A new study by a team from the World Bank finds that to adequately care for the health of its future population, South Africa will have to substantially invest in a skilled health workforce.
The country’s increasing population, changing demographics and growing middle class are just a few of the trends that will put pressure on South Africa’s health system in the coming decades. By 2050, South Africa is expected to grow by 15 million people, and about 77% of the population will be living in cities. Economic growth will help expand the middle class, especially in urban areas, and poverty is expected to be reduced to about 30% by 2030.
At the same time, South Africa’s life expectancy is projected to increase from the current 64 to about 73 years in 2040, if HIV/Aids can be controlled. Due to out-migration of the youth, many rural people will be both poor and elderly and will be facing chronic diseases, which are increasingly affecting the poor.
Technology will transform people’s expectations for care, how care is provided, how providers are educated and how information is utilised. In 2019, more than 91% of South Africa’s population had access to a smartphone. This widespread availability to access information can increase people’s expectations for healthcare.
South Africa’s emerging market for the medical technology industry will reach $1.8-billion in 2023 and will continue to grow and facilitate learning and medical work. Data systems will advance e-health, disease surveillance and communication with consumers and providers. Technology will facilitate data collection and analysis for planning, management and responsiveness to health needs.
The World Bank study also found that Covid-19’s impact on the health workforce has resulted in exhaustion and increasing attrition, which has worsened existing health worker shortages. But the pandemic demonstrated that South Africa’s health system can change quickly.
The pandemic elicited an extraordinary response from health professionals, who mobilised innovations in education and service provision that are historically unprecedented in the country. Remote medical work and public-private collaboration became a necessity to ensure access to care for all. Lessons from the experience can inform successful practices as South Africa looks to adapt its health system to future challenges.
https://www.dailymaverick.co.za/article/2022-05-15-fuel-thieves-siphon-off-millions-from-mpumalanga-eskom-power-station/
Preparing a health workforce for the future
South Africa is expected to become a high-income country within the next decade. With economic growth, the government will generate more domestic revenue that can be invested in medical education and the health workforce. Based on the analysis of the current context, six recommendations emerge from the World Bank study:
- Invest in high-quality education and medical research
The quality of general education will need to improve substantially to ensure that the education system produces enough qualified students for health professions. In 2017, only 55% of children successfully completed secondary school. In two international comparative assessments, in 2015 and 2016, South African children ranked last among 49 countries in mathematics and reading. These outcomes need to improve to increase the number of qualified candidates for health studies.
In 2020, South Africa’s medical institutions produced about 1,800 graduates, fewer than comparator countries such as Chile, Colombia and Turkey.

South African universities would have to triple the number of medical graduates to about 5,500 annually to achieve the same output as Chile. To teach them, medical schools will have to recruit faculty internationally, including among diaspora academics. However, the government’s current plans are to increase the number to just 2,000 medical graduates annually by 2030. This is not enough to ensure care for a growing population and to replace an ageing health workforce.
