The government plans to destroy 8.5 million doses of the Covid-19 vaccine produced by pharmaceutical company Pfizer at the end of October.
The situation also raises questions about the fate of a further 10.1 million stockpiled doses of the Johnson & Johnson vaccine that will expire between June and September 2023.
South Africa’s rate of vaccine doses administered per day has dropped to a fraction of its peak last year — even though a large segment of the population has still not been vaccinated. In September 2022, 33% of South Africa’s population was fully vaccinated, according to Our World in Data. It’s far off the initial 70% target set at the start of the vaccination drive early in 2021. By comparison, Rwanda reports an 83% fully vaccinated population, Botswana’s vaccinated population is reported to stand at 66% and Mozambique’s is 42%.
‘Shocking indictment’
Some public health researchers and specialists are pinning the failure to get shots into arms not on people’s deepening complacency or vaccine hesitancy, but on what they say is the Department of Health’s missteps and mistakes in managing the national vaccination drive since vaccines arrived in the country in the first quarter of 2021.
/file/dailymaverick/wp-content/uploads/2022/09/MC-Covid-Vaccines_1.jpg)
“That these vaccines are going to be destroyed is a shocking indictment of a vaccination programme that has been badly run from inception. What is incomprehensible is why there was no expertise in mass public health programmes from the beginning,” says Professor Francois Venter, the divisional director of Wits University’s health platform, Ezintsha. Venter was also a member of the Ministerial Advisory Committee early in the pandemic.
“This was always going to fail because the Department of Health and the private sector had this incredible confidence that they could by magic make this a success even though they had no track record. The key to getting people to take up any kind of public health service is ‘demand-creation’, and the people who know how to do this are those who work with programmes like male circumcision, HIV testing and ARV access — not the Department of Health or the private sector,” says Venter.
“From the start, there was no proper budget for advertising the vaccination services, there was no real strategy around what the key messaging was going to be, and the Department of Health just expected people to arrive at a local facility and get vaccinated.”
Venter says demand-creation combines creativity, accurate and consistent messaging, and urgency to get widespread buy-in. He says the first misstep was the halt in the roll-out of Astra Zeneca vaccines in February 2021. Then, he says, the EVDS (Electronic Verification Data System) failed to have substantial population penetration and now, Venter says, the “wheels [of the campaign] have fallen off”.
/file/dailymaverick/wp-content/uploads/2022/09/MC-Covid-Vaccines_2.jpg)
According to data from the SA coronavirus portal, by 11 September, a total of 37,535,745 vaccine doses had been administered. However, the number of daily doses administered nationwide recently dipped below 1,000 on weekends and below 10,000 on weekdays.
Waning vaccine demand comes against the backdrop of the South African Medical Research Council’s (SAMRC’s) sobering estimates of excess natural deaths. They estimate that the country has seen around 330,000 excess natural deaths since 3 May 2020 — with more than 270,000 of those probably directly due to Covid-19. In 2022, the SAMRC estimates there have so far been just over 42,000 excess natural deaths.
‘Dedicated resources not possible’
The Department of Health, however, insists the vaccination programme is on track.
“There is no problem with the national vaccination campaign. Vaccines are available, the vaccination programme has been integrated into the primary healthcare delivery system, and communication continues in all national media,” says Foster Mohale, the spokesperson for the National Department of Health.
/file/dailymaverick/wp-content/uploads/2022/09/MC-Covid-Vaccines_3.jpg)
“The challenge is that the public is complacent that there is no or low perceived risk. This is a complex challenge in a society that is easily influenced by inaccuracies and misinformation spread in social media,” he says.
Mohale says the vaccination programme is continuing with an eye on the possibility of another Covid-19 wave, but he admits that they face competing priorities. “The health system has to care for millions of people with other health conditions and needs and dedicated resources are not possible for Covid-19,” he says.
Wasted resources?
Destroying the vaccines in October may well be classified as wasted resources, but the financial value of the potential waste is hard to quantify. The government won’t disclose the cost of procuring the vaccines, citing “contractual agreements”.
Mohale says it has to be factored in that 7.9 million doses of the Pfizer vaccine, out of the 39 million doses received by South Africa, were a donation from the US government.
In April 2021, the then health minister Zweli Mkhize told Parliament that both Johnson & Johnson and Pfizer were selling their vaccines to the country at $10 a dose with no refunds or cancellations permitted. At that pricing, the cost of wasted vaccine doses come the end of October will run into tens of millions of dollars.
