Imtiaz Sooliman is the founder of Gift of the Givers
Gauteng is in great difficulty.
This is evident from the calls to us of desperation from medical professionals, families and patients. The overwhelming request is for oxygen concentrators, oxygen cylinders and oxygen, or bed availability at hospitals.
Both private and public hospitals are filled to capacity.
Beds are very difficult to come by. Patients travel from hospital to hospital to try to find an emergency department that is not busy. Once there, patients wait for hours before they can get access to a bed. The lucky ones get admitted, but the rest are sent home.
What is the problem?
In a nutshell, it is staff shortages that have not been addressed during both waves. Given the huge effect of the third wave, healthcare workers are going to get burnt out very rapidly. In addition, there are water challenges at some hospitals.
Because of the situation at hospitals, general practitioners, physicians and allied health professionals are intensifying home-based care, providing a service as best they can. There are limitations as bigger oxygen flows are required as patients get progressively worse.
An immediate solution is to open Charlotte Maxeke hospital. While it is understood that the burnt section is unsafe, apparently structural engineers have said that many parts of the hospital are fine. This has to be verified as I don’t have access to any reports, but I have had first-hand accounts.
At its peak, Charlotte Maxeke can take care of 300 Covid-19 patients. It has excellent ICU facilities.
The public needs a rational explanation as a matter of urgency as to why it is two months since the fire burnt through the hospital and yet this important facility is not functional at the height of the third wave of Covid-19.
From what I’ve been told, Hillbrow hospital is only functioning at 40% capacity. Why can’t this facility be upgraded to increase bed capacity?
There is information that dedicated facilities for Covid-19 were built at huge cost at Chris Hani Baragwanath hospital and are not being used. This needs to be investigated and verified as bed space may be available.
I have heard that a hospital built in Kempton Park has been closed for two decades. It has been vandalised. This is another potential facility to be upgraded to increase bed capacity.
Upgrades can be partial and focused specifically for Covid-19. This will require bulk oxygen supply, oxygen points, oxygen machines, beds and some cosmetic touch-ups with good ablution blocks. ICU is an optional extra given the time constraints.
If adequate oxygen is timeously provided through all these additional facilities, steroids are used judiciously and the normal Covid-19 management protocols are applied, lung damage can be minimised and the need for ICU substantially reduced.
Nursing staff are required, but, fortunately, paramedics can also make a huge difference. At Livingstone Hospital, Gift of the Givers has been funding eight nurses and 19 paramedics since last year. It has been an incredible success.
Gift of the Givers delivered 2,500 CPAP ( continuous positive airway pressure) machines last year to various hospitals in six provinces in 10 days. These machines utilise oxygen at between 10 to 30 litres per minute and the results are excellent — we can see patients improve.
This was a life-saving intervention that we can now deploy.
These machines are far more efficient than oxygen concentrators, nasal prong oxygen, face masks and, in some cases, equally efficient to high flow nasal oxygen machines that use 60-100 litres of oxygen a minute. The CPAP machines were designed and manufactured in South Africa and funded by the Solidarity Fund.
Gift of the Givers has written to the Solidarity Fund asking for an additional 600 of these CPAP machines and 200 units of an advanced version called Save-P immediately.
We will offer this free of charge to any public or private hospital which agrees to increase Covid-19 bed space, along with lending two ambulances to the province. They will get one machine for each bed space created.
Doctors have reported that oxygen concentrators are out of stock and we have sent a batch to Johannesburg, with more to follow.
Many other organisations are also working extremely hard to provide these concentrators. They give a patient a chance to recover or buy time while waiting for a hospital bed.
To deal with water cuts at hospitals, the borehole at the Rahima Moosa hospital is now working with a capability of providing 18,000 litres a day, while at the Helen Joseph hospital, our teams found the capability to provide 1,500 litres per day at 240m deep.
