By early July 2020, there were around 150 vaccine candidates for Covid-19 under development, with more than 20 in clinical trials, led by a combination of private companies and public-private partnerships.
In just one of these global clinical trials (Oxford University/AstraZeneca) the South African government, through Wits University, agreed to participate alongside Brazil and the UK. The details of the partnership agreement with the South African government, in relation to access and pricing (should it be successful), has not yet been made public.
Given the unprecedented nature of Covid-19, and coupled with growing reports about global PPE hoarding and profiteering, world leaders called in May for a ‘People’s Vaccine’ which South Africa has signed onto as well.
The People’s Vaccine demands that “all vaccines, treatments, and tests (must) be patent-free, mass produced, distributed fairly, and made available to all people, in all countries, free of charge”. Significantly, it warns that “the world cannot afford monopolies and competition to stand in the way of the universal need to save lives”.
Locally, however, there are concerns that global statements by the South African government are not matched by local political and regulatory action. For example: despite a flurry of lockdown regulations being gazetted, the apartheid era Patents Act, which governs South Africa’s patents system, remains on the statute books, unamended, without the much-needed revisions that would provide a clearer legislative route for equitable, fair and reasonably priced access to testing, vaccines and treatment for Covid-19. This, while other countries, including France, Germany, Canada, Israel, Chile, and Ecuador, have already done so, and despite a revised IP policy framework that seemingly has Cabinet approval.
At present, certain select regulations that deal with expedited inquiries into price gouging for essential supplies are available (using anti-trust mechanisms) but they limit the power of the authorities to excessive pricing matters (not patents), and only after the fact.
So it appears that the South African government will instead rely on its own activism, negotiation, and, dangerously, the benevolence of the global vaccine development industry, during a pandemic, where profiteering is already happening.
Without a clear and enabling legislative framework, access will not be guaranteed – mainly because the default response of powerful vested interests and lobbies before, and during, this crisis has been to rely on our courts and generous jurisprudence – armed with large legal teams from the private sector – for ‘their’ commercial and property rights protection and vindication.
It will be no different with a vaccine, should an ideal candidate be discovered. We are simply putting too much faith in an industry that has not fully supported equitable access to life-saving treatment before.
Multi-government and multi-disciplinary task teams – across regions, with IP lawyers, market and pricing experts – are justified, and must be established to support brave public health vaccine researchers and clinical participants.
Thus, while the political and global space to theoretically ask for equitable access to a vaccine exists (more so than with the HIV/AIDS epidemic), the legal and political system is far from ready, not just in South Africa, but in many other developing countries too. And the global pharmaceutical industry and their shareholders, including the generic manufacturing industry, will be betting on this.
Moreover, as initial supplies of effective vaccines are expected to be insufficient to meet global demand, companies will likely prioritise selling to the highest bidder – or set their initial price high enough to de facto exclude most developing countries.
Added to that is the unprecedented levels of nationalism and hoarding that we are witnessing – from PPE to vaccines, medicines, and diagnostics, with the US president leading the charge, eagerly followed by other countries such as the UK and India.
The tendency to protect national interests and prioritise profit and financial interests over people’s lives (pricing life-saving products as high as “the market can bear” with no reference to actual costs), is not going to disappear. This is why we need to establish a rights-based framework that articulates why and how Covid-19 vaccines, and other medical tools to curb the pandemic, must be seen as global public goods and be made available to all people in equitable ways.
No more colonisation of global health, but a truly equitable contribution of countries globally to both devising and generating the solutions, and having access to them. This must include the political will to craft transparent and binding Covid-19 access agreements.
It is critical to move away from voluntary access agreements to binding commitments – from fluffy words to enforceable guarantees.
What would that look like?
- Countries such as South Africa should actively engage in clinical trials to test candidate vaccines, but on terms that favour people, not companies. This includes scientific co-leadership and transparent and fairly negotiated agreements, with links to building local manufacturing capacity and having guaranteed access to regional supplies.
- Support the building of regional alliances and initiatives (via Africa CDC and AU) to empower a common voice and ensure priority setting in R&D, manufacturing, supply and access that specifically addresses the needs of the continent, or developing countries more generally.
- Demand a seat at the table in global discussions about vaccine R&D, manufacturing, allocation, and supply, especially as they work out allocation and financing policies for developing countries (which are currently driven by multilateral donor politics).
- Prepare the ground politically for possible patent barriers, and ways to overrule those, including amending South Africa’s Patent Law, in line with recent policy proposals.
If we cannot achieve this, then a fatal outcome awaits us: we will lose more lives and pay the price we are literally asked to pay – like HIV/AIDS in the late 1990s and early 2000s in South Africa and elsewhere, where the wealthy and insured could afford to buy life-saving treatment while the poor died prematurely.
Finally, while years of state capture have hollowed out state capacity in South Africa, we have a small window during the pandemic to re-equip the state with the necessary internal and external expertise.
