World Cancer Day, spearheaded by the Union for International Cancer Control, takes place every year on 4 February and is a unifying initiative under which the global community comes together to elevate the profile of cancer in a positive and encouraging manner. In 2021, the theme “I Am and I Will” encapsulated the extraordinary spirit and the strength of the people working in the cancer community.
Cancer continues to affect us significantly and as we commemorated this day, we reflected, acknowledged and recognised that the continued battle against cancer is not a singular effort; a consolidated response is inescapable to ensure a path to victory. Everyone can play a role in ensuring our success.
As we look towards further advancements in the field of cancer in the current year, we cannot but reflect on the havoc, challenges, and the implications that the Covid-19 pandemic has brought in 2020. Cancer organisations globally have faced difficulties in maintaining life-saving services, not only due to a drop in resources but also because of the necessary measures enacted to contain the spread of the coronavirus and fears of contagion on the part of patients. Reports over the past year highlight exacerbated shortages in frontline staff, sometimes redirected to the Covid-19 response; interruptions and delays in prevention programmes, diagnostics and testing, clinical trials and research; difficulties in engaging in community outreach with restrictions on travel and social gathering; and greater barriers to accessing essential medicines in low- and middle-income countries.
For the cancer community, these have been testing times. Patients’ access to diagnostics, treatment and care has been hit in many ways, and have found themselves often isolated – in clinical consultations and in their daily lives – at a time when they most needed support. Oncology professionals, who are trying to do their best while lacking the evidence to define “best care” in the Covid-19 setting, are working within health systems ill-prepared to deal with the high number of virus-infected patients. This, at a time when physical distancing made normal professional collaboration and patient care more difficult and when many healthcare staff struggled with access to the personal protective equipment and testing needed to keep them and their patients safe.
Despite the vast problems, we applaud the heroism of our nurses, doctors, researchers, volunteers, advocates and other caregivers in oncology from around the world who held the frontline over the past 12 months through the Covid-19 pandemic, understaffed and underequipped, at a great cost to their health, mental health and too often, their lives.
A year later and we are now starting to see how organisations and healthcare workers are rallying across the globe to support patients, resume screenings and diagnostics, maintain awareness on the need for prevention and provide a safe environment for treatment. Volunteers have mobilised to deliver medication and even food to patients in need or ensure transportation to care centres.
The private sector is developing innovative technologies to reduce the time spent in care settings while maintaining quality of treatment. Digital technology is allowing doctors and research centres to collaborate and share knowledge at a global level, accelerating the move towards greater patient-centred care.
We have begun integrating everything we’ve learned about using information technology to communicate, collaborate and teach remotely, and about the value of interdisciplinarity – looking for answers among classic “repurposed” or innovative molecules developed for other diseases; virologists and oncologists learning from one another.
And at a time when face masks and distancing are putting up additional barriers, it invites health professionals, not least in oncology, to identify more closely with their patients, recognising that the sense of fear and vulnerability in the face of a disease that we don’t fully understand, or know how to treat, or even how to avoid, is common to us all.
We certainly live in interesting times that can be seen as somewhat of a paradox. The oncology field has been undergoing a permanent revolution over the past three decades. Molecular diagnosis and new imaging modalities have transformed clinical practice. We have seen the implementation of hormonal and targeted therapy, immunotherapy, CAR T cell technology, genetic engineering, enhanced radiation therapy and nuclear medicine – all of these with great advantages but also non-negligible toxicities.
The digital revolution has brought us big data (data science) and eHealth technology. We now interrogate our genetic background, and sequencing and ’omics are in day-to-day use. We measure our health using a proliferation of smartphone apps – not all of them endowed with the same quality or reliability.
However, with these advances, costs have risen progressively, leading to therapies becoming less affordable and wide disparities in access emerging along geographic, ethnic, gender, age and socioeconomic lines.
Living longer frequently entails many years of poor health in later life, and often also loneliness – cancer is a disease of the whole body: organ, microenvironment, and the soul, as we know that the health, wellbeing and happiness of cancer patients depend on many factors beyond diagnosis and therapy. So we need to not only give more emphasis on predictive, preventive and personalised medicine approaches, but also participatory, and with a psycho-oncology dimension.
