On 2 April, a letter from South Africa’s future arrived from the trenches of the coronavirus battle in New York, the epicentre of the pandemic in the United States.
“Our new reality is unreal,” tweeted Dr Craig Spencer, director of Columbia University’s Global Health in Emergency Medicine.
A veteran of the Ebola emergency response in Guinea in 2014, Spencer said there is “really no way to describe what we’re seeing” in New York.
Each patient going into respiratory distress in their hospitals needs six to eight professionals: nurses, respiratory techs, ER doctors, anaesthetists; each needs an hour or more of treatment time.
“Back to back. All shifts… the mental exhaustion is only starting to set in… I worry about my colleagues. Every day, someone calls me crying. How long will they hold? How long will I hold? The days add up. The worry adds up. I’ve never seen my colleagues so afraid.”
The magnitude of these reports is not lost on Cape Town paramedic Lindiwe (not her real name) who, like many other medical professionals in South Africa, is holding her breath ahead of the coronavirus peaking here.
When coronavirus news first began crowding out headlines in January, Lindiwe wasn’t too worried.
“At first I thought it was something that will pass fast and that it will be alright. But then we started to see the numbers increasing here. I’m not going to lie, this is scary,” she says.
Another letter from the future arrived last Wednesday, when British media reported the death of yet another medic there. Dr Alfa Sa’adu had come out of semi-retirement at the age of 68, to return to the NHS fold where he’d already given more than 40 years of service, to help his colleagues take on the virus. He died after contracting Covid-19 two weeks earlier.
That same day, the tally of doctors killed by Covid-19 disease in Italy reached 66.
“It’s hard putting into words how real this is,” health reporter in New York Jessica Glenza told The Guardian’s podcast Today in Focus.
Speaking of the strain that doctors, nurses and other medical teams are under, she said they were “breaking down in tears at the anxiety”, and how torn they are between the fear of exposure to the virus and their obligation to work.
The medics fear taking the virus home, with some even reporting that they are stripping naked in the hallways of their New York apartment blocks to remove potentially contaminated clothing before stepping inside their homes. They are worried about the shortage of personal protective equipment (PPE), and anticipate running out of ventilators and having to decide “who lives, and who dies”.
“It’s emotional just to talk to frontline workers because of how much stress they’re under, and they’re not even at the peak yet,” Glenza said last week. And this, in her own words, is one of the most well-resourced medical communities in the United States.
SA medics holding their breath
One of the first suspected coronavirus cases that Lindiwe and her EMS crew picked up in March was a woman who was three days into her symptoms, including blurred vision and fever. When the paramedics ran through the screening questions to see if the patient might have coronavirus, the woman answered “no” to all of them.
“But when we got her to hospital, she changed all her answers to ‘yes’ (when she spoke with the doctor).”
With the patient’s symptoms and exposure history suggesting she did have the virus, the paramedics had to move her to another hospital. But they didn’t have the right PPE, were met by unhelpful nursing staff on the other side, and didn’t have anywhere to doff their contaminated clothing once they’d handed the patient over. The ambulance crew had to strip off some of their clothing outside the hospital, in front of the ambulance.
“Ever since then, I’ve been very emotional. When I come home, I cry.”
And this is the quiet before the storm.
Lindiwe’s main worries are for her colleagues who might contract the virus on the job — the EMS crew is like her family, she says. She’s also worried about taking the virus home to her own family, where there are two children aged seven and eight.
“We go home and we think are we safe?”
Normally she loves her work, but with the dark clouds of the pandemic gathering, she finds her shifts suffocating.
“When I get home, I feel like I can breathe again.”
Daily Maverick spoke to a number of medical personnel in public and private healthcare, to get a sense of the mood on the ground. This included doctors, an ER trauma specialist, a cosmetic surgeon who is volunteering at a private hospital while her practice is shut during the lockdown, a paramedic and various therapists. All had to comment anonymously because of their employers’ restrictions on speaking to the media.
Most reported concerns about a shortage of PPE. Some were worried about the inability of the medical infrastructure to cope with the kind of caseloads seen in the north. One mentioned the reluctance of some colleagues to volunteer support because of being parents to young children. Some were anxious that medical employers are unable to give adequate support to their teams through the peak. Some are “stoic”, but most are “holding their breath” in anticipation of what’s coming.
Medics in the public health sector are already stretched beyond capacity, says Kentse Radebe, a fellow with the Tekano Health Equity programme and contributor to the SA Human Rights Commission’s Section 11 Committee report on mental health.