We are currently drilling at a second site. DM





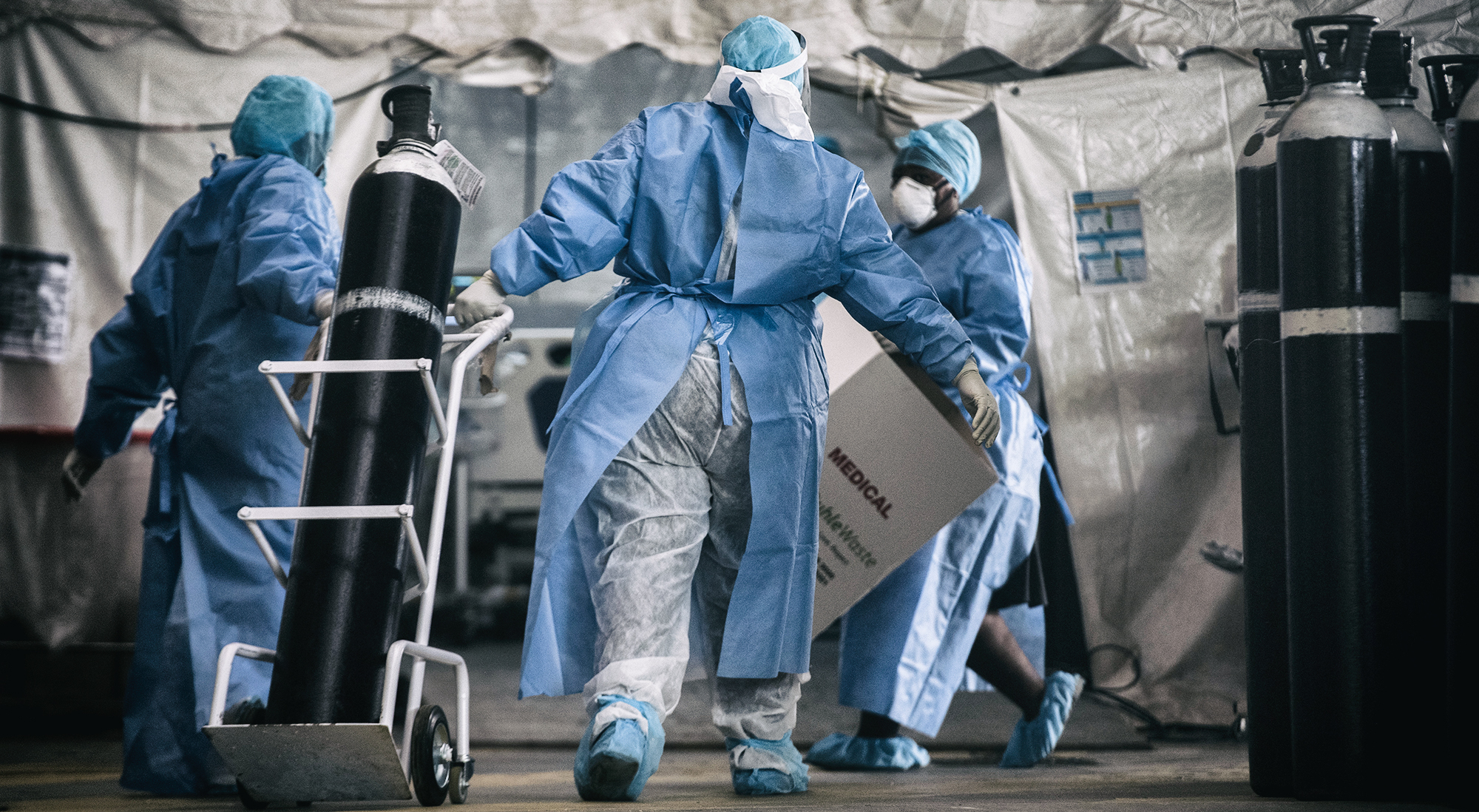 The overwhelming request in Gauteng is for oxygen concentrators, oxygen cylinders and oxygen, or bed availability at hospitals. (Photo: Gallo Images / Alet Pretorius)
The overwhelming request in Gauteng is for oxygen concentrators, oxygen cylinders and oxygen, or bed availability at hospitals. (Photo: Gallo Images / Alet Pretorius)