Medical negligence not the only cause
In recent years, the country has seen a high number of medico-legal claims against government that are related to cerebral palsy. According to a 2021 discussion paper by the South African Law Reform Commission (SALRC), at the end of the 2019-2020 financial year, the total medico-legal claims against government departments amounted to R147.12-billion. Even if only a small fraction of the claims are paid out, the amounts are nevertheless large enough to significantly dent provincial health budgets.
Using data from provincial departments of health up to the 2018/2019 financial year, the Clinton Health Access Initiative’s health financing teams inferred that about “50% of all claims are cerebral palsy-type claims (birth asphyxia, neonatal encephalopathy, cerebral palsy), making up more than 60% of the liabilities in six out of the nine provinces”.
According to the SALRC paper, there is a common misunderstanding that cerebral palsy is mainly caused by birth trauma. As outlined by various experts in the previous article, birth trauma is only one of many things that can cause cerebral palsy. Indeed, the picture is much more complicated than the high number of claims would suggest.
Understaffed and under-resourced
Dr Mark Richards, a neurodevelopmental paediatrician at the University of Cape Town and Red Cross Children’s Hospital (speaking in his personal capacity), says several factors contribute to the public perception that medical incompetence and failure are the main cause of cerebral palsy.
“Big payouts from litigation, children disabled by cerebral palsy, [and] long queues at clinics all contribute to public perceptions of medical incompetence and failure. This is not the whole story, though,” he says.
“Far more common than clinical error in South Africa, are the number of events that occur because service pressures exceed our capacity to be safe. This is what is not fully appreciated in the legal process.”
One area where it seems service pressures are impacting on care is in the monitoring and documenting of births.
/file/dailymaverick/wp-content/uploads/2022/07/MC-Cerebral-Palsy-Part2_1.jpg)
Dr Stefan Gebhardt, Professor in Obstetrics and Gynaecology at Stellenbosch University, stresses that good documentation during birth events is needed. But monitoring and documenting are extremely difficult to do in scenarios where the healthcare system is overcrowded. He explains that a single midwife will only have time to properly monitor and document two women at any time during labour. So more trained staff is needed in the public sector.
“Good note keeping, including regular foetal monitoring, does not cost anything, but in an overcrowded system where one midwife or doctor has to deliver more than one patient at the same time it sometimes becomes difficult to focus on all the aspects,” he says. “So, a nursing staff ratio of 1:2 is required in low-risk labour wards. When there are high-risk women, the ratio should be closer to 1:1. This is currently unachievable in our setting due to (lack of) resources.”
Dr Thembi Katangwe, a paediatric neurologist and PhD candidate at Stellenbosch University’s Department of Paediatrics and Child Health makes a similar argument. “The ultimate solution would be to improve the quality of healthcare services provided in our state hospitals, especially perinatal care,” she says.
She adds that in order to achieve this, the country needs to employ enough qualified healthcare workers in all facilities, as well as equip these facilities properly and set up “targeted interventions to deal with the major causes of cerebral palsy in the country”.
‘Poor documentation’
Gebhardt says poor documentation plays an important role in court proceedings, as it is assumed that if something like monitoring was not documented, it was not done. Another aspect that plays an important role in court proceedings is external foetal monitoring, also known as cardiotocography or CTG. He says this is “a very unreliable form of foetal monitoring and was introduced into general care without any randomised trials ever done”.
“The incidence of cerebral palsy is still the same as it was before the introduction of CTG, so it has not made any difference,” he says.
Yet there might be better ways of detecting placental problems, according to Gebhardt. “A way of detecting placental problems during the antenatal care period may help identify babies that may have a poor outcome. There is a cheap, local invention called UmbiFlow — from the SAMRC (South African Medical Research Council) that shows a lot of promise to do this,” he says. The SAMRC’s website describes UmbiFlow as a “portable device that estimates the flow of blood in the umbilical cord”.
Lack of data, lack of understanding?
When asked if South Africa is doing enough to understand the public health burden of birth injury related to cerebral palsy, and how to address the complex determinants of this, Richards says the answer is both yes and no.
