We can now breathe a sigh of relief after science has confirmed that using South Africa’s most popular birth control Depot medroxyprogesterone acetate — commonly known as Depo Provera — doesn’t increase women’s risk of HIV infection.
For three decades, observational research has suggested women who use the three-month injection could be at a higher risk of HIV. This is how the Evidence for Contraceptive Options and HIV Outcomes (ECHO) Study was born.
The study was not only about putting an end to the worldwide speculation and confusion about Depo. It also investigated whether or not two other contraception methods — a 10-year small copper IUD and a two-month progestin-only injection — increase the chances of contracting HIV.
Now we know there is no link between these birth controls and HIV risk.
While this is the best outcome, these results paint a grim picture of our fight against HIV — where young black women continue to bear the brunt.
Researchers found an alarmingly high HIV rate among the study’s participants. Close to 400 of the 7,829 women who took part in the study were infected with HIV during the trial. This means, about four in every 100 women were infected with the virus each year.
“[There were] 143 HIV infections in women who used Depo Provera, 138 from those on the copper-bearing IUD and 116 in women who used a levonorgestrel implant,” member of the ECHO management team Dr Jared Baeten said during the study’s launch at the ninth South Africa Aids Conference in Durban.
Additionally, sexually transmitted infections were common at the start of the trial; with 18% having chlamydia, 5% gonorrhoea and 38% with the herpes simplex virus.
What these findings tell us is that unsafe sex is definitely happening; half of the study participants also reported not using a condom the last time they had sex at the time of enrollment.
We don’t know the reasons for this as the study did not offer any qualitative findings. But previous studies point to one culprit.
Patriarchy.
Heterosexual women often struggle to convince their sexual partners to use condoms. This can be exacerbated when they’re in romantic relationships. For instance, a 2017 study published in the Global Health Action journal found that although women reported negotiating safe sex in their relationships, they feared the possible consequences of insisting on using condoms with their partners.
But, female condoms could be the game-changer as studies have shown that they give women more power to negotiate in the bedroom.
If only they were as available as the male condom.
Female condoms are hard to find even in public clinics, mostly because of the cost of making them, which is about nine rand per female condom as compared to approximately 30 cents for one male condom. Because of this, government procures a much lower number of female condoms, and to add to that, a pack of two Cupid female condoms retails for about R40 in the private sector.
How does this affect South Africa’s policy?
Well, government intends to distribute at least 850 million male condoms and 33 to 40 million female condoms (as stated in the latest strategic plan for HIV), which is a staggering five per cent of the number of the male versions.
This shows us that preventing new HIV infections will not happen without considering the personal, the political and the theoretical.
“We’ve all maintained that HIV is not just a medical condition, it’s also a socio-political one,” Soul City CEO Lebogang Ramafoko told Health-e. “The ECHO study is revealing that we need to take stock of what we’ve done to address social, structural and commercial determinants of health. A lot of investments have gone into biomedical interventions, such as medical male circumcision and the HIV prevention pill Pre-Exposure Prophylaxis — simply known as PrEP.”
Our HIV prevention methods need to focus more on other factors that are outside of the medicine, Ramafoko added, such as gender-based violence, poverty and patriarchy.
This same patriarchy prevents a young woman from going into clinics to ask a health worker for the only two things that can prevent her from HIV — PrEP and condoms. That same patriarchy follows her into her bedroom, where condom use is out her hands.
This system is insidious.
It creeps into clinic corridors where women seeking information about their birth control options are herded like cattle and told what is good for them with no consideration given to their wants or needs.
While activists have welcomed the clarity regarding the link between HIV and birth control methods, especially Depo Provera, some are concerned that the study doesn’t address the concerns and questions about the three-month injection being forced onto women.
For instance, a nurse in Mpumalanga told 20-year-old Pearl Mahlangu that using Depo Provera makes it harder to fall pregnant because “it stays longer in the system”.
“I didn’t choose Depo Provera,” she told Health-e. “The nurses made the choice for me.”
Now, Mahlangu has severe side effects such as uncontrollable headaches and heavy bleeding. She wants to change to oral contraceptives.
Meanwhile, Thabsile Shongwe, 30, who is also from Mpumalanga said nurses put her on the three-month injection after she had her second baby. “The side effects are horrible. I no longer have my period, I eat too much and I have a very smelly discharge and I was told by nurses that it’s normal.”
Patriarchy is persistent.
And it should be blamed for the 397 new HIV infections that happened during the ECHO study — despite participants having access to all the biomedical resources needed to prevent this.
Professor Helen Rees, who is a member of the ECHO study management team, echoed these sentiments.
The truth of the matter, she said, is that it was impossible to have 100% HIV prevention in this study — as well as other similar prevention studies — even when PrEP and condoms are available because of the context of these women’s lives and the possible gender dynamics they may find themselves in.