/file/dailymaverick/wp-content/uploads/2022/09/MC-Covid-Vaccines_4.jpg)
Mohale confirms that the “environmentally approved” disposal will come with its own price tag. Estimates are “R18 and R25 per kilogram of waste disposed and a tray of 1,170 doses weighs approximately 1.2 kilograms”.
Other options
The Department of Health says it is trying to extend the October expiry date by three months but is awaiting South African Health Products Regulatory Authority (Sahpra) approval. It has also attempted to offload the 8.5 million near-expiry vaccine doses to other countries.
Mohale says the government has approached the African Union and the Covax facility. The challenge though, he says, is that any recipient country has to agree to the “no-fault compensation scheme”, which indemnifies manufacturers in the event of any adverse events due to the vaccine.
The government has no plans to use up the vaccines by making them generally available to children under the age of 12. Mohale says the Vaccine Ministerial Advisory Committee has advised against the mass vaccination of “small children”, although vaccination for immune-compromised children between five and 11 is encouraged. He says the EVDS is being adapted to accommodate this population cohort.
The government will also not shorten the recommended intervals between booster shots in a bid to use up the vaccine doses. However, he says, “further boosters over time to accommodate waning immunity are under evaluation”.
/file/dailymaverick/wp-content/uploads/2022/09/MC-Covid-Vaccines_5.jpg)
‘Everything has been so slow’
Public health specialist Lynne Wilkinson says allowing the vaccines to go to waste without alternative campaigns to ensure they are used is a travesty. This is especially as vaccination rates in the country are so low and the unknowns around long Covid still pose potential health burdens for sufferers, she says.
“Government needs to think out of the box now by making an additional vaccine accessible and available for whoever wants one, or running vaccination blitz days or working with religious leaders to vaccinate at gatherings, for instance,” she says.
Wilkinson says at more than a year down the line into vaccination, there should have been lessons learned to inform a better vaccination strategy going forward. She says the exit of corruption-tainted Mkhize should also have been a moment for stronger leadership and revived confidence in vaccination rather than the vagueness that has now allowed people to self-assess Covid risks.
“Everything has been so slow and has just dribbled on and dribbled on instead of mobilising community-based organisations and making it easy for people to get a vaccine,” she says.
Wilkinson spearheaded a vaccination drive at the Bulungula Incubator based in the Eastern Cape village of Nqileni in 2021. Within weeks, she says, they achieved vaccination rates of more than 95% for over-60s as soon as vaccinations became available for this age cohort — and this in a deep rural setting.
“We activated all our community resources — meeting elders, going door to door and using community radio and making information clear and available,” she says.
‘Inequality, not hesitancy’
But many more villages and places that fall off the radar easily still need to be reached for vaccination.
Professor Kate Alexander of the University of Johannesburg’s Centre for Social Change, says low vaccination rates come down to inequality, not vaccine hesitancy. Alexander points out that it’s not a question of money either, with significant overseas donor money having been pumped into the country via the likes of USAID to accelerate the vaccination roll-out.
“Government just doesn’t have a clue about how to deal with issues of inequality, so hesitancy becomes an argument by which the government blames ordinary people for the vaccine uptake instead of working on simple interventions to get rid of barriers.
“Government also doesn’t know how to relate to community-based organisations and focuses on existing ‘leadership’ rather than younger activists. Big NGOs have a similar problem,” she says.
Interventions, Alexander says, could be better access to information about vaccination sites, flexible operating hours for vaccination sites, addressing transport problems to get to sites, and mobilising community groups, like young people, to get the message across. She warns that failure to change direction puts the remaining 10 million vaccine doses in the stockpile in similar jeopardy of expiring before being used up.
“It’s scandalous and a shambles,” she says of the inaction. It’s prompted her to join the growing call for an inquiry into South Africa’s handling of the pandemic and vaccination campaign.
“An inquiry should be accessible to the public and have the right to subpoena evidence. The low level of vaccination is primarily a question for social science, whose practitioners would also have something valuable to say … if the relevant data was made publicly available,” she says. DM
Professor Francois Venter is quoted in this article. Venter is a member of Spotlight’s Editorial Advisory Panel. The panel provides the Spotlight editors with advice and feedback on the quality and relevance of Spotlight’s public interest health journalism. The Spotlight editors, however, remain editorially independent and solely responsible for all editorial decisions. Read more on the role and purpose of the panel here.