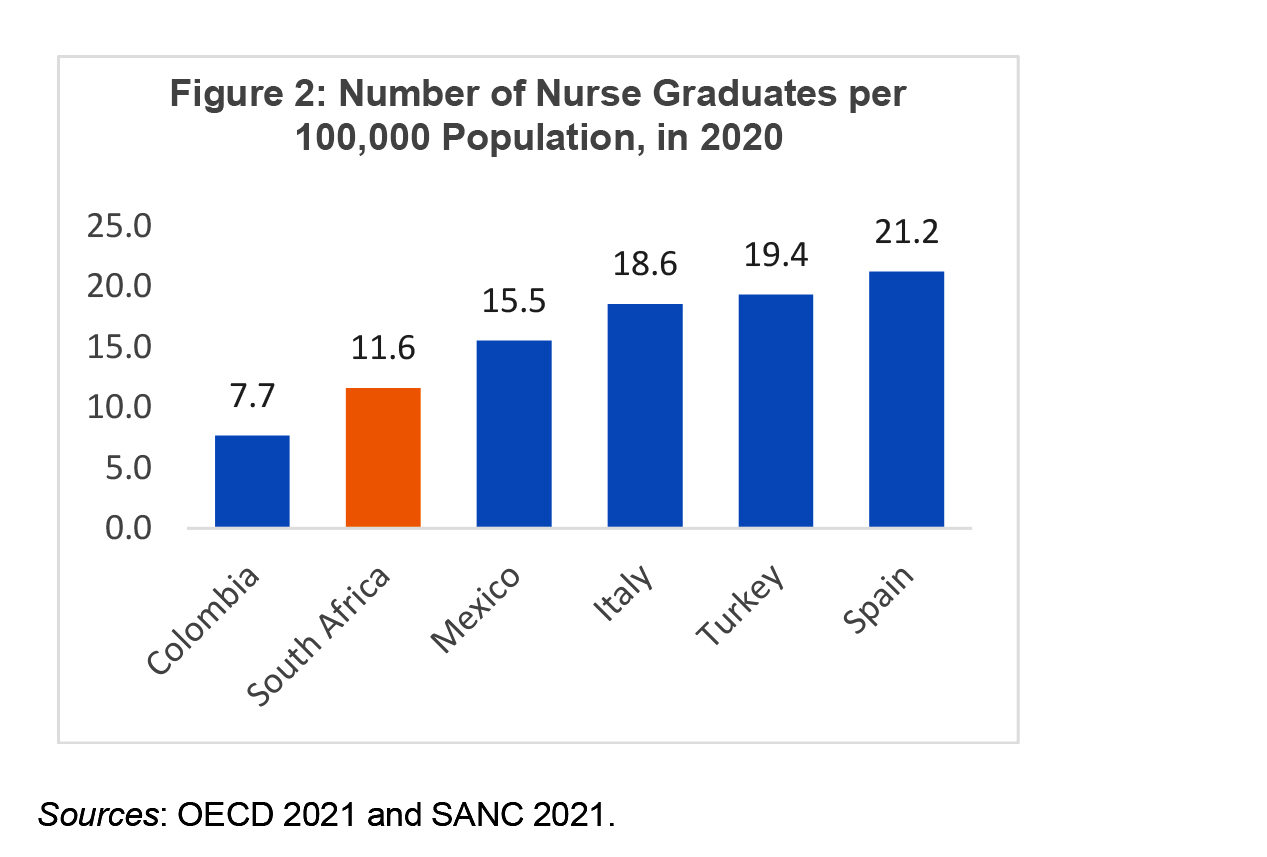
South Africa will also have to substantially increase the number of nursing schools and nurses to take care of a growing and ageing population and replace retiring nurses. About 47% of registered nurses and 29% of diploma nurses are older than 50 and will retire within the next decade. But South Africa trains fewer nurses than comparator countries such as Mexico and Turkey.
The creation of a South African techno-medical hub would attract researchers from around the world, as well as foreign research investment in genomics and technology, providing a major boost for medical research at universities. The focus could be on science, technology and innovations in health fields that are eligible for international funding.
2. Reform education financing to train more medical and health graduates
Medical education is one of the most expensive fields of study. Training a medical doctor in South Africa costs about R900,000 ($63,500). To expand high-quality medical and nursing education, more resources are needed, and they need to be spent efficiently. However, education is already the South African government’s fastest-growing expenditure category. In 2020, the government spent 19.5% of general expenditures on education, which is considerably higher than the average 11% of GDP spent by Organisation for Economic Co-operation and Development (OECD) countries.
South Africa should increase tuition fees for South African medical students, but offer them income-contingent loans (ICLs) to cover the cost, say the researchers. ICLs require students to start repaying their loans once they are earning an income above a certain threshold. For example, Hungary has no income threshold and a 6% repayment rate on full earnings, while the UK requires graduates earning over £25,000 per year to contribute 9% of their gross earnings toward the repayment of their loan.
Funding for education needs to be spent efficiently. The government should conduct a cost-effectiveness analysis of financing for students pursuing medical studies at home and abroad and their learning outcomes. Based on findings, the government should contract with cost-effective accredited medical universities abroad that could accept more medical students from South Africa.
The academic performance of health schools in South Africa should be evaluated to allocate funding. Regular independent analysis of academic programmes would make it possible to identify schools that need targeted support to improve their quality while also rewarding those that perform well.
3. Plan the health workforce based on future trends and within the resource context
The health workforce planning process should consider future trends and constraints. The Department of Health’s 2030 Human Resources for Health Strategy found there was a severe shortage of health workers to meet current needs and recommended hiring an additional 96,586 staff by 2025.
This would require recruiting among unemployed health workers, training substantially more health professionals and hiring foreign-trained health staff from countries with large diasporas (such as Ghana, Nigeria and Serbia), who could apply for a Critical Skills Work Visa. However, there are not enough unemployed health workers, training takes time and hiring foreign medical staff is almost impossible as the 2022 Critical Skills List includes only nurse educators.
High spending on wages currently limits any hiring into the sector. In 2019-20, 63% of the government’s health expenditure was on wages; to rein in this wage bill, it has largely ceased to hire additional staff to fill vacant positions. As a result, 35% of physician positions in the public sector are vacant.
