An HIV vaccine remains what South Africa and the world needs to prevent new HIV infections. This is in addition to a range of other HIV prevention tools that are available and in the pipeline. However, one of the HIV vaccine research studies, Uhambo (HVTN 702), has been stopped early because it was determined by an independent review body that it did not show a possibility to prevent HIV. This, for a moment, came as disappointing news; however, as South Africans we realise the search for a safe and effective HIV vaccine has to continue. The early halt cannot be the end; the journey has to continue.
A lot of credit goes to thousands of women and men who out of informed consent volunteer to participate in HIV vaccine studies. We hear from them that they do so out of conviction and commitment to protect the future generations from the effects of HIV. This has brought together communities from rural Mnambithi and Mthatha, to Soshanguve and Khayelitsha townships and another 10 research sites in five provinces. Their lived experience of what HIV is capable of in altering promising young lives has mobilised them to come forward and participate in finding a vaccine.
Communities responded to calls shown by dedicated researchers who led the study, like Dr Mookho Malahleha in Soshanguve and many others who were at the forefront of ensuring this dream becomes a reality. Malahleha’s call on national television on 1 December, 2016 helped galvanise 5,400 participants from communities to participate in the study. The Uhambo study was a true example of scientists, advocates, private and public partnerships journeying together towards a common cause.
With South Africa still carrying the heaviest burden of HIV infections in the world, a commitment to developing an HIV vaccine provided additional hope for the end of AIDS. So when HVTN 702 had to be stopped, the hopes of all involved, for a minute, took a knock. In fact, there is a lot more work that needs to be done, requiring the HIV prevention research community to soldier on and continue the search.
South Africa is involved in other HIV prevention studies that are not only taking place in the country but on other parts of the continent. Another vaccine trial, HVTN 705, also known as the Imbokodo study, is taking place here and elsewhere in southern Africa. It therefore cannot be affected by the cessation of the HVTN 702 study because of the differences in the way the vaccines are developed in both studies. We even hope that research will soon begin for another, known as the PrEPVacc trial, here in South Africa and three other countries. PrEPVacc will compare two different vaccines and incorporate daily oral PrEP in the study design.
We expect results from the AMP study looking at infusions of antibodies later in 2020 and, in the next two years, HPTN 084 looking at an injectable PrEP. HPTN 084 could be taken every two months.
More and more communities in Africa are mobilised, taking part in trials adding to the 5,400 participants in Uhambo. There are more than 7,700 Africans who are participating in HIV prevention efficacy trials, with South African women being at the forefront. Their example ought to be an encouragement to more women and men to volunteer for other HIV prevention trials. We are encouraged that many people are asking to participate and we know they will. South Africans see the urgent need for research to continue to save people now and future generations.
Trial participants and Community Advisory Boards show trust in and build relationships with teams of researchers, community educators, trial health workers, and others who work every day to help find new prevention options. This kind of unity is what we need towards a proud South Africa for a world with no new HIV infections.
While hard at work, waiting for a safe and effective HIV vaccine, we have to make what we currently have work. This is because Uhambo reminds us that more and more HIV prevention strategies have to be radically scaled up. The 4% of women in the study who became infected with HIV should be a wake-up call that South Africa has no option but to do more in making HIV prevention accessible and effective.
In trials, participants are provided with care, a full package of HIV prevention and counselling. That’s evidence that if we provide this kind of targeted service with care, it would help reduce drastically the events of new HIV infections. We need to work harder in involving communities as health providers to help each other in providing HIV prevention services. We have treatment which, when those who live with HIV are supported and take it diligently, will not infect others. Daily PrEP in addition to condoms has to be scaled without fear for those who need it. There’s no emphasising how the health systems can’t be let off the hook on how they fail communities, effectively not helping the efforts of preventing new infections and other health services.
So what’s next for HIV vaccine research in South Africa? We’re resilient. We will keep going. As with so many fights in our past, we don’t have another option. In 2019, according to the WHO 240,000 South Africans were newly infected with HIV. We all have to do what we can to bring that number to zero.
Let’s remember to be thankful for and support all of those 5,400 trial participants and the hundreds of research staff from Khayelitsha to Mnambithi who made this trial possible. Even if we cannot be trial participants, we can support the thousands of participants in other trials now and in the future. Whether trials give us the positive results we hope for or the disappointing ones we don’t want to hear, they give the field more information about how finally to put an end to the increasing numbers of HIV infections.
As civil society we have a role to work with our government and press for accountability in supporting research through funding as well as ensuring communities are mobilised to take part.
Advocates will continue to advocate and agitate for an HIV prevention research sector that is truly driven by communities. We not only hold science to account, we push for meaningful and honest engagement with transparency. Communities are the true backbone of South Africa’s research efforts to find an end to HIV. Leaving them behind by not adequately resourcing them is not in the best interest of ending HIV and its social effects. MC
Ntando Yola is an HIV prevention advocate and a co-founder of Advocacy for Prevention of HIV in Africa (APHA).
Nandisile Luthuli is a Regional Stakeholder Engagement Adviser at AVAC, based in South Africa.




