SPOTLIGHT
Covid-19: Understanding immunity and what it means for a vaccine
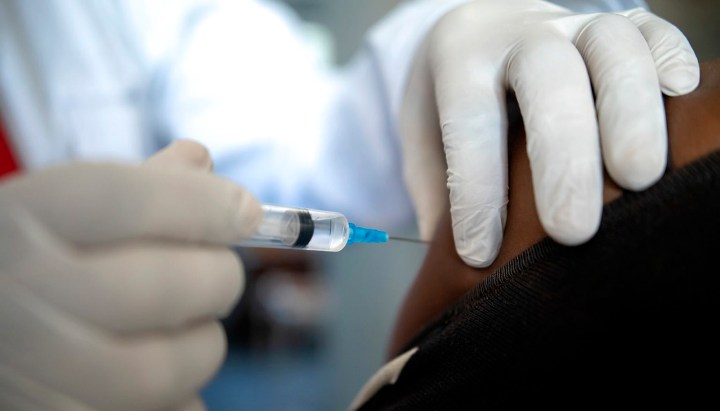
Immunity to Covid-19 is much more interesting and far more complicated than simply something you do or do not have. Kathryn Cleary spoke to two experts about what we know about Covid-19 immunity and the implications of that for antibody testing and the development of vaccines.
It has been more than seven months since the first known case of Covid-19 was confirmed in China and, since then, experts and scientists around the world have been racing to create a vaccine that could give people immunity. But what exactly immunity to Covid-19 might look like is not yet clear – and it is both more interesting and more complicated than simply something you do or do not have.
Immunity, according to the head of immunology at the University of Cape Town, Prof Clive Gray, refers to some level of protection, be it natural or by way of a vaccine. Naturally, our bodies are already equipped to fight off acute viral infections like SARS-CoV-2, the virus that causes the disease Covid-19, through a combination of innate and adaptive immune responses.
Gray explains that, along with antibodies, the immune system produces what are called T-cells and B-cells. Together, these cells work to fight off infections in our bodies by recognising specific parts of the virus called “antigens”, killing off the virus, and storing that information in memory B and T-cells. This way, if we become infected with the same virus again, our body remembers how to fight the infection.
Overall, this process is called a T-cell response, and is the body’s first line of adaptive immunity. The production of antibodies follows a T-cell response, as both T and B-cells are needed for the body to create antibodies.
Different antibodies and what they mean
Antibodies are not all the same – the first antibody that gets released is called an IgM antibody. “That’s the first measurement that we can make of an antibody response, then, later, they switch from an IgM to another type of antibody, and in this case, it could be IgG or IgA, or if you have an allergy response, it could be an IgE. In SARS-CoV-2 infection, it could be either an IgG or an IgA,” says Gray.
Detecting IgM and IgG is crucial for an antibody test to be effective, but with SARS-CoV-2, the timing between an early IgM response, later becoming an IgG response, is slightly unusual as these responses tend to overlap, more so than other viral infections, explains Prof Jonathan Blackburn, head of chemical and systems biology at the University of Cape Town.
“In Covid-19 disease, that difference in timing between IgM arising early and IgG replacing it later, doesn’t seem to happen, meaning that there is a much more truncated time period where you can detect IgM and not IgG, which we don’t yet fully understand,” says Blackburn.
Blackburn and Gray are lead authors of a paper published last week in the South African Medical Journal (SAMJ) on antibody testing for Covid-19. The paper highlights the complexities of antibody tests in relation to the time frame that IgM and IgG antibodies are present in the body following infection, which might only be three months before they disappear. However, while this rapid disappearance of antibodies may sound like a bad thing, it’s completely natural, says Gray, keeping in mind that classically we would have memory B-cells should there be re-infection in the future.
“What’s been found, is that the antibody response, both IgM and IgG and IgA, wane fairly rapidly after symptoms have dissipated. That’s a natural response. That’s going to happen with any infection where symptoms disappear and it’s a resolving infection, so it’s nothing unusual,” adds Gray. What this means, he says, is that when trying to measure the antibody response, or use an antibody test, positive detections can only be made in a time-sensitive window.
Time-sensitive window for antibody testing
“One of the greatest areas of confusion that I see in the antibody field related to Covid-19 is this: if you run an antibody test on an individual and you see that they have antibodies to the virus, does that mean that that person has immunity and could potentially go back to work? In reality, a positive antibody test doesn’t necessarily mean that,” emphasises Blackburn.