Now, they will be even more stretched as the pandemic spreads here.
“Their stress, anxiety and fear will be heightened now. We must ramp up the emotional support they will need. Even prior to this crisis, we didn’t have a mental health sector that was geared to support professionals in this context.”
Mental health experts step forward for the frontliners
Many of the civil society organisations that already offer mental health support to the public are now rallying to extend this to the medical community, but some of these NGOs are limited by staff capacity and have cut back on operations as they work from home during the lockdown, says Radebe.
The Psychological Society of South Africa (PsySSA) is mobilising an extensive nationwide pool of psychologists to offer pro-bono telephonic debriefing and crisis intervention for medics.
PsySSA executive director Fatima Seedat says the organisation is working closely with the Department of Health to coordinate a response, and has thrown their net widely to draw in volunteers from across the country.
Medical personnel needing mental health support should email PsySSA with their contact details, and their location. Seedat says the organisation will link them up with a therapist in that person’s region, and initiate an introduction that can lead to pro-bono telecounselling.
Therapists can volunteer with PsySSA by signing up through this Google form.
The organisation has also released a special Covid-edition public interest resource kit addressing mental health issues during the crisis.
Another nationwide helpline specifically for medical practitioners during the pandemic is the National Medical Frontliners Counselling Hotline, a 24-hour WhatsApp-based platform (WhatsApp: 079 513 7015). Co-ordinated by Cape Town social worker Kayla-Tess Pattenden, the initiative has drawn together a national pool of volunteer therapists and counsellors to offer pro-bono debriefing and containment therapy for medics (up to three sessions per person).
Pattenden says this is a grassroots initiative that grew out of the number of therapists now stuck at home during the lockdown, who were volunteering their services.
Medics reaching out to the hotline support team will also be given a risk assessment screening, and be asked to give the telephone number of the line-manager within their healthcare institution, should they need to be referred back to their employer for additional treatment or be booked off work for mental health reasons.
The South African Depression and Anxiety Group (Sadag) recommends that emotionally overwhelmed medics contact Sadag’s national hotlines (listed below) and check the Sadag website where it is posting regular Covid-19-related updates about online support, and making toolkits available.
Radebe says it is also critical that institutional culture allows for peer-to-peer support during this time.
“Clinics and hospitals must create an environment where medics can take breaks, get sleep and rest when they need it, and that they can debrief with colleagues,” says Radebe. “We underestimate our own capacity to support one another, even just through speaking with a colleague, asking them how they are feeling, if they want to talk, or if they just want someone to stand next to them for a while.”
Meanwhile, as Lindiwe braces herself for the storm to arrive in the Cape, she gets most of her emotional support from colleagues through a busy WhatsApp chat group.
“I just want to talk,” she says.
Help the women frontlines: what the public can do
“The majority of South Africa’s healthcare workers are women,” says Radebe. “They are often the caregivers at home, looking after children, the elderly, a spouse, or extended family.”
At a community level, Radebe recommends that the public supports these healthcare workers by taking over their responsibilities at home, through cooking meals, childcare, and so forth.
“If you’re the partner or neighbour of a healthcare worker, see how you can help with their home responsibilities.”
Offering support through providing meals on-site is also a good way for people who are sitting at home to help medical frontliners. Radebe recommends finding a local clinic or hospital and using a food delivery service to send meals or food parcels where they are needed.
The final message probably comes from the doctors and nurses in the north, who are pleading with the public, again and again, to stay at home and help stop the spread of the virus. Every infected patient arriving at a hospital increases the likelihood of the medical frontliners getting infected themselves, putting them out of action, and putting their lives at risk. Help save our lives, they say, so that we can save yours. DM /MC
Who to call: mental health hotlines for medics during Covid-19
Psychological Society of South Africa (PsySSA): email executive director Fatima Seedat (fatima@psyssa.com) directly and see the PsySSA online toolkit for Covid-related resources.
