Ballooning cancer costs coupled with a still-flimsy strategy for a broad continuum of care means planning effectively for the next decade must come down to doing better than just throwing money at an enlarging public health burden.
The Cancer Alliance launched its Cost to Cancer Report this month alongside a commissioned cost modelling and projections report. Together, the new findings make a clear case for plugging gaps now to avert a future crisis. The report sets out clearly how the cost of cancer care continues to explode, while the unequal access to quality care becomes more firmly entrenched and provision for adequate human resources — from community healthcare workers to specialist clinicians and technicians — remains under pressure (see the Maverick Citizen article of 2 September 2021).
A Cancer Alliance webinar on 7 September unpacked the modelling and projects by actuarial consulting firm Percept. Participants also heard from clinicians, public health activists and a National Treasury representative who tabled strategies for better budgeting and investment; more patient-focused care and representation; better data collection and analysis; and greater advocacy and civil society support to put cancer awareness on the public agenda.
Public health consultants at Percept and report co-authors Jodi Wishnia and Emma Finestock set out the methodology for the modelling. The research focused on the incidence of six cancers — breast, prostate, cervical, haematological and paediatric — over the next 10 years and the expected costs of treating them in that period.
“The purpose of this model is to assist with a budget submission to National Treasury for cancer services,” Wishnia said, pointing out that they found that an additional R50-billion will need to be budgeted for by the end of the decade.
“Prostate, cervical and breast cancer have the highest projected incidence. Most of the incident cervical cancer and lymphoma cases occur in people living with HIV… The high prevalence of HIV in South Africa is therefore a key driver of the increasing incidence of these cancers,” the researchers also noted in their report.
The co-authors said their “best buys” would focus on improving access to early screening interventions and changing poor health-seeking behaviour, especially among men.
“We feel very strongly that the approach to the cancer incidence and the burden should be married to other disease approaches — we don’t need another conditional grant only for cancer, as humans present with multiple conditions in the system,” Wishnia said.
“As some of the cancers are intimately linked to HIV, there is a case for using some of the HIV conditional grant funding money to make access to treatment more of a reality for those particular cancers.”
The call for “entire care cascade from prevention, screening, early diagnosis treatment and palliative care” was reiterated by Dr Yogan Pillay, former deputy director-general for health programmes, now country director with the Clinton Health Access Initiative.
In his presentation, Pillay said: “We need to use the patent laws to lower the cost of cancer treatments. We did this with HIV by moving to generics.”
Pillay said developing an effective national cancer strategic framework beyond 2022 would also have to be about filling and replenishing healthcare personnel at all levels and focusing on accurate data collection at a community level.
Treasury chief director Mark Blecher represented the government at the webinar. He said that over the next 10 years they expect “in real prices, cancer funding would need to increase from R16-billion to R36-billion — a R20-billion increase for funding cancer care [Precept’s numbers come closer to R50-billion]. There’s no question that finding R20-billion is a lot of money, but when you look at it like this over 10 years, then the numbers start becoming much more manageable.”
Currently, Blecher said, Treasury has ring-fenced R771-million over three years for cancer care. He added, though, that better governance and support for strategic planning, invention and monitoring still count for better impact.
“A lot of these things are not necessarily just the money; the money is just part of it. A lot of it is management and governance,” he said.
Blecher also flagged the inequality in the public and private sectors and noted that these partnerships need to be re-examined so “strategic purchasing” can translate into quality care for more patients.
Professor Lydia Cairncross, head of the Breast and Endocrine Surgery Unit at the University of Cape Town’s Faculty of Health Sciences at Groote Schuur Hospital, said during the webinar that it’s still patients’ lived realities that should be the most visible human cost of cancer.
She added: “We need to count the cost of a fragmented health system and a fragmented approach to cancer care… People often forget that surgery is only about 50% of cancer care. That’s only at the level of treatment; we also need an integrated approach at the primary level. There’s a blind spot that cancer is this hi-tech, highly specialised disease, but actually, cancer diagnosis starts right at the level of a patient knowing that their symptom could be a cancer.”
She added that the public service also needs to be “better capacitated” and policy and practice need to intersect better for real health impact, not just what makes up talking points and words on a document.
Improving treatment literacy, putting the focus on listening and hearing from patients and being unapologetic about demanding the right to decent healthcare are critical advocacy strategies, said Treatment Action Campaign chairperson Sibongile Tshabalala.
Tshabalala said the lessons from fighting HIV/AIDS “may not be 100% there, but show us what can be done and that they should be used everywhere”. The TAC and the Cancer Alliance have already joined forces to make a stronger civil society stand.