On the one hand, he says “an immense amount of work and research [are] being performed to try and improve birthing safety, respectful maternity care, service delivery, healthcare worker training in the huge and complex system of public maternity services”. He says in the Western Cape hospitals he is familiar with, “obstetricians and midwives go to great lengths to improve and respond to birth injuries in a constructive way”.
On the other hand, he says, “The difficulty… is that the capacity to provide national and provincial mechanisms to understand and respond to the complex phenomena of birth injuries is not adequate at present. We don’t have sufficiently defined and developed systems to evaluate the complex ecosystems that result in birth injuries. There are parts of the country that do this comprehensively at the local hospital or district level, but we have no nationally or even provincially mandated system that addresses individual cases of Hypoxic Ischaemic Encephalopathy (HIE) in state healthcare.”
/file/dailymaverick/wp-content/uploads/2022/07/MC-Cerebral-Palsy-Part2_2.jpg)
Richards says he has advocated for the implementation of such a system, but is not aware of any in place at present.
According to Katangwe, better data on cerebral palsy will ultimately help us identify what is contributing to the high prevalence of cerebral palsy in the country. “Updated records on cerebral palsy can easily identify the major contributors of cerebral palsy in the country and therefore assist in advocating for, as well as properly channelling the resources to deal with the preventable causes of cerebral palsy appropriately. Data availability can also provide the basis for identifying cerebral palsy cases that are truly due to medical negligence,” she says.
Some are of the view that South Africa needs to establish a cerebral palsy registry.
Dr Natalie Benjamin-Damons, a physiotherapist and lecturer in paediatric physiotherapy at the University of the Witwatersrand explains that South Africa does not have a registry to determine the number of children that develop cerebral palsy and how many survive into adulthood. Such a registry would be useful, she says, as it would provide information on how many children are born with cerebral palsy, what factors contributed, how many have access to a school and healthcare, as well as survival rates.
While such a registry does not yet exist, Katangwe says Stellenbosch University, with the University of Cape Town, have established a Western Cape Cerebral Palsy working group to establish a registry for the Western Cape. She says such registries were first introduced in high-income countries and are computerised databases that contain information on persons with cerebral palsy in a particular area.
“These registries have an important role in studying the causes of cerebral palsy, evaluating the best therapeutic interventions, assessing patients’ quality of life, and driving the organisation of healthcare services for children and adults with cerebral palsy,” she says.
Policy and guidelines
When asked what the current policies are in the public healthcare sector aimed at reducing the incidence of cerebral palsy, Gebhardt responds that there are guidelines geared towards the reduction in deaths or poor outcomes during pregnancy, but none specifically geared towards preventing cerebral palsy. One key document is the Intrapartum care guidelines. There are also the maternity care guidelines, which are currently being revised, and a maternity case record, where the birth process is documented.
/file/dailymaverick/wp-content/uploads/2022/07/MC-Cerebral-Palsy-Part2_3.jpg)
Gebhardt says as far as he is aware there are currently no plans from the government to implement a system or procedures or policies to try to reduce cerebral palsy specifically. “The general focus is on reduction of maternal deaths, stillbirths, and neonatal encephalopathy,” he says.
Spotlight contacted the National Department of Health for comment, but after almost a month received no response.
Support also needed after diagnosis
Much of the focus is on prevention and on infants, but the effects of cerebral palsy can be lifelong. Benjamin-Damons says there are children who have cerebral palsy that fall through the cracks and more should be done to find them. She adds that a culture of teamwork between the different disciplines, like paediatricians, occupational therapists, physiotherapists and educators is needed.
“Cerebral palsy in our context is far more complex than we realise and the more we understand that we each have a role to play, the better the outcome would be for the children,” she says.
“All of us… from the medical professionals to even our law practitioners, [must understand] that it’s not about getting this huge sum of money or proving our healthcare system is inefficient. It’s about ensuring that the patient is getting the best care and that the government is also in a position to provide good care,” she says.
This article was published by Spotlight – health journalism in the public interest.
Read Part One here.





