While the recovery in tuberculosis (TB) testing numbers is a step in the right direction, speakers at the opening (under the theme of ‘working together to get TB control back on track’) left little doubt as to the scale of the challenges ahead in the country’s TB response. Even before Covid-19-related disruptions, South Africa had some of the world’s highest TB rates.
Improved testing numbers
Dr Harry Moultrie, senior medical epidemiologist for geospatial modelling at the National Institute of Communicable Diseases, presented data showing how TB testing numbers (using the GeneXpert molecular test) were substantially below forecasted levels from April to August 2020, then within the forecasted bounds from September 2020 to November 2021, and have been exceeding the upper bounds of forecasts since December 2021.
The data shows that from April to August 2020, 448,000 fewer tests were done than forecasted and 25,400 fewer positive tests were recorded than anticipated.
/file/dailymaverick/wp-content/uploads/2022/09/MC-TB-Conference_1-Graphic-1.jpg)
Moultrie said there were substantial differences in TB testing between provinces, districts, and sub-districts and that the increase in testing volumes in 2022 was largely driven by women aged 25 to 44. In 2022, the percentage testing positive in men is roughly double that in women.
Nelson Mandela Bay Metro in the Eastern Cape had the highest test positivity rate (>16%) of all districts. Bar the Overberg District, all districts in the Western Cape had test positivity rates from 14 to 16% along with Mangaung in the Free State which was also in this percentage bracket.
The lowest test positivity rates were recorded in KwaZulu-Natal’s uMzinyathi District (Dundee), Zululand, and uMkanyakude District in the north-east where between 0 and 2% of tests were positive.
Moultrie stressed that going forward, we will need locally targeted interventions to guide the country’s TB programme.
/file/dailymaverick/wp-content/uploads/2022/09/MC-TB-Conference_2-Graphic-2.jpg)
One intriguing finding is that as testing volumes have recovered, there hasn’t yet been a rebound in either the number of positive tests or test positivity above predicted levels. Though there is currently no definitive explanation for this, Moultrie suggested several possible explanations — such as it simply being too soon to see a rebound, non-pharmaceutical interventions potentially having reduced community transmission of TB, and the impact of certain policy changes (such as recent changes in testing strategy).
The bigger picture
Away from the TB testing numbers, the news is less good.
Dr Norbert Ndjeka, chief director of TB control and management at the national Department of Health, presented data showing that in 2020 South Africa was underperforming on three key indicators in the World Health Organization’s (WHO) End TB Strategy (2035). The TB incidence rate in the country dropped by 11% from 2015 to 2020 (the WHO’s target was 20%), so South Africa is only about halfway there. TB deaths have decreased by 9.2% (the WHO’s 2020 target was 35%), and 47% of TB patients faced catastrophic costs in accessing medication (the WHO’s 2020 target was 0%). Though TB medicines are free in the public sector in South Africa, patients face other costs, such as the cost of transport to healthcare facilities.
An underlying theme in Ndjeka’s presentation was the idea that in order to reduce TB incidence and deaths, we need to improve TB testing and linkage to care. He said finding people with undiagnosed TB is crucial, and told delegates, “we are not finding the people we should be finding”.
Visit Daily Maverick's home page for more news, analysis and investigations
“We need to be testing regardless of symptoms,” he said. “We are struggling to find people with TB, to link them and retain them in care. To deal with TB, we need to be looking at how many did we miss, [and] what if we had found them, and treat[ed] them. We need to find them all.”
These comments underline the Department of Health’s targeted universal testing (TUT) strategy by which TB tests are now offered to people living with HIV, people who recently had TB, and close contacts of people with TB, irrespective of whether or not they have any TB symptoms. An interesting new detail in Ndjeka’s presentation was the statement that such tests should be offered to eligible persons on an annual basis. Spotlight recently reported on the early experience with South Africa’s TUT rollout.