To address this issue, pay scales for each position should be defined according to the objectives of the position, using measurable factors such as seniority, patient load and complexity, length and timing of shifts and location in an underserved area. Performance-based bonuses can be added for achieving an agreed set of targets.
The lack of jobs in South Africa leads many health professionals to seek opportunities abroad. Since 2002, South Africa has experienced a net loss of physicians to OECD countries, reaching about 14,000 in 2010. By 2014, this number had dropped to about 11,000 South African–born physicians.
These high emigration rates represent a loss of return on the government’s investments in medical education. To reverse this trend, legislators will need to create more health positions; increase the attractiveness of the public health system as an employer; ramp up hiring; and find ways to ensure that medical graduates will work where the need is the greatest.
4. Invest in health workforce management and the use of modern technologies
Modern personnel management practices can help increase the attractiveness of working in the public sector with effective employee promotion policies, better working conditions and opportunities for professional education and to conduct research.
Mental health services should be made widely available, including through virtual telemedicine. After Covid-19, some health professionals may not be able to work in clinical practice any more. Others may wish to acquire additional education, including working in medical informatics, data science and related technology, which the government could help to support.
Many South African students study abroad, but find it difficult to enter the health workforce at home. In 2020, a survey identified 458 foreign-trained medical graduates who were either unemployed or working in non-medical roles in South Africa because their registration with the HPCSA was still pending. The HPCSA could change hiring rules to allow foreign-trained graduates to work alongside certified physicians for up to two years, at which time they would have to pass the HPCSA exam. This is similar to a rule in Germany that defined rules for equivalency recognition of the degrees of physicians and nurses who have completed their training in non-EU countries.
An enabling environment and better understanding of technology can broaden telemedicine acceptance among the population. Nurses will need to learn how to conduct telemedicine visits from home or from virtual care centres without sacrificing their personal bonds with patients. Regulations are needed to establish the requirements for these visits and ensure access.
5. Collect data and conduct analysis to inform strategies and policies
Data will be essential for health workforce planning and management and for determining medical and health education budgets.
A centrally managed database could hold detailed information on health sector performance, the health workforce, students and graduates, as well as on the unemployed. Statistics South Africa could expand its role to collect detailed health workforce data. This could include administrative and payroll data, as well as collect disaggregated health labour data to be used in health workforce planning.
Business tax forms could also be used to capture data from private sector providers. Better data will enable regular monitoring and analysis of the sector to inform policy decisions.
6. Expand collaboration with the private sector and an international workforce
The study recommends greater collaboration with the private sector and other countries to improve access to care. With a growing middle class, demand for private sector care in South Africa will continue to grow.
Policymakers should therefore take advantage of opportunities to partner with the private sector, particularly in the provision of highly specialised care. Memoranda of understanding and contracts can set out agreed terms for the use and remuneration of private sector staff for treating public sector patients.
South Africa is fortunate in having an international health workforce, but harnessing the benefits requires measures to facilitate integration. Physicians and other health professionals should be added to the government’s Critical Skills List to prioritise their immigration to South Africa. Foreign medical staff could also be recruited through bilateral agreements with countries that already have a mobile health workforce, such as Egypt, Ghana, Mexico, Nigeria and Serbia.
The hiring process could be facilitated by introducing online recruitment and registration and by actively recruiting among diaspora health professionals working abroad. To facilitate the integration of foreign health staff into the South African health system, the government should provide them with induction and language courses and information on administrative formalities inside and outside the workplace.
The World Bank report, “The Future of Medical Work in Southern Africa”, provides further analysis and more detail on how the country can best prepare for the coming changes. DM/MC
Courtney Price Ivins is a health specialist with the World Bank’s East and Southern Africa Unit.
Annie (Liying) Liang is an operations analyst with the World Bank Group’s East and Southern Africa Unit.
Nicole Serfontein is a global health lawyer with 20 years’ experience working in the public and private health sectors on governance, finance, legislative and market strategies.
Thulani Matsebula is a senior economist with the World Bank Group’s East and Southern Africa Unit, based in Pretoria.
Pia Schneider is a lead economist with the World Bank Group, working on health reforms in Eastern and Southern Africa, Europe and the Middle East.
[hearken id="daily-maverick/9472"]




 The country’s increasing population, changing demographics and growing middle class are just a few of the trends that will put pressure on South Africa’s health system in the coming decades. By 2050, South Africa is expected to grow by 15 million people and about 77% of the population will be living in cities. (Photo: iStock)
The country’s increasing population, changing demographics and growing middle class are just a few of the trends that will put pressure on South Africa’s health system in the coming decades. By 2050, South Africa is expected to grow by 15 million people and about 77% of the population will be living in cities. (Photo: iStock)