- National Medical Frontliners Counselling 24-hour Hotline (WhatsApp): 079 513 7015
- Sadag (24 hour): 0800 456 789 (tel); 31393 (sms)
- Sadag suicide crisis line (24 hour): 0800 567 567
- Sadag (WhatsApp support): 076 882 2775
- Lifeline Crisis (24 hour): 0861 322 322
- Lifeline Counselling (WhatsApp): 065 989 9238
- Gift of the Givers toll-free careline: 0800 786 786
- Substance Use & Abuse hotline: 0800 121 314





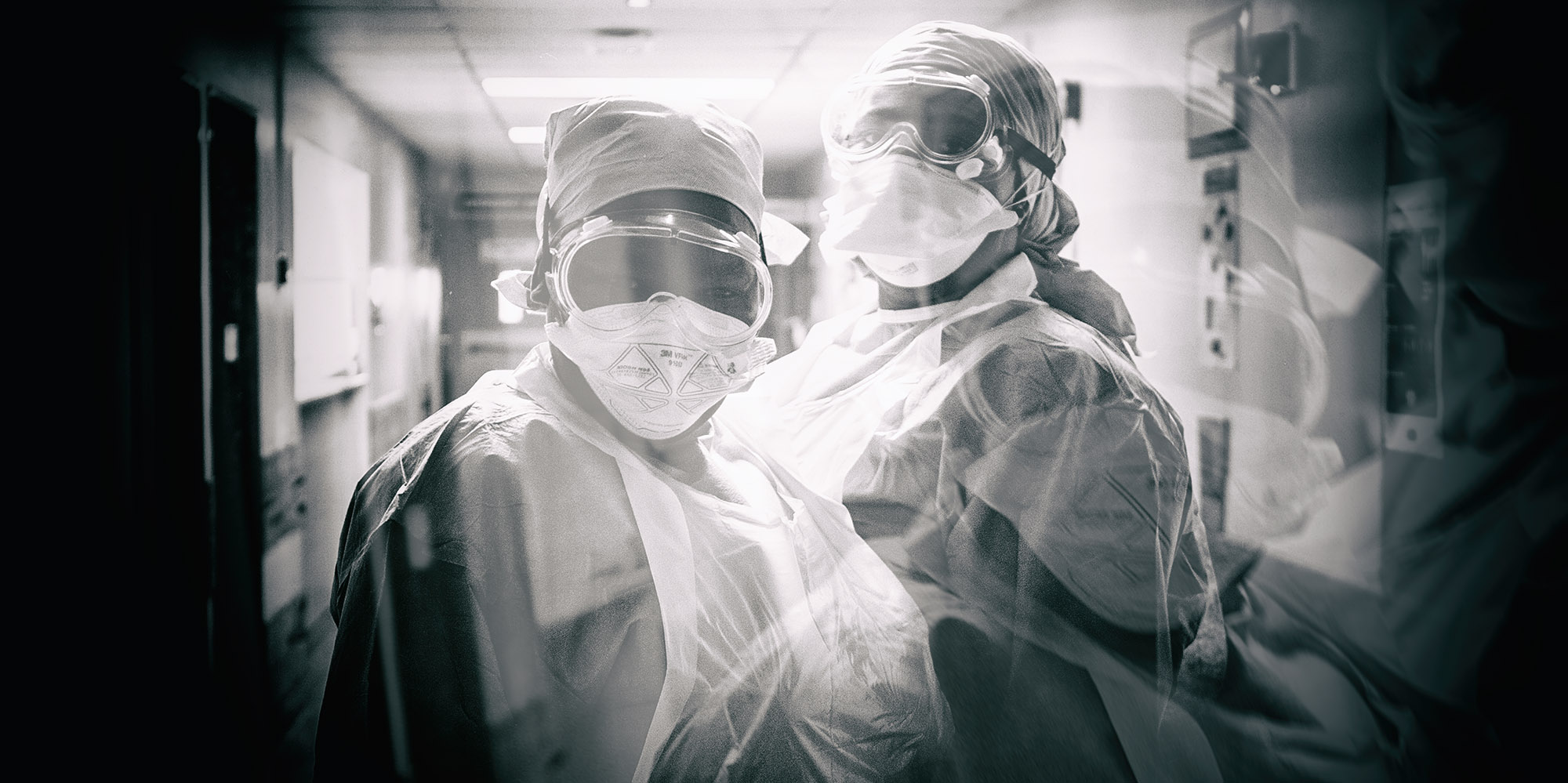 A nurse in an isolation unit at Tygerberg Hospital in the Western Cape on March 11, 2020 in Cape Town, South Africa. (Photo: Misha Jordaan/Gallo Images via Getty Images)
A nurse in an isolation unit at Tygerberg Hospital in the Western Cape on March 11, 2020 in Cape Town, South Africa. (Photo: Misha Jordaan/Gallo Images via Getty Images)