Maverick Citizen Op-Ed
Drug-resistant infections: The silent pandemic that must be tackled now
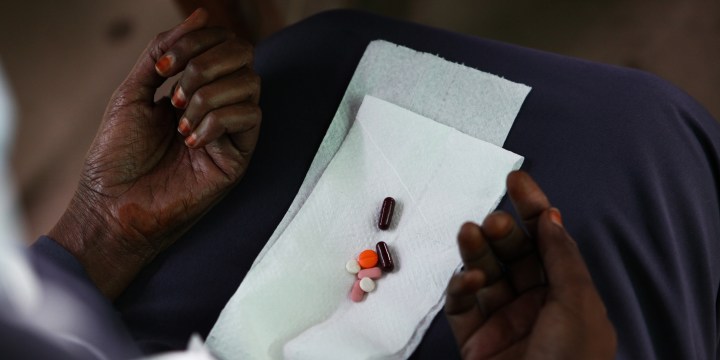
The unchecked growth of drug-resistant infections is a silent pandemic with long-term implications for global health security. As the world reels from the impact of Covid-19, it would be a tragedy not to apply the lessons we are learning to the fight against drug resistance.
Drug-resistant “superbug” infections kill an estimated 700,000 people a year worldwide, a number set to rise exponentially as drug resistance grows and weakens our ability to treat even common infections.
A worrying number of infections are becoming harder – and sometimes impossible − to treat due to drug resistance.
The consequences of not addressing the silent pandemic of drug-resistant infections now could result in a future where we are unable to treat common infections like pneumonia, urinary tract infections and infections in newborns.
Africa is in a particularly precarious position. The continent has the largest burden of endemic diseases, such as HIV, TB and malaria and is faced with emerging infectious pathogens and a growing threat of antimicrobial resistance (AMR).
In a recent commentary, the Africa Centres for Disease Control and Prevention (Africa CDC) warned about the rising threat of AMR, given that AMR will cause an estimated four million deaths in Africa by 2050.
The cost of failing to adequately prepare for Covid-19 has been a global wake-up call and raised concerns about emerging pandemics, including the pandemic of AMR.
If Covid-19 has taught us one important lesson, it is that pandemic preparedness requires a global coordinated effort, and no country can do it alone. Out of this tragedy, we can mobilise and take collective responsibility to prevent a catastrophe of AMR. Strong leadership, collaboration and investment in measures to fight drug resistance will be pivotal.
Strengthening our ability to fight drug-resistant infections requires a sustained, coordinated response, which must also ensure affordable access to solutions. Particularly critical to tackling drug-resistant infections is the One Health concept, recognising the importance of connecting the health of people to both the health of animals and our shared environment.
With the ever-present threat caused by the overuse and misuse of antibiotics, South Africa is playing its part to step up to the challenges of AMR.
In October 2019, South Africa’s health minister, Dr Zweli Mkhize, signed the Antibiotic Guardian Pledge, in which South Africa seeks to be a global leader in antibiotic stewardship. This is vital to conserve the efficacy of antibiotics currently in use and to delay the progression of AMR.
Sustainable access to effective antibiotics remains a key challenge in the country, while far more investment is needed.
Research is also vital.
The South African Medical Research Council (SAMRC), through its extramural programme, is conducting and funding research on AMR.
The SAMRC Centre for the Study of Antimicrobial Resistance (CAMRA) consists of a multi-disciplinary team of national and international experts focused on addressing specific aspects of bacterial multidrug resistant pathogens, including tuberculosis.
The SAMRC has established several partnerships with local and international organisations to collaborate on AMR research & development, including with the Global Antibiotics Research and Development Partnership (GARDP), a not-for-profit organisation developing new treatments for antibiotic-resistant infections that pose the greatest threat to health.
The SAMRC was one of the seed funders for GARDP.
South Africa is one of four countries involved in a global GARDP phase 3 trial to assess the efficacy and safety of a novel antibiotic called zoliflodacin, the only drug being developed specifically to treat gonorrhoea, a curable sexually transmitted infection.
As a first-in-class treatment, zoliflodacin is active against drug-resistant strains of gonorrhoea. Every year, there are 87 million new gonorrhoea infections globally.
GARDP is also involved in efforts to combat the growing problem of neonatal sepsis. More than 214,000 babies across the world die each year from drug-resistant infections. Babies are particularly vulnerable, as their underdeveloped immune systems struggle to fight infections.
GARDP and partners have completed one of the largest ever studies on the care of babies with sepsis.
The study, which has looked at over 3,200 newborns in 19 sites across 11 countries, including in three public hospitals in South Africa, will provide evidence to fill knowledge gaps and help transform treatment.
Working together on these kinds of partnerships is key to tackling health threats and providing life-saving treatments. It’s also in tune with CDC Africa’s call for a new public health order to cope with 21st century disease threats, including AMR.
Committed partnerships between all players across the continent – from doctors, scientists and researchers to governments and policymakers – will be needed to overcome our challenges.
The evolving pandemic of drug-resistant infections has the potential to cripple the world in the same way that Covid-19 has done this year. However, unlike with Covid-19, we know what it will take to combat drug resistance.
With sufficient political will and resources, there is an opportunity now to significantly step up our response to drug-resistant infections and prepare ourselves to handle the unpredictable and silent nature of the pandemic.
The fight against drug-resistant infections will rely on governments and other partners seizing this opportunity to develop a more robust, coordinated and equitable approach to pandemic preparedness and global health security.
Our success in fighting this pandemic will depend on the motivation now to secure investment and ensure access to solutions like better surveillance of resistant infections, tests to identify resistance and treatments like novel antibiotics. DM/MC
Glenda Gray is the President & CEO of the South African Medical Research Council (SAMRC) and is on the Board of Directors for the Global Antibiotic R&D Partnership (GARDP)
Carol Ruffell is Head of the Joint Office Southern Africa for the Drugs for Neglected Diseases initiative (DNDi) & Global Antibiotic R&D Partnership (GARDP)















 Become an Insider
Become an Insider
Dear Dr Gray, thank you for highlighting this very scary future reality. It makes me wonder about the state of the developing immune systems right now in the millions of children being over-sterilised, social distanced and masked all day every day at school – those that are fortunate enough to actually be attending school at all. Surely this is completely counterintuitive considering the necessity of constant immune stimulation necessary for good long term health. Children are the lowest of the low in risk of being ill as well as spreading Covid 19 so why are we doing them such a disservice? And also undermining the spread of immunity through our communities which will ultimately be protective of the more vulnerable? Healthy immune systems means healthy pregnant mothers and more transferring of maternal antibodies to baby and therefore less neonatal sepsis and deaths? As a medical person and parent I feel quite disturbed by the impact of our response to this virus on the physical and mental health of our children in the short and long term. It simply doesn’t make sense.