The global cancer burden of cancer is estimated to have risen to 18,1 million new cases and 9,6 million deaths in 2018. One in five men and one in six women worldwide develop cancer during their lifetime, and one in eight men and one in 11 women die from the disease. Unless greater efforts are placed into altering the course of the disease, this number is expected to rise to close to 30 million new cases by 2040.
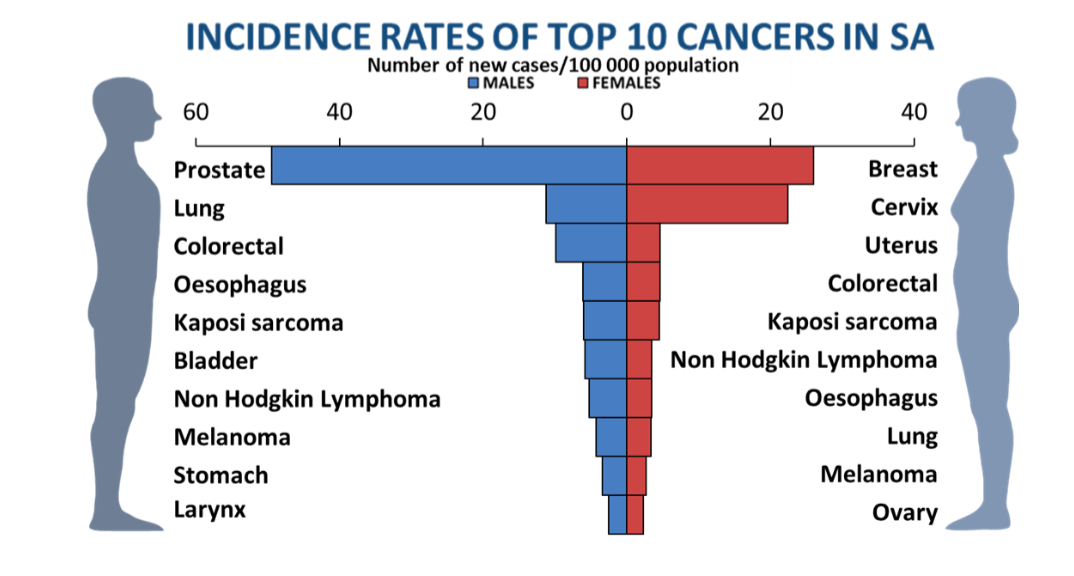
With South Africa’s growing population of approximately 59.6 million and an ageing population, the caseload is expected to double by 2040 as well. Cancer remains the sixth main cause of mortality in South Africa and latest data from the National Cancer Registry reveals that in 2017, at least 81,607 new cases were diagnosed. Cancers of the breast, cervix and prostate continue to dominate, with a similar profile extending into Africa.
It is important to note that about 30% of cancer deaths are due to the five leading behavioural and dietary risks, that is, high body mass index, low fruit and vegetable intake, lack of physical activity, tobacco use, and alcohol use. Many cancers can be prevented by avoiding exposure to these common risk factors.
In addition, a significant proportion of cancers can be cured – by surgery, radiotherapy or chemotherapy – especially if they are detected early. There is an urgent need to increase early-stage cancer detection, screening, and diagnosis to significantly improve cancer patients’ chances of survival and quality of life. When a cancer is detected at an early stage – and when coupled with appropriate treatment – the chance of survival beyond five years is dramatically higher than when detected at a later stage when the tumour has spread, and the disease is more advanced. Furthermore, early diagnosis can also reduce the cost of treatment.
Despite this, millions of cancer cases are found late, leading to expensive and complex treatment options, diminished quality of life, and avoidable deaths.
There is no “one” solution to the country’s cancer problem. Barriers exist at the individual, health system, and government level, which prevent millions of people globally from receiving an early diagnosis and better treatment. There are huge disparities in health resources (infrastructure, human resources, access to treatment) that make populations in Africa, including South Africa extremely vulnerable to developing and treating cancer.
Therefore, continued efforts in strengthening the capacity of the health sector, improving access to treatments and supportive services remain core to curbing the rising epidemic of cancer. DM
Professor Vikash Sewram is the Director of the African Cancer Institute in the Faculty of Medicine and Health Sciences at Stellenbosch University.




 (Photo: Unsplash / Angiola Harry)
(Photo: Unsplash / Angiola Harry)