Multi-government and multi-disciplinary task teams – across regions, with IP lawyers, market and pricing experts – are justified, and must be established to support brave public health vaccine researchers and clinical participants.
The alternative is that South Africa, and the developing world, will be the last to benefit from any advances in science, amid mass human suffering and death. DM
Fatima Hassan heads the Health Justice Initiative and is a human rights lawyer and social justice activist. The Health Justice Initiative is a new public health and law initiative focusing on Covid-19, drawing on the expertise of multi-disciplinary researchers in law, economics, and public health, as well as universities and experts in and outside of South Africa.
Els Torreele is a social justice activist and access to medicine researcher and activist and the former Executive Director of the Médecins Sans Frontières Access Campaign.





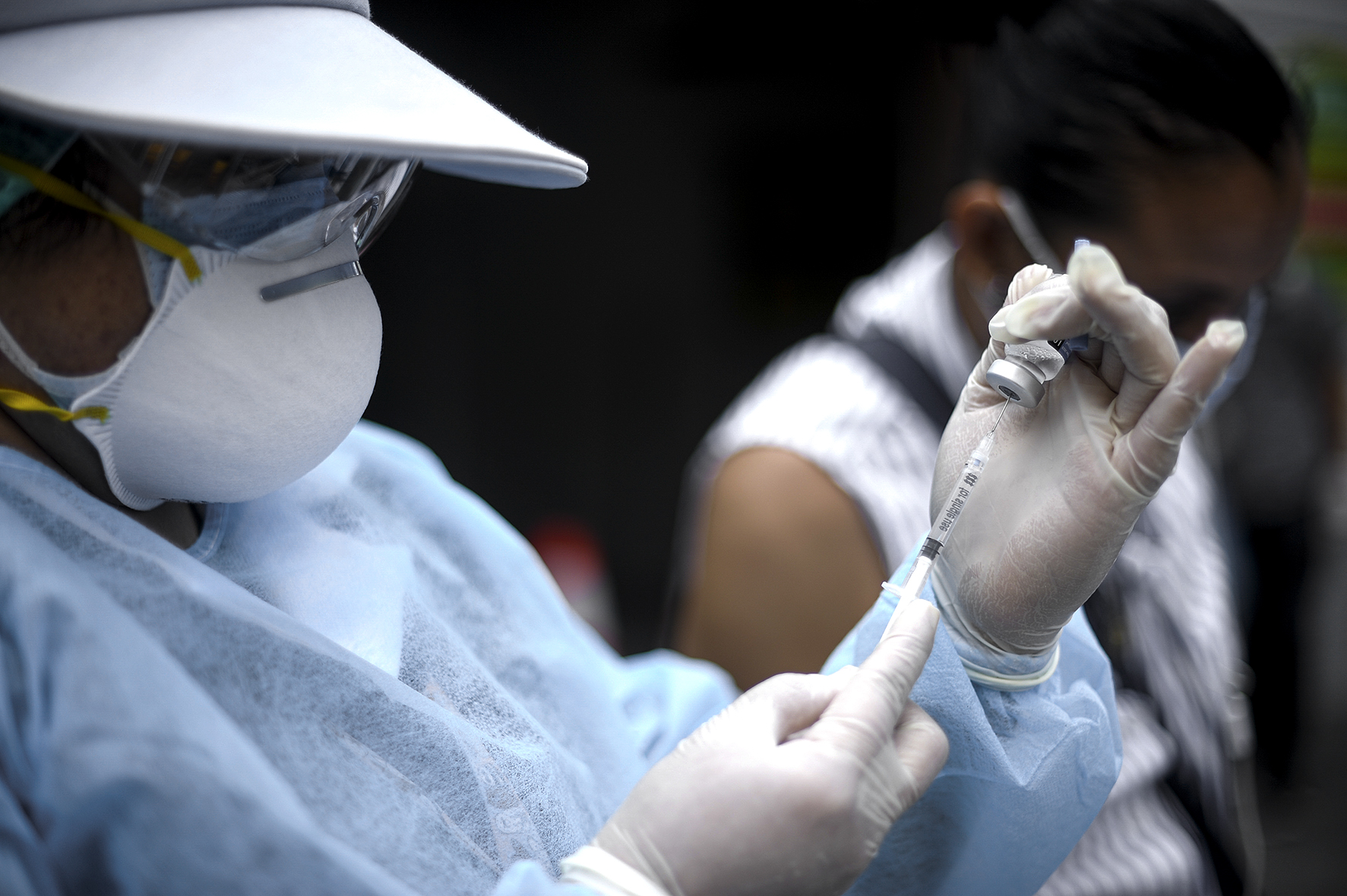 We are putting too much faith in an industry that has not fully supported equitable access to life-saving treatment before, say the writers. (Photo: Camilo Freedman / Bloomberg via Getty Images)
We are putting too much faith in an industry that has not fully supported equitable access to life-saving treatment before, say the writers. (Photo: Camilo Freedman / Bloomberg via Getty Images)