BHEKISISA OP-ED
Rape increases the long-term risk of contracting HIV – an issue South Africa must take seriously
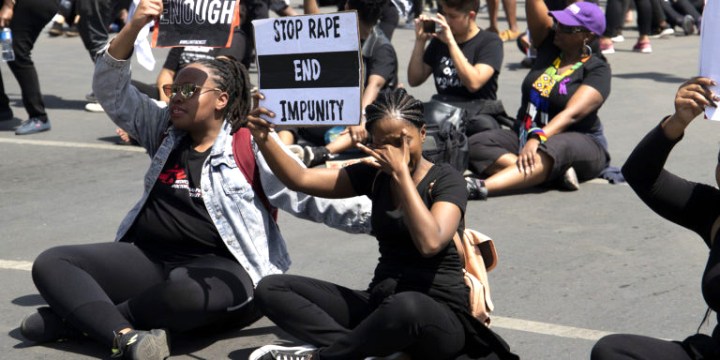
Trauma care for rape survivors has been crucially underfunded and the evidence of the HIV-related consequences is staggering.
The Rape Impact Cohort Evaluation (RICE) study, the results of which were released this week, revealed that female rape survivors were 60% more likely to contract HIV over a period of up to three years after their rape than women who had not been raped.
The 1,019 women included in our research were between the ages of 16 and 40 and had all attended either a rape support centre or a primary healthcare facility in the greater Durban area.
Our findings are important because until now post-rape health services have mostly focused on preventing the risk of immediate HIV acquisition — in the course of the rape — as opposed to addressing survivors’ risk of contracting HIV over an extended period of time afterwards.
To the best of our knowledge, this is the world’s first study to follow rape survivors for up to three years after their rape and then compare their risk of HIV infection with that of a control group.
The implications of our study’s results for the need to provide long-term, comprehensive care and support for rape survivors are considerable as they are more costly and complex to implement than short-term HIV prevention care.
To decrease someone’s chances of becoming infected with HIV immediately after a rape requires a 28-day course of antiretroviral drugs — known as post exposure prophylaxis (PEP) — that is initiated within 72 hours of the rape incident. The intervention is not without challenges, not least because poor adherence of PEP post rape is well documented.
But addressing the long-term mental health effects of rape trauma, which are likely drivers of survivors’ increased risk of HIV infection over time, is an entirely different story.
Survivors of rape have a uniquely high risk of developing and enduring post-traumatic stress syndrome (PTSD). Depression, substance abuse and suicidality often accompany PTSD and between a quarter and a third of rape survivors continue to have PTSD symptoms six months after the rape.
The psychological pain caused by the trauma of rape is too often compounded by blame and stigmatisation stemming from the families and communities of rape survivors. Internalised shame and self-blame also play roles. These are compounded by symptoms of anxiety and depression as a consequence of rape, and – all too commonly in South Africa – pre-existing symptoms from prior experiences of trauma.
Anxiety, depression, PTSD, shame and self-blame can all massively compromise survivors’ ability to negotiate safety in sexual encounters. Such untreated mental anguish can also lead to self-medication via heavy drinking or drug use — again increasing HIV risk in sexual situations. In addition, the combination of incapacitating mental distress and social stigma from being a rape survivor can compromise employment and other economic opportunities, potentially increasing risky survival sex. The same risk patterns were described in research showing the causal pathway between intimate partner violence (IPV) and HIV infection.
But in South Africa, few rape survivors have access to the long-term mental health services they need to break these patterns.
Although post-rape care in the country has improved for survivors who are able to access Thuthuzela Care Centres (TCC), the South African Medical Research Council’s (SAMRC) 2012 research report on rape across South Africa showed that fewer than a third of survivors were able to access such centres. Most post-rape care is still delivered in the emergency departments of district and regional hospitals, without dedicated funding, support or training for the medical staff who provide frontline care to rape survivors.
Even within TCCs, more needs to be done in providing sufficient mental healthcare.