The next step for the Cancer Alliance is to use the evidence and data gathered for the report to inform upcoming “inclusive solution think-tanks”. Its call remains for more collaboration and empowered decision-making and intervention. It will help South Africa cover more bases with less and help the country track closer to a best-case scenario for a cancer burden by the time 2030 rolls around. DM/MC





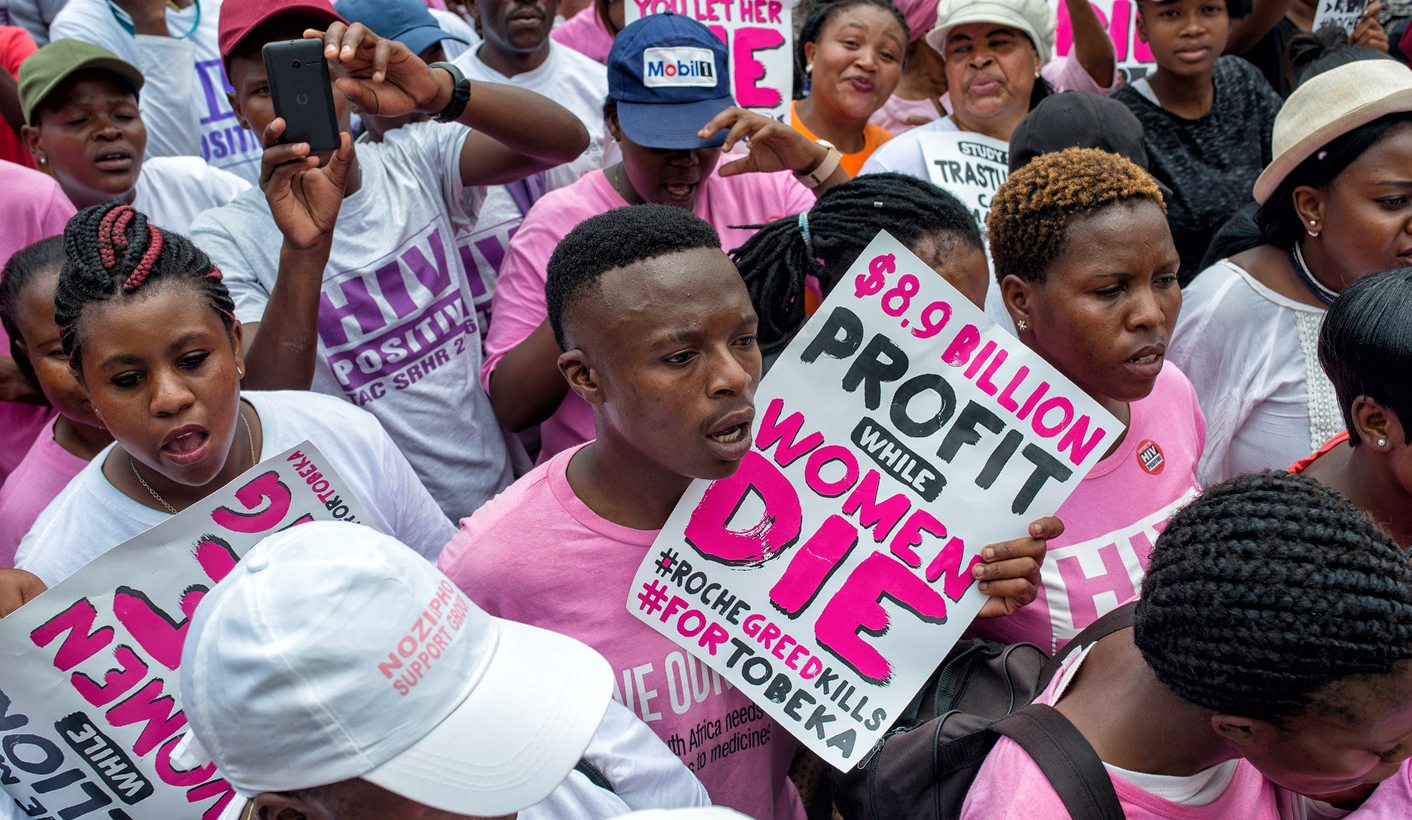 Treatment Action Campaign members protest against the high price of a life-saving breast cancer drug. (Photo: Ihsaan Haffejee)
Treatment Action Campaign members protest against the high price of a life-saving breast cancer drug. (Photo: Ihsaan Haffejee)