Below are two stories that provide a window into the challenges facing overstretched health workers and the people who depend on public healthcare services.
A displaced doctor from Charlotte Maxeke hospital speaks to us. The doctor requested that we not use his/her name for fear of victimisation.
I’m one of the doctors working in the Wits circuit at Charlotte Maxeke and am currently displaced because of the fire and the subsequent closure of the hospital.
My experience of how this has impacted patients and people that I see directly has been the most notable at the oncology clinic which is currently being run out of Chris Hani Baragwanath Academic Hospital.
As a result of the closure of Charlotte Maxeke, it’s seeing all of what is called south Gauteng.... that is, all of the patients who don’t fall into the Pretoria drainage area. This means that anyone who has any malignancy, and was seen at Charlotte Maxeke or Baragwanath before, are now being seen together here.
Let me start with the obvious things.
The clinics are incredibly full... they’re incredibly busy. And many of the patients who came from Charlotte Maxeke have had a significant interruption in day care.
Many of those who’ve been on chemotherapy or receiving radiation have now gone almost three months without receiving either. Chemotherapy regimens are ones that you can’t give and then hold for a few months and then give again; the whole point is to try to deal with very actively replicating cancers.
The result is that patients have had these regimens interrupted and subsequently, in quite a few of them, the cancers have come back or they have started to develop a progression of their disease. There are also people who were in remission and who have been treated where the cancer has come back more aggressively as a result of this treatment interruption. That’s been a very, very difficult thing to see.
The second thing that’s very difficult is that the records are all at Charlotte Maxeke. A few are brought across to Bara on a weekly basis, but usually there’s a big mismatch between the patients and the records. So the right records are not always brought through, or even any records at all for some patients.
So we are often left guessing at what the patient’s chemotherapy regimens were, to the point of saying to them, “did you have the red drip or was it...?” You know, asking the patients to describe the regimens and then hazarding a best guess.
For different malignancies, there are sometimes different options of chemotherapy. You can’t just restart a different regimen, you need to — if they’ve received three cycles of one regimen — you need to continue that same regimen.
But we are genuinely sitting there with oncologists and they are guessing at what they think the person was on previously, based on very, very scanty information, and trying to restart the regimen.
Very often we end up having to say, “we can’t actually continue with treatment because we don’t know what you are on”. Sometimes we can work out what cancer it is, but sometimes we can’t because all the records are missing and you do need very particular details about the kind of cancer and what it is sensitive to.
We can usually work out what cancer it is because we can access the online lab system. But there are no digital records in terms of what the patient’s treatment was. So to these patients, who are already having treatment interrupted for two to three months, if not longer, we have to say, “we think your cancer might need to be restaged because now it’s progressed”.
And we therefore delay treatment even further.
Often they must now get another CT scan or another biopsy or something like that to restart investigating them, because things have changed in the last three months. This would obviously give them a much worse prognosis in terms of risk of recurrence and us not being able to offer any kind of curative therapy, because now you’re delaying and delaying and delaying.
So now there are further delays because we are reinvestigating and all of the places that do these investigations, like Bara, are completely overloaded with patients. So the dates given for CT scans and other investigations are pushed further and further out, which will then impact on their treatment as well.
So yes, it’s been a very disheartening thing to see.
Sibongile’s story
Sibongile Tshabalala is the national chairperson of the Treatment Action Campaign. She lives with HIV and is a veteran activist in the fight for health rights.
My aunt is Betty Nhlapo.
On Wednesday night last week, I received a call from my uncle telling me that both he and my aunt had tested positive for Covid-19. My aunt was coughing a lot and she was unable to walk.
The next morning my mom called to let me know that my aunt’s situation was getting worse. I phoned my uncle and advised him to call an ambulance, which he did at around 11.15am. After an hour, I called back and learnt that the ambulance had not arrived. I made more calls and was told that there were no ambulances for now.
They promised that as soon as one was available she would be taken to hospital.
I then decided to go and support my uncle. We drove to Daveyton from Vosloorus at around 12h30 and arrived there 45 minutes later. The ambulance still hadn’t arrived.
I called the Ekurhuleni district health manager, a Mr Magoro, to assist and he called to check why the ambulance was not coming. I know him because he used to work in the national department of health. I often call him when I am trying to get help for people in the community who have problems with the health system.
Meanwhile, we sat with my aunt who was struggling to breathe and the situation was getting worse by the minute. I was so depressed. I was scared we might lose her while waiting. It was so painful... I could see my uncle feeling powerless and not knowing what to do.
My aunt was sitting in the dark. She couldn’t even say two words. It’s so painful to know we are losing so much money in the health sector to corruption and people are dying like this. Then our politicians are saying everything’s okay. But on the ground, it’s not okay. It’s a disaster.
At just past 2pm the district health manager followed up again with the Emergency Medical Services (EMS) department. He put me on the call and a guy by the name of Mr Mahlangu lied when he said the ambulance had come and they tried to call us, with no luck. When I started to challenge him, he said the ambulance will arrive in 10 minutes. Then we waited for another 20 minutes without any luck.