Alongside accelerating court proceedings and improving conviction rates, a key goal of TCCs is to decrease secondary victimisation of survivors, such as being stigmatised because of their rape. The delivery of these services is the responsibility of the Department of Social Development which, in turn, uses under-resourced non-government organisations (NGOs) to provide the necessary psychosocial care.
The NGOs employ lay counsellors to provide counselling, which largely takes the form of crisis management. This typically includes allowing the survivor to talk about the rape, containment of feelings and preparing survivors for procedures they will likely undertake, such as forensic examinations and providing statements to police. Referrals to other services are covered in this partnership, but this is often where psychosocial care for most survivors ends.
In 2015, the SAMRC assessed the capacity of mental health services in the Western Cape for rape survivors in acute care services and found poor integration of mental health services into post-rape care for survivors. Often, survivors were referred to their nearest community health centres (CHC) for continuation of care, but without any monitoring to ensure that care actually continued, or assurances that the CHC had the capacity to provide long-term trauma care. Indeed, most CHCs didn’t have the ability to provide such a service. Essentially, referral amounted to passing the buck.
It’s therefore no surprise that a 2016 review of the TCC model concluded that “there are serious concerns about the ability of TCCs to provide long-term psychosocial support”.
Rape survivors need varying forms of support and care, but with PTSD symptoms persisting in almost one in three rape survivors, there are hundreds of thousands of survivors who need psychological support. Based on the number of rape cases recorded by SAPS between April 2019 and March 2020, and the levels of under-reporting that research studies have established, an estimated one million rape incidents took place in South Africa in the 2019/2020 reporting year. We calculated this number by using the 42,289 reported rape cases for 2019/2020 multiplied by 25. A 2012 community-based survey in Gauteng revealed that only about one in 25 women who were raped reported it to the police.
Providing care for rape survivors is complex as their lives are often in flux; services therefore need to be flexible. Nonetheless, the SAMRC’s 2015 review of mental health service use in the month after rape in the Western Cape, showed that women who received long-term counselling services from a specialist NGO generally had the best understanding of post-rape mental health and mostly continued attending counselling sessions, despite barriers such as transport and having to take time off work.
So why doesn’t South Africa care more about rape survivors’ mental health?
The answer is deeply embedded in gender inequality in the country, where survivors are often blamed for rape by community members while men accused of rape are defended by their families and friends.
Optimising post-rape care has not been a political priority.
Much of the funding for health services after rape has been mobilised to prevent HIV transmission during rape by providing PEP, which is simpler and cheaper than addressing the full set of rape survivors’ needs.
Given South Africa’s history of both collective and individual trauma, the country should be leading the world in offering trauma-informed care, guided by research. Our inability to do so is an outstanding failure of the health sector and a sad legacy of underfunded mental healthcare.
Over the past decade, global evidence from low- and middle-income countries, including South Africa, has shown that lay providers, closely supported by professionals, can be trained to provide effective, accessible psychological services that reduce psychological stress, relieve symptoms of mental illness and decrease harmful drug and alcohol use that can lead to risky sexual behaviour. The evidence from humanitarian and conflict settings shows delivering such care is achievable in difficult situations and reveals how far behind South Africa has dropped in not prioritising effective mental health care for trauma survivors in the public health system.
The new evidence from our RICE study is an urgent wake-up call: the rape policy and clinical management guidelines of the health department must be revised and updated to include evidence of the need for long-term psychosocial care. A true multisectoral approach to post-rape care must be initiated immediately.
The South African National Strategic Plan (NSP) on gender-based violence and femicide provides the strategic framework for the health department to come to the party and do right by rape survivors. Healing is a key component of the six pillars in the NSP and using the evidence of the impact of rape on women’s health will make “healing” more than just an empty phrase in the NSP. DM
Naeemah Abrahams, Rachel Jewkes and Kristin Dunkle are senior researchers at the Gender and Health Research Unit of the South African Medical Research Council.
This story was produced by the Bhekisisa Centre for Health Journalism. Sign up for the newsletter.



















 Become an Insider
Become an Insider
Comments - Please login in order to comment.