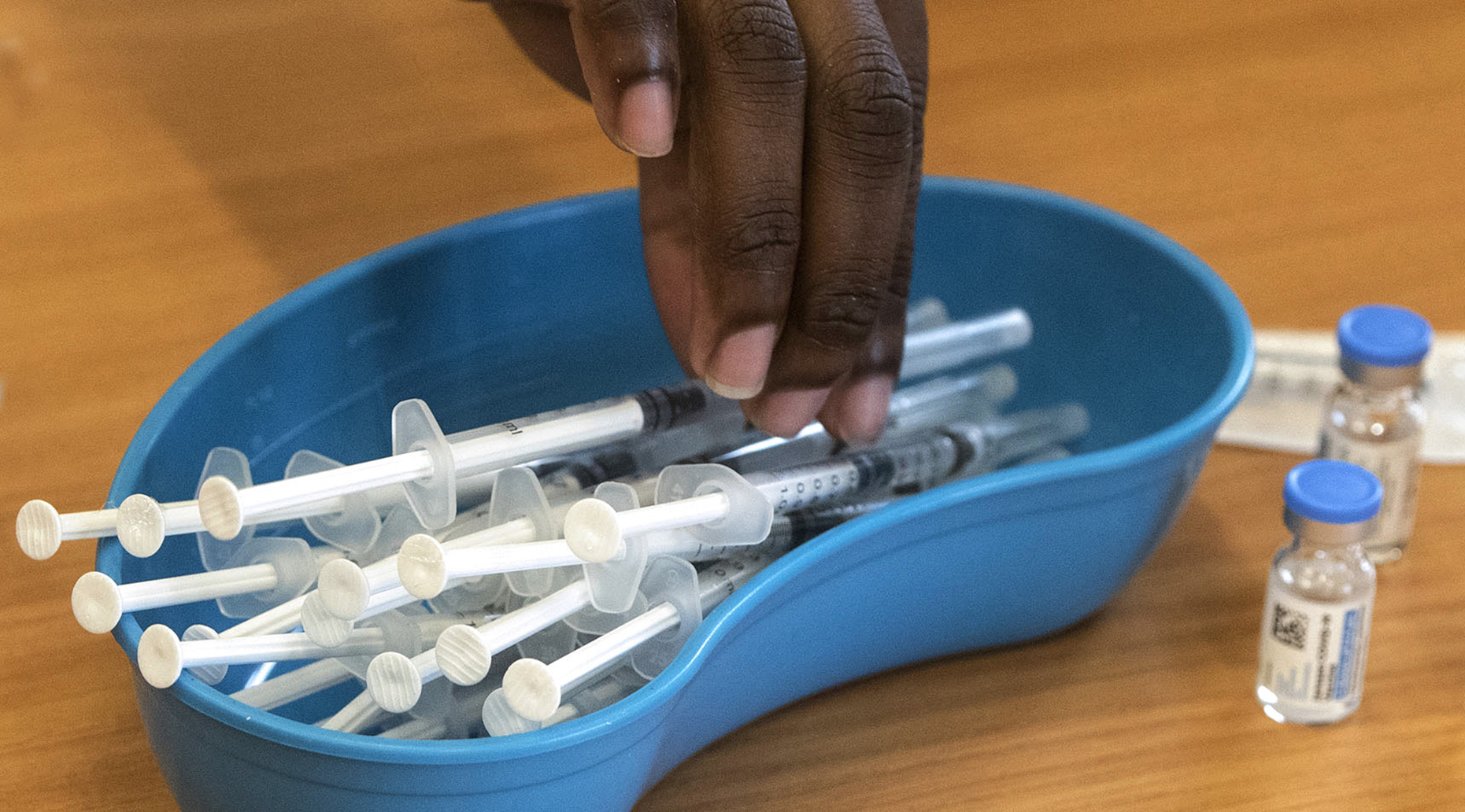 Some public health experts say the Covid-19 vaccine doses destined to be binned next month are ‘a shocking indictment’. (Photo: Gallo Images / Brenton Geach)
Some public health experts say the Covid-19 vaccine doses destined to be binned next month are ‘a shocking indictment’. (Photo: Gallo Images / Brenton Geach) 