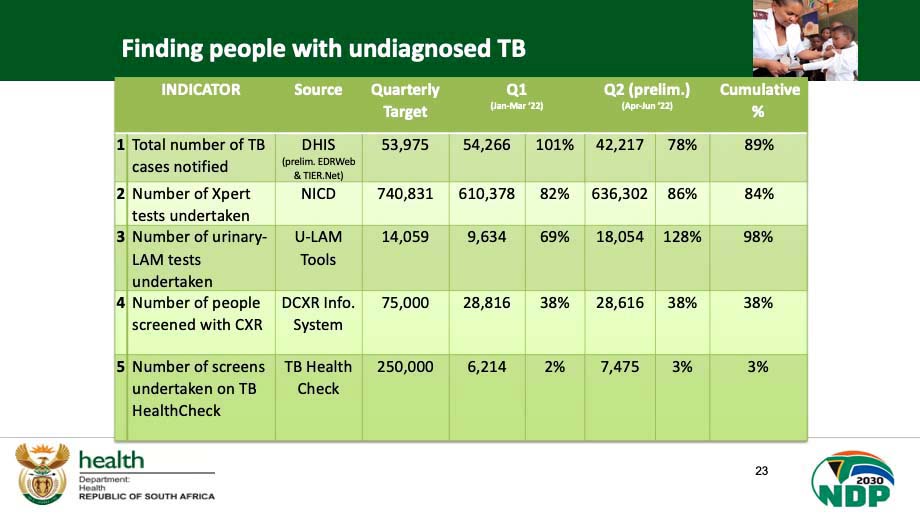
Ndjeka presented a list of TB testing and screening targets that form part of the government’s TB recovery plan — which in addition to the molecular testing used in TUT programmes also includes targets for X-ray screening and testing of immunocompromised people living with HIV with a urine test (urinary LAM).

The department set itself a quarterly target of 740,831 TB tests (using GeneXpert). In Quarter 1 (between January and March this year), they achieved 82% (610,378) of this target. In the second quarter (April to June), they showed a slight improvement with 86% of the quarterly target reached.
The quarterly target for urinary LAM tests was set at 14,059 but they only managed 69% (9,634) in the first quarter. In the second quarter, they over-performed with a figure of 128%, meaning they managed 18,054 LAM tests.
The quarterly target for digital X-ray screenings was set at 75,000 but by the first quarter, they only managed 38% and also 38% for the second quarter. The department also set itself the target of 250,000 screenings conducted on TB HealthCheck each quarter but only managed 2% in the first quarter and 3% in the second quarter.
Ndjeka said part of their strategic vision is to “support people from the moment they come into contact with a health provider to know their test result and link to care faster, provide better care, through shorter regimens and tailored support in facilities and communities, build an ethos that values prevention as much as treatment in which civil society and frontline workers feel supported”. He also said they need to create a culture of data-driven decision-making and build public-facing dashboards to help prioritise care to where it is most needed.
Not ‘business as usual’
“We need sound research to make meaningful strides and improve the experience of our TB clients in keeping with the End TB Strategy,” Deputy Minister of Health Dr Sibongiseni Dhlomo told delegates in his keynote address. “I trust that our presence here shows our commitment to science and the value we place on evidence-based medicine.”
This may sound like business as usual, Dhlomo said, referring to government’s TB plans. However, closer examination he said shows that there are some new interventions and exciting developments.
“For example, expanded screening activities with TB Check, as well as the use of digital chest X-ray for TB screening. Using SMS to provide patients with their TB results is also being introduced to link people to care faster and save people the trouble and cost of returning to the clinic when unnecessary,” he said.
He added that government is planning to introduce more patient-friendly treatment regimens to help improve retention in care — including a new four-month regimen for children and a new six-month regimen for drug-resistant TB. (Spotlight reported on the latter here and a story on the prior will be published on Friday).
/file/dailymaverick/wp-content/uploads/2022/09/MC-TB-Conference_5.jpg)
“We want to scale up implementation of TB preventive therapy including 3HP to improve TB prevention and reduce transmission, especially among people staying in the same home as someone who recently developed TB,” he said.
3HP is a TB prevention regimen consisting of the drugs rifapentine and isoniazid taken for three months, as opposed to the old standard of isoniazid for anything from six to 36 months. As Spotlight recently reported, the rollout of 3HP in South Africa finally seems set to gather steam after chronic delays.
South African National Aids Council CEO Thembisile Xulu said in order to make noticeable progress, we must acknowledge that TB is also largely a social problem and our response and interventions should not just be biomedical.
“As the theme of the conference suggests, we must work together to end TB stigma and discrimination because these continue to be barriers against TB management. We must change our TB management approach to be more holistic by engaging multi-sectoral stakeholders at every stage of the elimination process in order to make positive changes. We need to better understand the ‘lived’ experiences of both health workers involved in TB control and TB clients themselves,” she said.
In practice, she suggested, this means bringing the lab closer to patients and enabling a ‘test and treat’ approach in one visit. DM/MC
This article was published by Spotlight – health journalism in the public interest.





 Professor Willem Hanekom, director of the Africa Health Research Institute (AHRI) during the opening of the 7th SA Tuberculosis Conference in Durban. (Photo: Tiyese Jeranji / Spotlight)
Professor Willem Hanekom, director of the Africa Health Research Institute (AHRI) during the opening of the 7th SA Tuberculosis Conference in Durban. (Photo: Tiyese Jeranji / Spotlight)