“Not all antibodies are protective and we don’t yet know whether everyone with protective antibodies will have a memory B-cell response.”
Gray says an antibody test outcome will not give you a prognosis. “It’s going to tell you that that person has been exposed and has formed an immune response. That’s all it’s going to tell you.”
Keeping the time-specific window in mind, someone who tests negative for an antibody test may have previously been infected, but their antibodies have already waned significantly enough that they are undetectable by the test. Similarly, if the antibody test is done too early, the body may not yet have mounted an antibody response, remembering that this follows a T-cell response. Adding to this, if the body clears the infection purely by a T-cell response before antibody production, an antibody test will not be a useful tool.
This is why the idea that antibody tests could potentially be used as verification or proof of immunity still requires experimental evidence, so further research is needed, says Blackburn.
Vaccine immunity
With vaccine immunity, Gray says it’s unclear what this could be as there is not yet enough available data from ongoing trials. He explains that looking at other vaccines, protective immunity comes from a combination of neutralising antibodies (IgG) and a T-cell response. Recent data released from the Oxford vaccine trial in the UK found that people who were vaccinated had both neutralising antibody responses and good T-cell responses, says Gray.
“I’ve worked in the field of HIV vaccines for 20-odd years and I know that this can mean nothing. We’ve found very good immune responses to other vaccine candidates, but when it translates to protection, it doesn’t. We have to be very cautious with how we interpret the science,” he warns.
Blackburn adds that the trial currently underway in South Africa on the Oxford vaccine is still a Phase I/II safety trial, which strictly seeks to demonstrate that the vaccine doesn’t cause any side effects or harm.
“It’s not really designed to see whether it provides benefit. That comes in efficacy trials which are substantially larger, but of course people are looking as early as possible including in the phase I/II trial to see if there are hints that it might provide some protection,” he says.
Protection from a vaccine depends on memory
Gray says the immune system’s response to a vaccine all depends on memory T and B-cells, and a good memory B-cell response induced from a vaccine is different from a natural immune response.
“When you have a natural infection, we know the immune response – and especially the antibodies – wanes fairly rapidly. That’s a natural response. What we want with a vaccine is quite the opposite, and the way we elicit a response from a vaccine is potentially different from natural infection.
“What we’re looking for are those memory B-cells and memory T-cells. Although we don’t know enough about natural infection [of SARS-CoV-2], right now we know nothing about a vaccine response related to protection. That’s why the next phase of the trials is important as this will tell us whether we have provided protective immunity,” he says.
“In classic immunology, when you’ve been infected with a virus or bacterium, you generate an initial antibody response to that infection and later one would hope that your immune system develops these memory B-cells as well. So, when you’re later re-exposed to the same pathogen, you’ve got a memory and you’ll respond more quickly next time,” adds Blackburn.
However, research is needed to tell us whether a natural SARS-CoV-2 infection produces these much-needed memory cells in individuals.
“The goal of a vaccine is not to produce a high [concentration] of antibodies that is there in perpetuity. The goal of the vaccination is to produce the memory B-cell and memory T-cell responses. Providing this happens, and there is no antigenic drift [change in the coating] in the virus (like that of flu), then in principle you should be protected for life. If there is antigenic drift or you don’t generate a memory B-cell response, then the solution would be repeat vaccinations,” says Blackburn.
“I think we still know so little,” says Gray. “We don’t know what a vaccine response that could cause protection would be.
“We know about antibodies, but the longer the disease and the pandemic runs its course, whatever direct trajectory it takes in South Africa and the globe, as we speak, we currently just know the tip of the iceberg.” DM/MC
This article was produced by Spotlight – health journalism in the public interest. Sign up for our newsletter.
"Information pertaining to Covid-19, vaccines, how to control the spread of the virus and potential treatments is ever-changing. Under the South African Disaster Management Act Regulation 11(5)(c) it is prohibited to publish information through any medium with the intention to deceive people on government measures to address COVID-19. We are therefore disabling the comment section on this article in order to protect both the commenting member and ourselves from potential liability. Should you have additional information that you think we should know, please email [email protected]"




 Become an Insider
Become an Insider