From the donors’ perspective, one idea behind decreased funding is that middle-income countries (those with a per capita income between $1,045 and $12,736) should be able to pay for the wellbeing of their own populations and address inequality. This is, of course, the dream. But the reality is that the world has a long way to go before equality, and, in the meantime, countries with more wealth do not necessarily have wealthier, healthier people. Already, 70 percent of the world’s poor people live in middle-income countries; by 2020, 70 percent of people living with HIV will as well.
Some public health advocates worry that donors shifted priorities without regard for whether former “recipient” countries were ready to transition away from external funding or — importantly — to do so in a way that protects the human rights of socially excluded groups who have historically been neglected by their governments and benefited from external aid.
In the context of HIV/Aids, the groups that are most at risk in the funding shift are those who have been the most marginalised in any society: people who use drugs; sex workers; and gay, lesbian, and transgender people, many of whom represent the majority of HIV cases in middle-income countries. These fears are already playing out. In Romania, where people who use drugs face barriers to access to services, and in Trinidad, where homosexuality is illegal, we have seen increasing HIV prevalence following donor withdrawal.
Questions about how to fill the funding gap left by the withdrawal of foreign assistance for health are gaining prominence among donors, civil society actors, and the private sector. This period of uncertainty provides fertile ground for private sector actors, including through the use of so-called public-private partnerships, which combine government and private resources to deliver social good and sometimes profits. While this seems like an attractive option for countries looking to diversify funding sources, it remains to be seen whether such models are more effective than aid or government funds alone.
The private sector has always played a prominent role in development, even before the “post-aid” era. An important question for middle-income democracies, though, is how to hold an increasingly diverse array of actors accountable for health-related decision-making. What if a health-related investment negotiated in a private board room proves ineffective? What if this decision is not based on the best available evidence? How can advocates, health service providers, and affected populations participate effectively in a process that is, by definition, partially private?
These questions couldn’t be timelier. This week, 18,000 government and industry representatives, scientists, and health activists gather for the 21st International AIDS Conference in Durban, South Africa to discuss the current state of the global Aids response. The conference is the largest on any global health or development issue in the world, and, as funding for the HIV response shrinks, the future of global health financing is on the agenda.
Certain kinds of public-private partnerships and other models of “blended” financing will undoubtedly be put forward as innovative approaches to fill funding gaps. These proposals may be based, in part, on unexamined assumptions that a private sector approach is inherently leaner, more efficient, and more effective than public funding mechanisms. But the value of public private partnerships does not lend itself to generalizations. We need more evidence to determine whether and under what circumstances these approaches lead to better health outcomes. Most importantly, we must think hard about how principles of good governance - transparency, accountability, and participation – can inform decision-making in these emerging models. The ultimate test should be whether they advance or hinder progress towards the human right to health.
One example demonstrates why a deeper and more honest discussion is necessary. In 2009, the government of Lesotho signed an 18-year contract with a private South African hospital to replace the main hospital in Lesotho’s capital, a deal promoted by the World Bank’s investment arm.
The Queen ‘Mamohato Memorial Hospital’ opened in 2011. According to a 2014 report by OXFAM, the hospital takes up 51 percent of Lesotho’s health budget, costing $67 million per year to operate — three times what the old hospital cost. Lesotho’s government plans to build a new public hospital to care for patients because the cost of treating them at Queen Mamohato Memorial is too high. And yet, in another way the partnership has been an enormous success. It is expected to generate a 25 percent rate of return on equity for the project’s shareholders and a total projected income nearly eight times higher than the original investment.
Discussions at the Aids Conference would benefit from some healthy reflection on whether public-private partnerships and other modes of blended finance are indeed the “magic bullets” in the next wave of health financing that some purport them to be. And here they can draw lessons from the legacy of early Aids activists.
From the beginning of the Aids epidemic, people with HIV — denied affordable medicines by their governments and pharmaceutical companies alike — immediately understood that they had to take control of the decision-making process. They created seats at the table for advocates in health decision making bodies from the Global Fund to the Joint United Nations Programme on HIV/ Aids to National Aids Councils to local clinics. From those seats, they advocated not just for affordable medicines, but for anti-discrimination measures and repeal of laws that criminalised HIV risk behaviors such as sex work, sex between men, and injection drug use.
This experience shows that health policies should be set by those most affected, not negotiated between governments and their investment partners. It is that foundation that we stand to lose if conversations about public health decisions are moved out of public spaces, if donors rather than recipients of aid regain control of the agenda.
