover and, in consultation with the minister of health and the board, to determine the healthcare benefits the fund will provide. Most respondents declared support for the bill’s aim of progressively realising universal healthcare. The trade union Nehawu said this “would allow for people to access healthcare services without incurring any financial hardship”.
However, respondents were concerned by the “open-ended” nature of clause 25(4). The bill was considered to lack detail on what services would be covered, their affordability and the level at which they would be offered. Inherent difficulties in the process of deciding on a benefits package under potentially severe budgetary constraints were identified. The bill has no information on how the benefits package should be determined.
What will the NHI cover?
Several respondents wanted greater clarity on what would be included in the NHI benefits package.
The Professional Provident Society and the US multinational pharmaceutical company MSD (known as Merck in the US and Canada) called for the NHI to “spell out” the benefits package. The South African Medical Association argued that it was “extremely difficult for health practitioners to support the NHI reforms, not knowing what will be available to patients, or under what conditions”. The National Health Laboratory Service argued that the bill should clearly state what the package would contain, what would be excluded and how excluded benefits would be paid for.
Affordability and level of benefits
The Health Funders Association was concerned that “given budgetary constraints, the NHI is likely to cover a much narrower range of services than what is currently provided by medical schemes”. Wits University pointed to the findings of the ministerial task team on social health insurance (2005), which concluded that “even with a minimum benefit, costed at the lowest level feasible, it appears not to be affordable in the medium term. Overall health expenditure would rise to exceed 11.3% of GDP.”
The Pharmaceutical Task Group was concerned that rationing medicine benefits to a level lower than currently available benefits would compromise patient care and health outcomes.
Funding constraints, benefits and trade-offs
The success of the NHI may depend on the extent to which it can successfully manage, within funding constraints, the inevitable trade-offs between the types and comprehensiveness of different benefits in the package of care. Respondents highlighted the difficulties this entailed, expressing concern about the lack of clarity on the approach, principles and process to be used.
While welcoming the move away from the current (mainly public sector) model of implicit rationing (via stockouts or differential service availability, for example) towards the more explicit rationing model implied by a “benefits package”, the Faculty of Health Sciences at UCT pointed out that it would be extremely challenging to create an affordable list of benefits. The medico-legal risks associated with getting this wrong were high.
MSD said the bill did not provide criteria for determining the benefits package and there were no clear inclusion or exclusion criteria. The meaning and intent of phrases such as “medically necessary” or “comprehensive” alluding to benefits were unclear. There were also no principles or guidelines within which the benefits advisory committee was required to act. This would make it impossible for the committee to comply with healthcare professional legislation.
The Faculty of Health Sciences at UCT recommended that, while some of the benefits needed to remain implicit, the fund should be explicit about health benefits to be covered, referral pathways, essential medicine and laboratory lists and clinical guidelines, as well as areas of “disinvestment” – benefits that the fund would not cover.
In terms of process, Mediclinic called for a “transparent process for determining the benefits package, taking into account access, quality and affordability”. In a similar vein, the US multinational medical technology company Becton Dickinson called for the governance processes in the selection and functioning of the benefits advisory committee and health services pricing committee to be adequately defined. MSD called for the benefits advisory committee’s recommendations to be binding.
Some principles for determining the benefits package were identified. MSD and wound-care product manufacturer Systagenix urged the use of an evidence-based medicine guide. Healthcare company Johnson & Johnson called for the principles underlying the determination of “comprehensive or “necessary” care to be made clear. The French multinational healthcare company Sanofi called for “affordable” universal access to be defined within the legal mandate of the fund. The South African Human Rights Council said: “Basic health services must be clearly defined to be in line with the Constitution as well as accepted international standards.”
No benefits for broader society
The Public Health Association of South Africa, the Medical Research Council of South Africa, the Collaboration for Health Systems Analysis and Innovation and others were concerned that the bill mainly focused on personal health services and neglected services related to the broader social determinants of health, disease prevention and health promotion.
This “contradicts the principles related to addressing social determinants of health outlined in the NHI White Paper” and reflects the “extremely narrow” conceptualisation of prevention and promotion in the bill, they said.
While recognising the importance of personal services, they recommended that the bill place greater emphasis on “intersectoral action to support health promotion, disease prevention and address the social determinants of health”.
Lobbying
The hearings revealed numerous groups lobbying for the inclusion of benefits linked to services provided by their constituency. Table 1 summarises a sample of organisations and the specific benefits for which they lobbied. Many of these organisations focused exclusively on lobbying for their interests and made no other comments on the bill.
