UNAIDS’ so-called 90-90-90 targets provide one of the best means by which to measure how well we are doing in the HIV response. The three 90s represent three targets relating to HIV testing, treatment, and viral suppression, that are to be met by 2020. The targets have been integrated into South Africa’s National Strategic Plan for HIV, TB and STIs (2017 – 2022), and as such are also national targets.
With a month to go to 2020, we assess South Africa’s progress against the targets using estimates from the Thembisa model. Thembisa is the leading mathematical model of HIV in South Africa and its estimates are used by UNAIDS.
The first 90: 90% of people living with HIV know their status

South Africa’s HIV testing efforts over the last decade have been impressive. As shown in the graph, the country is on course to meet and exceed the first target – with over 90% of people living with HIV knowing their status in 2018. Since new people are constantly becoming infected with HIV, testing efforts will have to be maintained to ensure that this rate does not go down.
The second 90: 90% of people with diagnosed HIV are receiving treatment
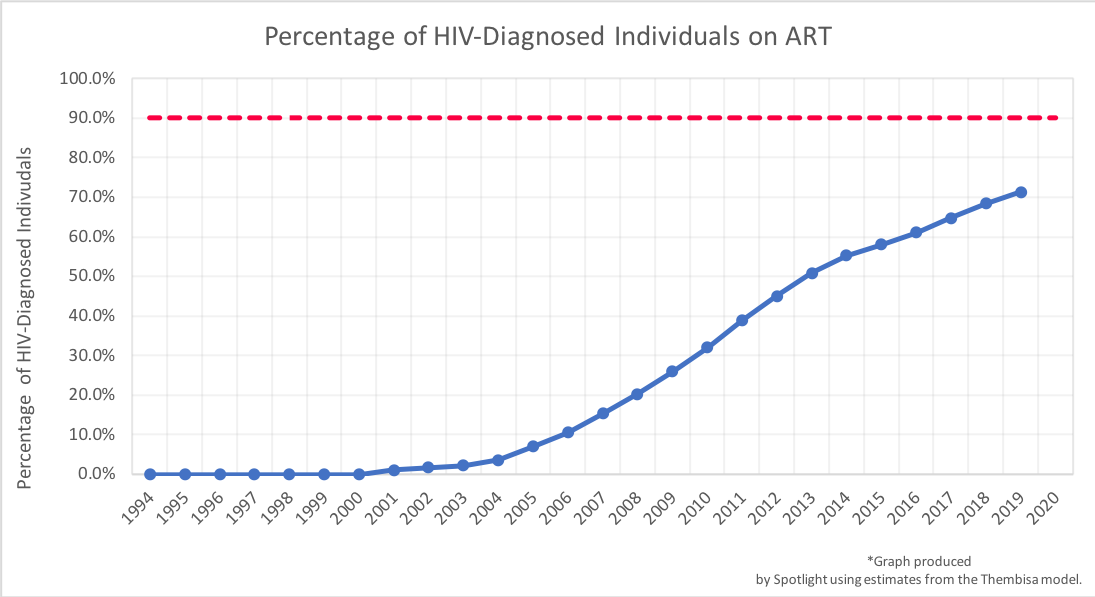
As shown on the graph, South Africa is not on course to meet the second target, with only around 68% of people diagnosed with HIV being on treatment in 2018. This number is anticipated to rise to around 73% in 2020 – still far below the 90% target.
Put another way, around three in 10 people who have been diagnosed with HIV in South Africa are not on treatment. This can either be because they never started taking treatment or because they started, but then stopped. (In another article we argue that this is the number one problem in South Africa’s HIV response.)
In fairness, South Africa’s HIV treatment programme has grown massively over the last decade and the hard work thousands of healthcare workers put into supporting people living with HIV should be acknowledged. The numbers leave no doubt, however, that there is still a long way to go.
The third 90: 90% of people on treatment are virally suppressed
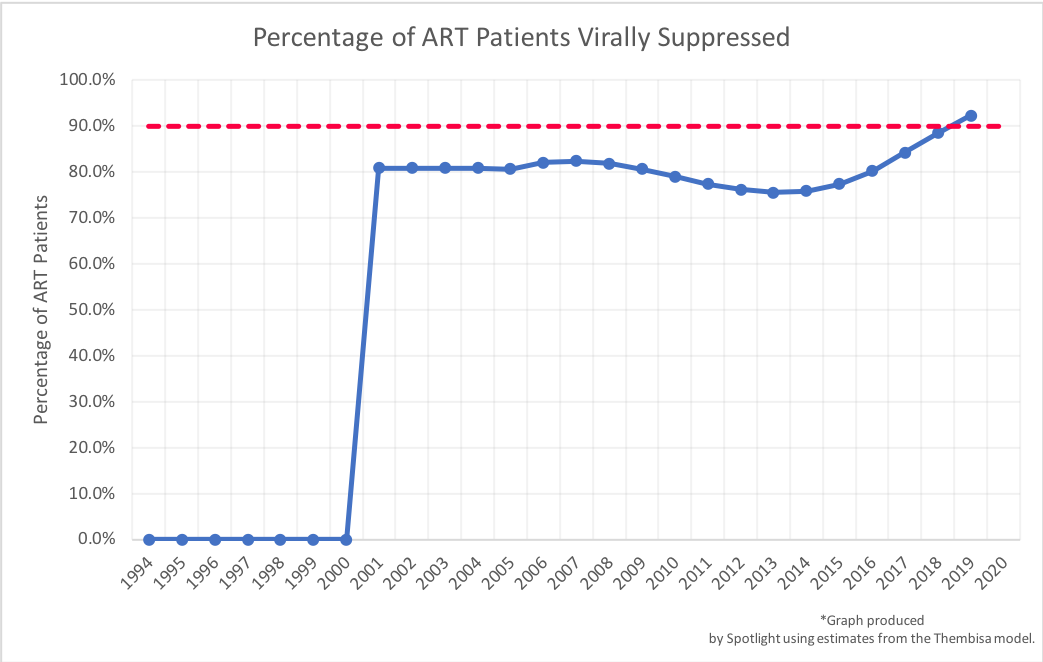