In 2016 and onward, we need to open up the debate about donor withdrawal from middle-income countries, exploring roles for governments, donors, civil society, and the private sector that would advance human rights and preserve and build on the gains of the global HIV response. It would be a breakthrough for the Aids movement to come up with minimum human rights standards for innovative financing approaches and public private partnerships in health. Let us start this discussion in Durban. DM
Julia Greenberg directs the Global Health Financing Initiative at the Open Society Foundations.
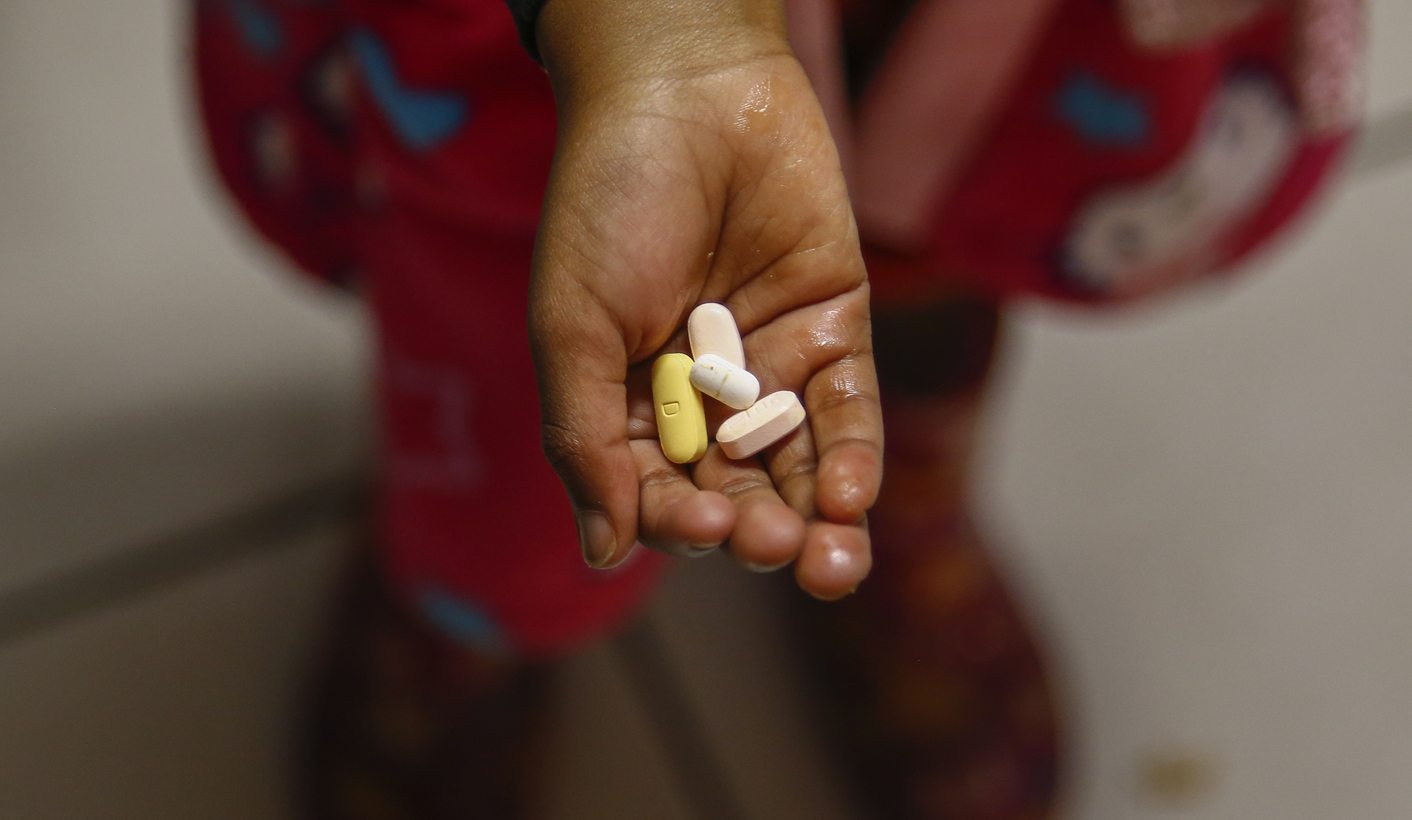
Photo: A South African child holds Antiretroviral (ARV) drugs prior to the daily routine of medicine taking at the HOKISA childrens home in Masiphumelele, Cape Town, South Africa 19 July 2016. EPA/NIC BOTHMA