“This is what we're battling with in terms of HIV prevention. Even in an optimised setting [such as the ECHO study], the prevention tools we currently have are not adequate to completely reduce HIV incidents down to zero,” she explained.
It’s great that we now have certainty about Depo Provera and other birth controls’ risk of HIV acquisition. What has been dubbed as a “public health conundrum” is over, but the pieces of the puzzle do not fit perfectly just yet.
Now we know. But the ECHO study findings are not a victory. Instead, they validate that medical solutions will only take us so far. It’s patriarchy that we need to destroy to protect the lives of black women. DM




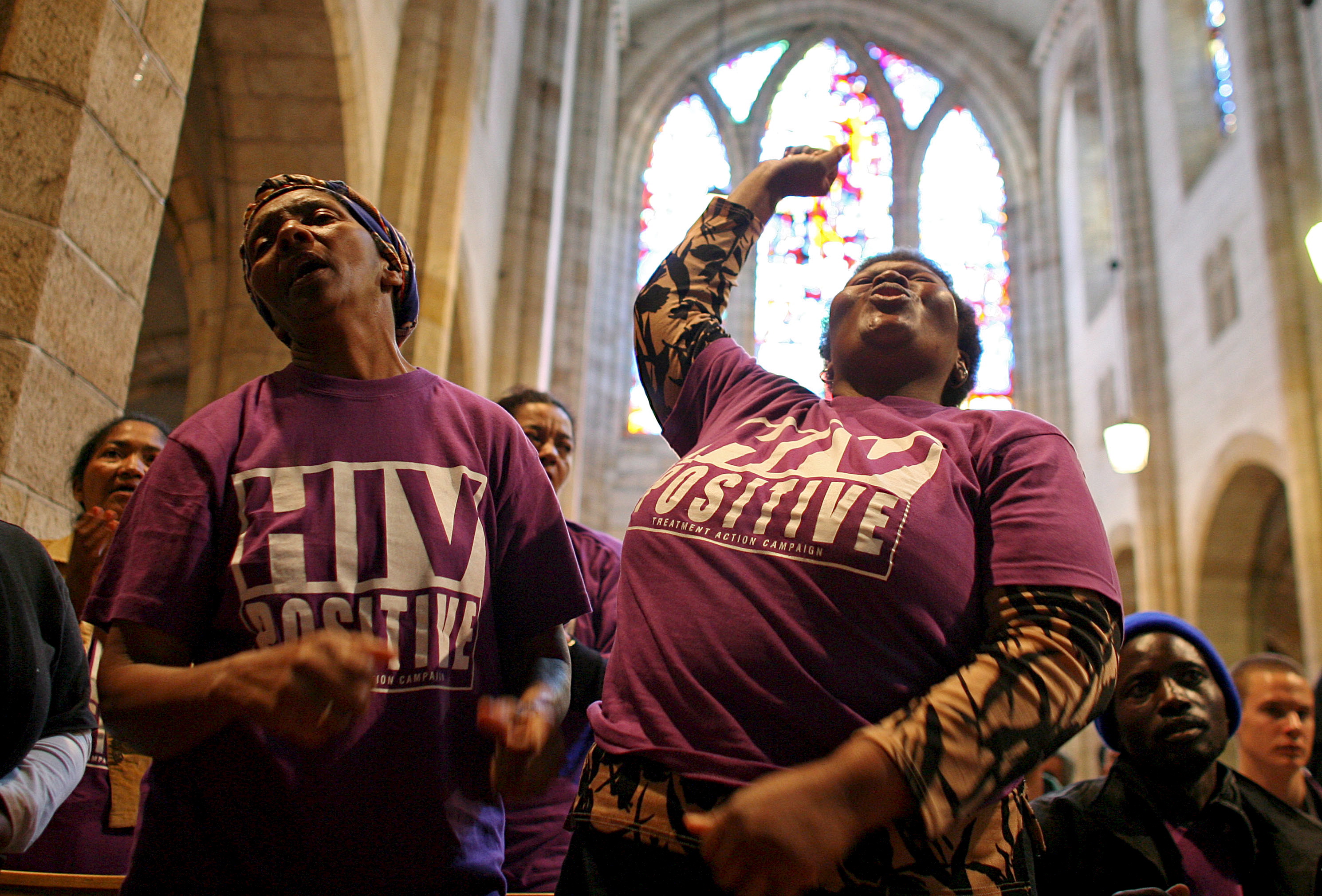 South African HIV/Aids action group members of the Treatment Action Campaign (TAC) protest during a meeting at St.Georges Cathedral in Cape Town, South Africa 29 August 2007.EPA/NIC BOTHMA
South African HIV/Aids action group members of the Treatment Action Campaign (TAC) protest during a meeting at St.Georges Cathedral in Cape Town, South Africa 29 August 2007.EPA/NIC BOTHMA