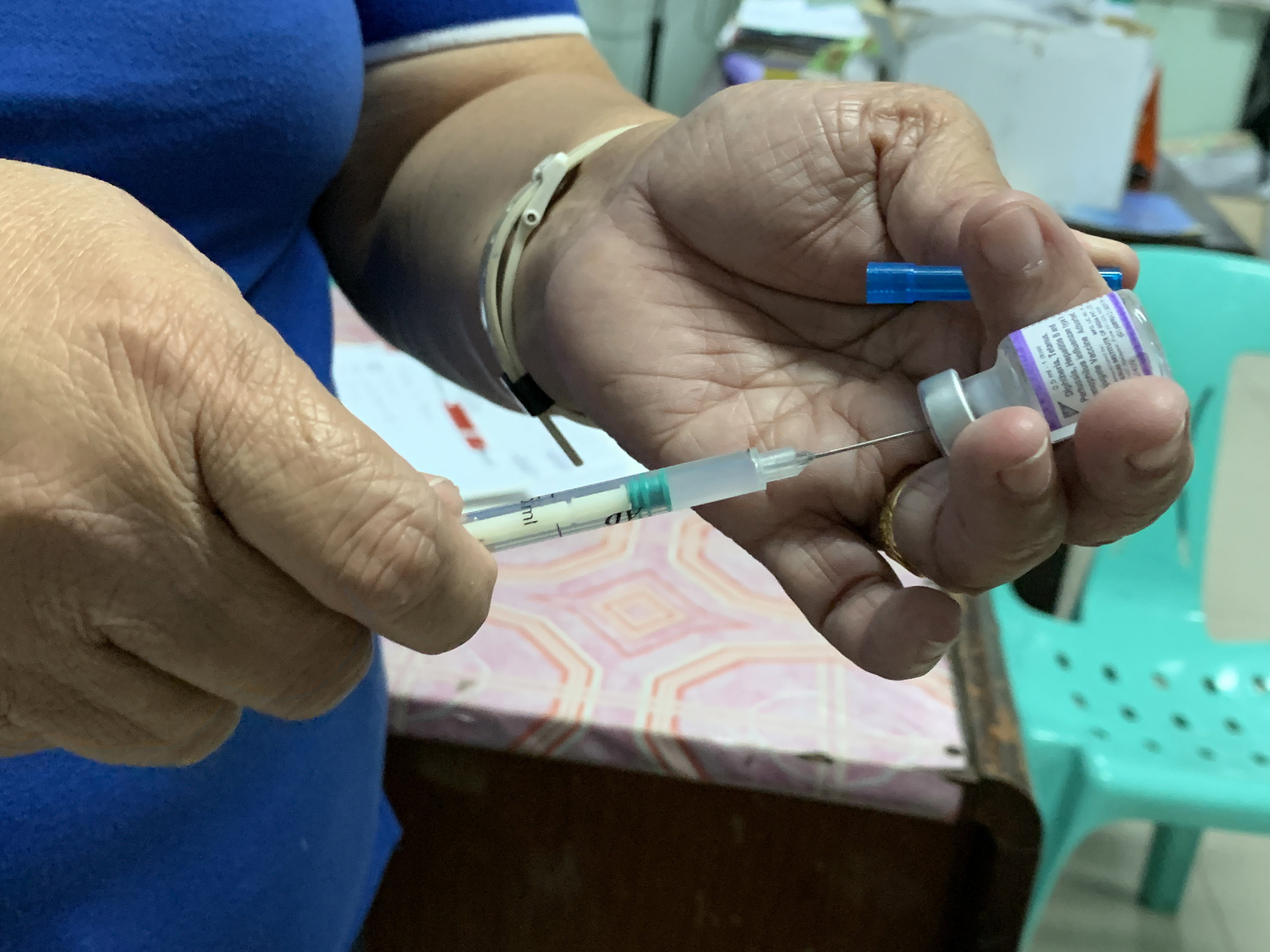 epa07912253 A Filipino health worker prepares a measles vaccine inside a government run health center in Manila, Philippines, 08 October 2019 (issued 11 October 2019). With epidemics of dengue and measles, which have killed more than 1,800 people, and a newly declared polio outbreak, the Philippine health system is overwhelmed and the country is at risk of becoming an incubator for preventable diseases, largely due to the fear of vaccines. The majority of those killed by dengue and measles are children under five, and in the last month two cases of polio have been confirmed - a three-year-old girl in Lanao del Sur and a five-year-old boy in Manila -, a non-curable disease which was eradicated in the country 19 years ago. EPA-EFE/FRANCIS R. MALASIG
epa07912253 A Filipino health worker prepares a measles vaccine inside a government run health center in Manila, Philippines, 08 October 2019 (issued 11 October 2019). With epidemics of dengue and measles, which have killed more than 1,800 people, and a newly declared polio outbreak, the Philippine health system is overwhelmed and the country is at risk of becoming an incubator for preventable diseases, largely due to the fear of vaccines. The majority of those killed by dengue and measles are children under five, and in the last month two cases of polio have been confirmed - a three-year-old girl in Lanao del Sur and a five-year-old boy in Manila -, a non-curable disease which was eradicated in the country 19 years ago. EPA-EFE/FRANCIS R. MALASIG