As shown on the graph, South Africa is on course to meet the third target, with around 88% of people on the treatment being virally suppressed in 2018. It is estimated that South Africa would have crossed the 90% mark in 2019 and that we should currently be at around 92%. (This is with a viral load cut-off of 1,000 copies of HIV RNA per millilitre of blood. The percentages are slightly lower if a threshold of 400 is used.)
These numbers tell us that most people who are on treatment are doing well and achieving viral suppression. The high rates here reflect both the fact that ARVs are highly effective, but also the relatively low number of stockouts of the standard first-line ARVs. These rates might well go up even further with the introduction of the new ARV dolutegravir – which is both quick to suppress the virus and has a high barrier to resistance.
The big picture

One shortcoming of the third 90 is that it only tells us what percentage of people who have both tested positive and who are on treatment are virally suppressed. The third 90 does not tell us what percentage of all people who are living with HIV (on treatment or not, diagnosed or not) are virally suppressed.
Since people who are virally suppressed are non-infectious and usually quite healthy, it is useful to know how many people living with HIV are virally suppressed and how many are not. Fortunately, this can easily be calculated by multiplying the three 90s (although this calculation will not take into account the very small number of people who have undetectable viral loads without taking treatment). Since the three 90s are being multiplied with each other, the combined target is 72.9%.
As shown in the graph, only around 55% of all people living with HIV in South Africa were virally suppressed in 2018. While this number should rise to around 62.5% in 2020, we will fall well short of the 72.9% target.
For more graphs showing the state of our HIV response, see HIV in SA: Seven graphs that tell the story. MC
*Thanks to Spotlight volunteer Kayla Kuhfeldt for preparing the graphs used in this article.
This article was produced by Spotlight – health journalism in the public interest.





 AIDS awareness ribbons (Photo: Chamila Karunarathne/EPA-EFE)
AIDS awareness ribbons (Photo: Chamila Karunarathne/EPA-EFE)