Eventually, the ambulance came at around 3.30pm. They took my aunt to Far East Rand hospital and I followed them. She was admitted in casualty. When I left the hospital around 9.45pm she was still in casualty and being given oxygen. Because of the curfew we had to go home.
My aunt was taken to the ward only the next afternoon, after the intervention of the district health manager.
We tried to call the hospital but couldn’t get through all day. Eventually, they called us and told us that unfortunately, we had lost her that evening.
She was 53.
We are burying her on Thursday. My uncle is not okay. He won’t be able to attend her funeral.
This situation is not good. We were promised a better house and a better life. But look how we live. They had a three-room house; it’s very small. Now my uncle is in quarantine in one bedroom. We take him out once a day to fumigate the room and the house. This is not what we were promised. My heart is very sore. DM/MC





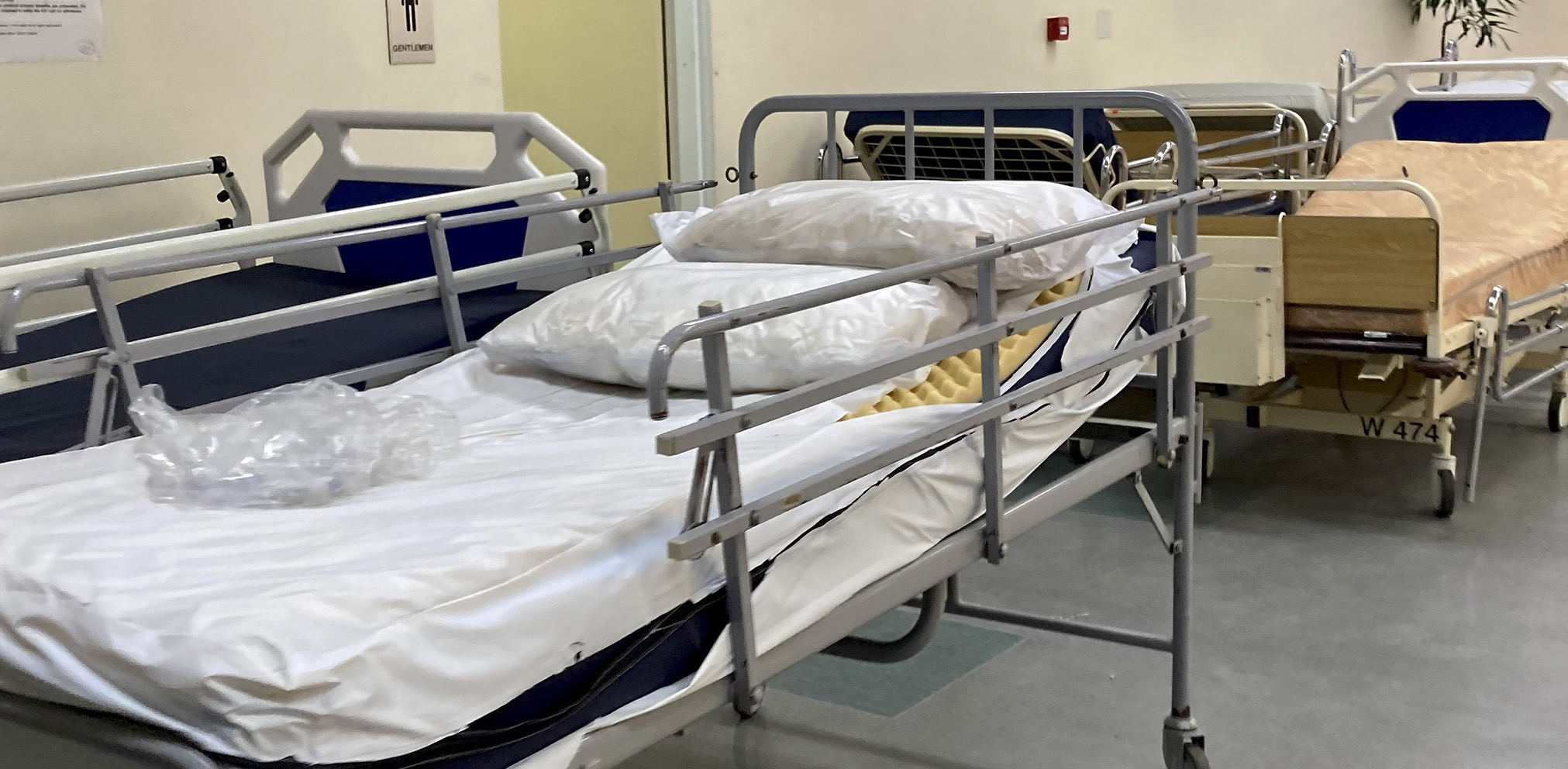 Stray plastic and refuse lies on the beds lined up along Hospital Street at Charlotte Maxeke Johannesburg Academic Hospital. (Photo: Supplied)
Stray plastic and refuse lies on the beds lined up along Hospital Street at Charlotte Maxeke Johannesburg Academic Hospital. (Photo: Supplied)