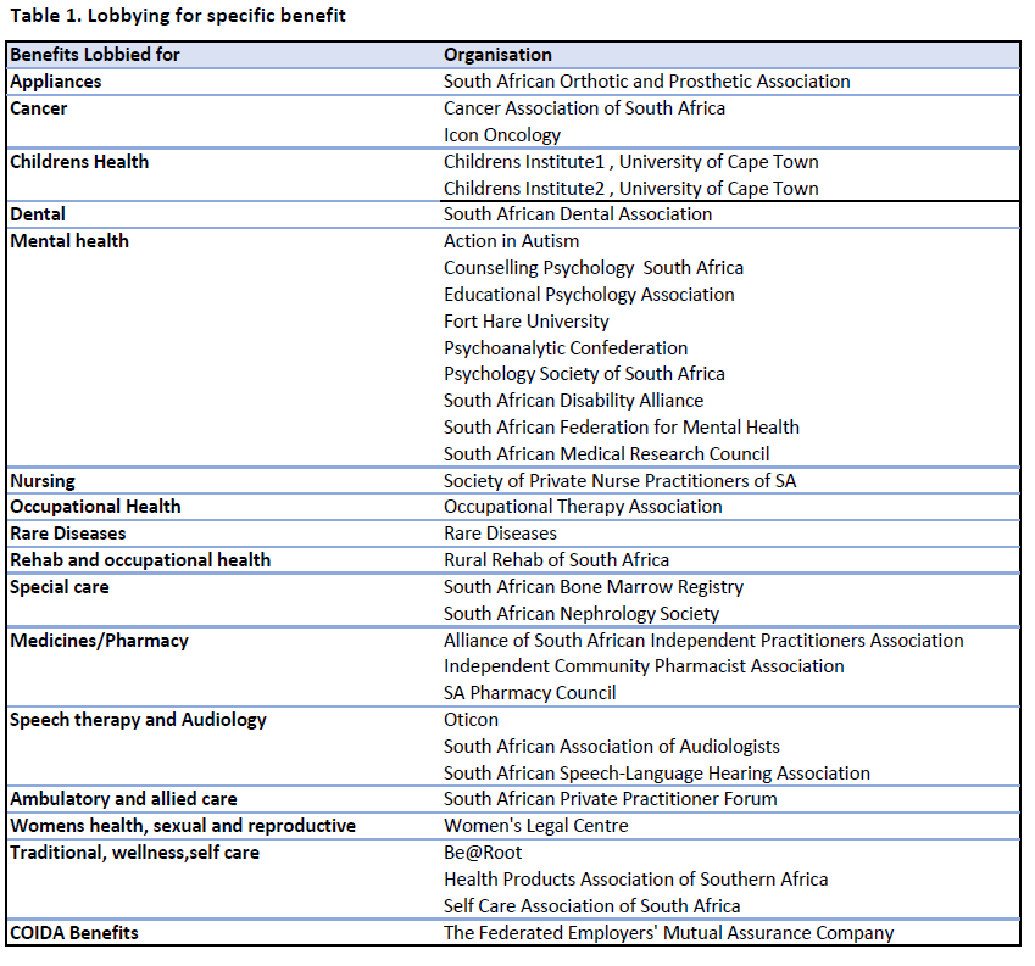
The Portfolio Committee on Health faces a challenge to reconcile the passionate demands of these special interest groups with the NHI brief to serve the best interests of population health.
Publicity around the NHI seems to have heightened expectations that the NHI will provide for “all healthcare needs without financial difficulty”. However, potentially severe financial constraints will require the NHI to carefully balance the types and comprehensiveness of the benefits it chooses to cover. Many respondents pointed out the bill’s lack of clarity on the benefits to be offered, and on processes and principles to guide the NHI in determining the benefits package.
C0mparisons with current medical aid scheme benefit packages seem inevitable, so the criteria and process of benefit selection by the NHI are likely to be subjected to ongoing public scrutiny. The task is likely to be complicated by the lobbying for selected benefits by special interest groups.
Committee’s challenge
The Portfolio Committee on Health faces a clear challenge to specify the NHI benefits and to provide more detail on the critical process of benefits definition and selection, or to leave the legislation “open-ended” as currently drafted.
The case for amending the bill to specify the benefits is weak. Any benefits the fund chooses to cover will be dependent on available funding and circumstances at a particular point in time. Specifying benefits in the bill would then require amendments to the bill each time benefits need to be changed – an onerous process.
The case for amending the bill to provide a clear process and principles to guide the NHI in determining the benefits package is far stronger. Benefit determination is a passionately contested terrain, and therefore amending the bill to provide clearer legislative guidelines will help the fund navigate this terrain.
With its focus on personal clinical care, the NHI Bill makes only rhetorical reference to comprehensive care, but several groups pointed out the exclusion of key public health measures required to ensure population health. This role is defined outside the brief of the NHI Bill, a serious omission in the eyes of some. To address this, the bill would need to fundamentally expand its scope of responsibility or make it clear that the responsibility for this level of healthcare lies elsewhere.
Based on their line of questioning during the hearing, the members of the Portfolio Committee on Health recognised that getting the benefits package right is critical to the success of the NHI. The Portfolio Committee on Health finding a way to establish a framework that allows for the benefits package to be determined in a manner which is effective and acceptable to broader society will be critical to the success of the NHI. DM/MC
This is the sixth article in our series about different issues dealt with in public submissions to Parliament on the NHI Bill. See Part 1, Part 2, Part 3, Part 4 and Part 5.
Geetesh Solanki is a specialist scientist at the Health Systems Research Unit at the SA Medical Research Council, an honorary research associate in the Health Economics Unit at the University of Cape Town and the principal consultant at NMG Consultants and Actuaries. Neil Myburgh is a professor in the Department of Community Dentistry, Faculty of Dentistry and WHO Collaborating Centre for Oral Health at the University of Western Cape. Stephanie Wild is a postgraduate student enrolled for an MPhil in Public Law at the University of Cape Town. Judith Cornell is a former director of institutional development and planning at the Nelson Mandela School of Public Governance, University of Cape Town. Vishal Brijlal is a senior director at the Clinton Health Access Initiative.
The opinions expressed are those of the authors and do not necessarily reflect the views of their institutions.
[hearken id="daily-maverick/9472"]




 (Photo: Leila Dougan)
(Photo: Leila Dougan)