Patients that have TB are at greater risk of developing severe Covid-19, and in turn Covid-19 may worsen TB treatment outcomes. As much of the world waits with bated breath for an effective Covid-19 vaccine, bacille Calmette-Guerin (BCG), a vaccine that’s been used since 1921 to prevent TB, is now being tested to help alter the course of the Covid-19 pandemic.
Why do people still fall ill with TB when there is a vaccine? One of the main reasons is that the BCG vaccine given after birth provides poor protection against TB disease in adolescents and adults. BCG is now being tested in a clinical trial to see whether giving it will prevent TB infection in those age groups. As a physician and researcher who’s devoted most of my life to the prevention and treatment of TB, I am looking on with interest at this renewed enthusiasm towards the only vaccine currently available for TB. As this year’s Covid-19 pandemic has brought to the fore, prevention is key when it comes to a disease that easily spreads from one person to another.
Although the development of new TB vaccines has been identified as a priority by the World Health Organisation (WHO), the reality is that we are years away from newer, more effective vaccines. In the meantime, though, we have other tools we can deploy to prevent TB disease from occurring or to treat it when it does occur.
Very exciting news was reported at the 51st Conference on Lung Health, which took place last week and centered on the theme of advancing prevention. Researchers reported that combining one of the antibiotics (rifapentine) used in the three-month TB preventive therapy regimen with three other antibiotics can reduce the duration of treatment for TB disease from six to four months. These results highlight that use of rifapentine is a game-changer for both treatment and prevention of TB disease.
Up until now, a long course regimen of a single antibiotic (isoniazid) for six months has been used to treat TB infection. New, short-course TB preventive therapy regimens, using a combination of isoniazid and rifapentine, given weekly for three months, are becoming available globally. By giving anti-TB drugs to people with dormant TB infections, we can prevent them from developing active TB disease in the first place, and the shorter regimen is associated with better treatment completion and fewer side effects.
Unfortunately, lockdowns implemented to contain the spread of Covid-19 have inadvertently introduced barriers to accessing health services, limiting TB diagnosis, treatment and prevention services. A modelling study released by the Stop TB Partnership in March this year found that the response to the Covid-19 pandemic could lead to 6,3 million more people becoming ill with TB by 2025, and 1,4 million more deaths from the disease over the same period. At least five years of hard-won progress in our TB response are expected to be lost.
The onslaught of Covid-19 has been compared to being in a war. We know from World Wars I and II that TB rates spiked as healthcare services were disrupted and resources were diverted to other sectors. Already, we’ve seen reductions in TB case notification during Covid-19, leading to ongoing disease transmission as undetected cases cannot be identified and treated. It is possible to end the TB epidemic, but it will take herculean effort, and as soon as we relax our efforts, the situation will worsen. We can’t drop our guard, we must push to implement effective TB interventions, particularly TB preventive therapy that shields those most at risk of developing TB disease.
It shouldn’t be a question of prioritising resources for either TB or Covid-19 – we must find a way to deal with both. Already, we are seeing some countries starting to integrate screening and testing for TB with Covid-19 contact tracing and testing.
Advancing TB prevention needs to become our motto. The world is on track to meet the United Nations targets of starting 30 million people on TB preventive therapy. Until now, the long, six-month course of TB preventive therapy has been used to reach those targets. By using short-course preventive therapy regimens, we can prevent TB in even more people as they are more likely to complete the treatment. Encouragingly, high TB burden countries, such as Pakistan, Zimbabwe, Kenya and Ethiopia, have already ordered or started scaling up short-course TB preventive therapy regimens, and more countries, such as South Africa, Uganda, Lesotho and Zambia are poised to start national roll-outs.
While Covid-19 is front page news, now is not the time to be complacent about TB. We must renew our efforts to prevent this long-standing disease if we want to save lives. And we must re-energise ourselves to meet the commitments made at the 2018 United Nations General Assembly to scale up TB preventive therapy to help end the TB epidemic. DM/MC
Prof Gavin Churchyard is a specialist physician, internationally renowned for his contributions in tuberculosis (TB). He is the founder and CEO of The Aurum Institute, which focuses on TB and HIV service delivery, management and research.