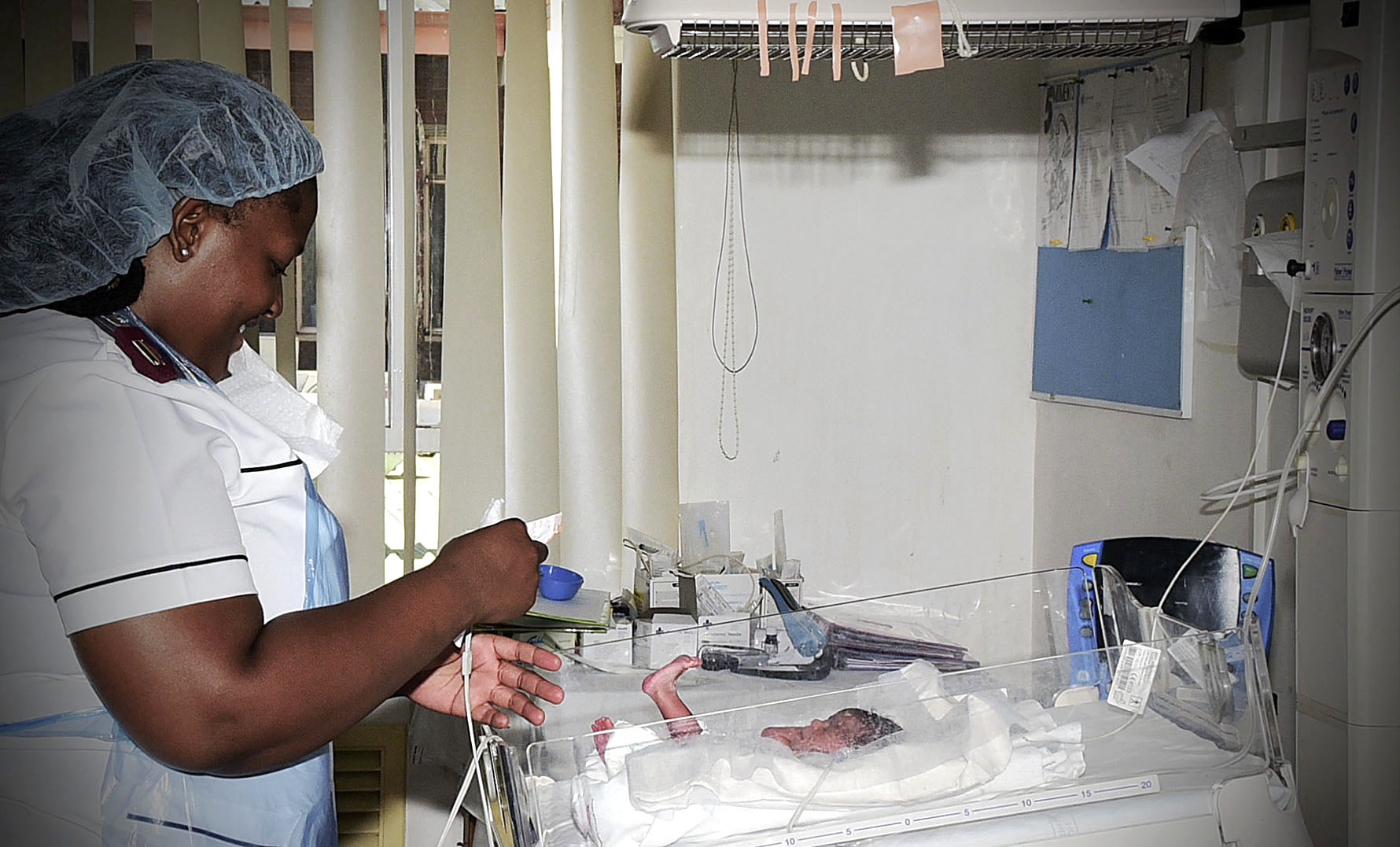 Much of the focus is on prevention and on infants, but the effects of cerebral palsy can be lifelong. (Photo: Denvor De Wee / Spotlight)
Much of the focus is on prevention and on infants, but the effects of cerebral palsy can be lifelong. (Photo: Denvor De Wee / Spotlight)