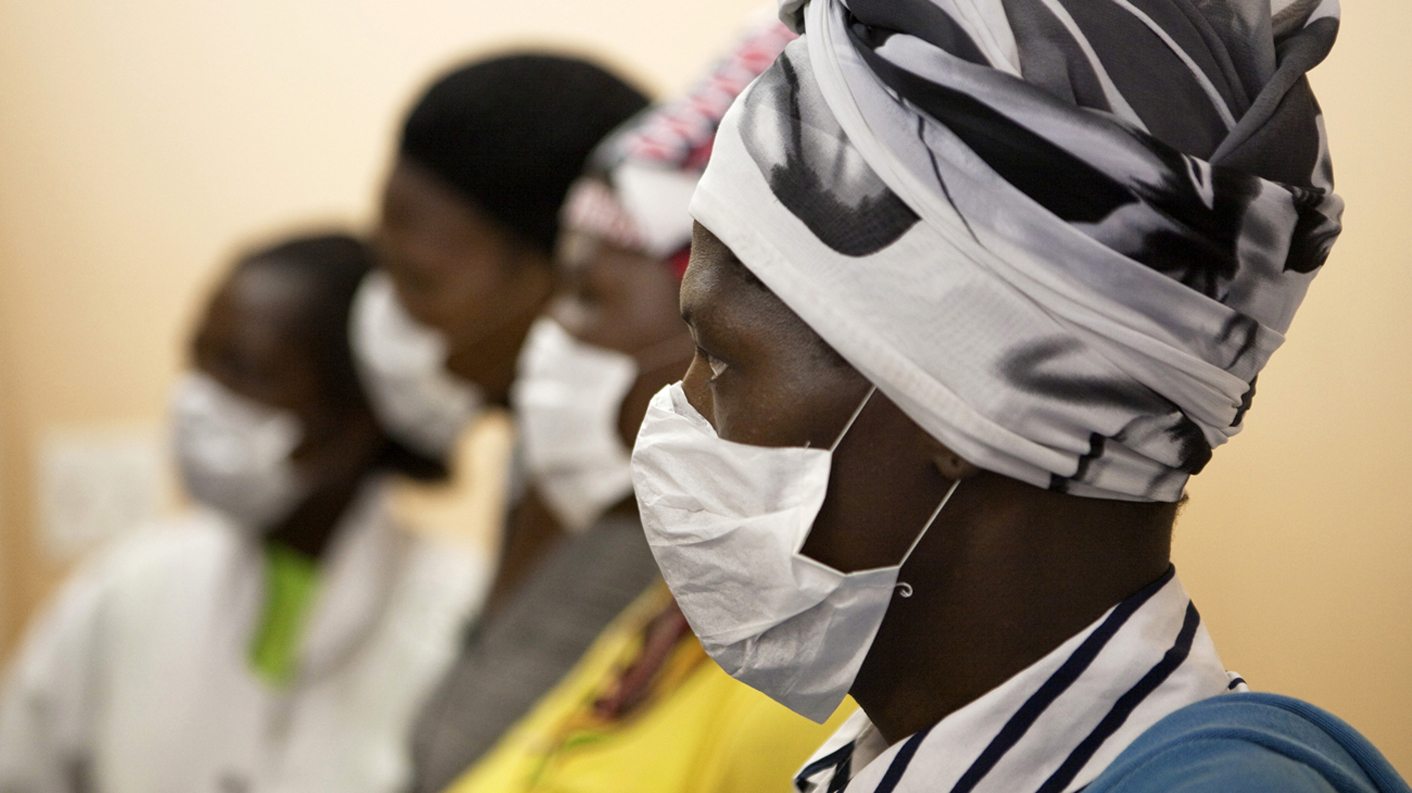 File Photo: Patients with HIV and tuberculosis (TB) wear masks while awaiting consultation at a clinic in Cape Town's Khayelitsha township, February 23, 2010. In South Africa, 5.5 million people live with HIV/AIDS ? more than in any other country - while 33 million people live with the disease worldwide. In Khayelitsha there is a saying, ?Living with HIV, dying from TB?. The weakened immune system leaves those infected vulnerable to infectious diseases like TB, which spreads easily in Khayelitsha?s poor living conditions and dense population. The TB incidence there is among the highest in the world. REUTERS/Finbarr O'Reilly
File Photo: Patients with HIV and tuberculosis (TB) wear masks while awaiting consultation at a clinic in Cape Town's Khayelitsha township, February 23, 2010. In South Africa, 5.5 million people live with HIV/AIDS ? more than in any other country - while 33 million people live with the disease worldwide. In Khayelitsha there is a saying, ?Living with HIV, dying from TB?. The weakened immune system leaves those infected vulnerable to infectious diseases like TB, which spreads easily in Khayelitsha?s poor living conditions and dense population. The TB incidence there is among the highest in the world. REUTERS/Finbarr O'Reilly