South Africa
SA healthcare: Some are still more equal than others
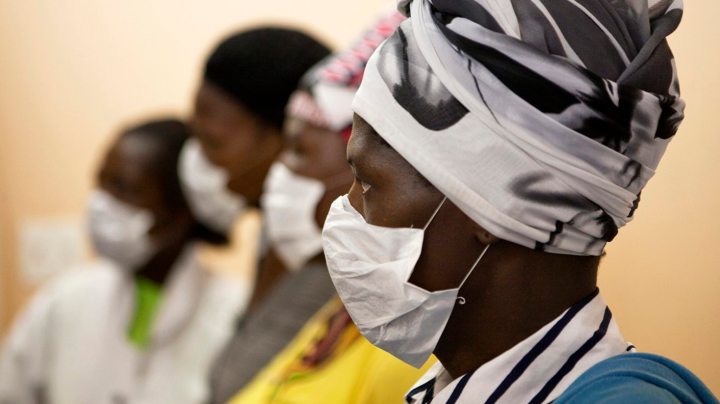
On Tuesday, Stats SA released a report on the health of the nation, based on data from 2011’s General Household Survey. The results are pretty upbeat in some regards – for instance, the South Africans surveyed mainly expressed satisfaction with their last visit to a health facility. But the report also highlights the unavoidable fact that South Africa’s health system is still rife with inequality which still correlates with race. Indeed, it would seem as if depressingly little has changed in this regard over the last twelve years. By REBECCA DAVIS.
“Use of health facilities and levels of selected health conditions in South Africa” is the decidedly non-alluring title of Stats SA’s latest report, which Statistician-General Pali Lehohla released to the media in Stellenbosch on Tuesday. While Stats SA doesn’t conduct a dedicated health survey, there are health-related questions which form part of the General Household Survey. This study is based on that survey, which consisted of interviews with just over 25,000 South African households carried out between July and September 2011.
What the study makes clear most plainly is that access to healthcare in South Africa is still very different for black and white South Africans. Beyond this, the province in which you live also plays a role in determining the ease of your access to healthcare, and its quality. As illustration, 62% of households in the Western Cape take less than 15 minutes to reach their nearest health facility. In the Eastern Cape, only 28% of households are this lucky. Individuals in KwaZulu Natal are most likely not to use the health facility nearest to their dwelling due to long waiting lines. As with so many other aspects of South African life, those in rural areas end up worst off.
The study’s findings are perhaps most revealing when compared with a previous survey of this kind. In 2004, Stats SA brought out a study titled “Perceived health and other health indicators in South Africa”, which consisted of an analysis of data gathered way back in 1999. The two studies do not overlap perfectly, because the 1999 survey contained a number of categories that its 2011 incarnation apparently lacked (unless the relevant data is being held back for a further report). In particular, the 2004 report on 1999’s data spends a lot of time discussing the “perceived health” of members of a household. Among the interesting findings of this were that in 1999, “among both women and men, those who had never married were generally perceived as having better health than those who were married”.
The 2011 survey focused on asking respondents for information on specific diseases or conditions that they said they suffered from. The results are sometimes intriguing: can it really be true, for instance, that Indians are more likely to have both asthma and diabetes than any other South African race group? Asking people to self-report on illness will always leave results open to skepticism: there are many reasons why people might either under-report or over-report illness.
“Obviously a survey method has limits,” confirms UCT’s public health head Leslie London. “Depending on how the survey is done, what methods are used to encourage participation, how well the interviewers are trained, language issues and so on, there will be varying degrees of accuracy.”
London says that something which might give a clue to the levels of illness under-reporting in the 2011 survey is that less than 3% of people aged 15 years or older said that they had been diagnosed with HIV or Aids. “We know the general prevalence of HIV in the whole population is hovering at about 11%, so one could take that as a rough measure of how much under-reporting might play a role, though for different conditions it will vary widely,” London told the Daily Maverick. “There is certainly less stigma in admitting to having arthritis than in having HIV or perhaps TB.”
There are a number of areas in which the 1999 data and the 2011 data may be compared, albeit imperfectly, however. One is the issue of medical aid. In 1999, 18,5% of the population aged 20 and above was reported to have “access to medical benefits”, and their health was perceived as better than those without such access. It’s difficult to compare the 1999 figures with the 2011 figures because the former only took in individuals over 20 years old, whereas the later figures seem to cover everybody. Taken at face value, though, the proportion of black South Africans who were covered by medical aid in 1999 was actually slightly higher than it is now. The figure stood at 8,9% in 1999, and is now at 8,8%. There has been a slight rise in white coverage, from 67,4% in 1999 to 69,6% in 2011.
Again, there are provincial differences at play here too. In 2011 the wealthiest provinces – Western Cape and Gauteng – had the highest percentage of the population covered by medical aid: 25% in the Western Cape and 23,7% in Gauteng. In Limpopo, by contrast, only 7,2% of residents were covered. Overall, the study states, “the younger population; the black Africans; and those residing in Limpopo had the least coverage of medical aid”.
Predictably, the same kind of pattern is found with regards to who’s using public or private healthcare. In 2011, over 81% of black South Africans and over 63% of coloured South Africans mostly used public sector health facilities, whereas 88% of white South Africans favoured private facilities, as did over 64% of Indian South Africans. Overall, the first port of call for the majority of households when illness strikes is a public sector clinic. The percentage of people using private health facilities rather than public actually seems to have dropped since 1999.
One interesting aspect of the 2011 survey is that the number of South Africans who consult traditional healers seems to be lower than one might expect. The survey found that just 5% of South Africans are in a category of people who consult traditional healers, spiritual healers and homeopaths. Again, however, London warned against reading too much into this.
“It is almost certainly what people felt the interviewer wanted to hear – and so they did not report using traditional healing to the extent that it is likely in use. That may have many reasons, to do with interpreting what is meant by health care, stigma, and so on,” London said. “However, it is also probably true that use of traditional healing is not as common as people think. There is a kind of urban legend that every African makes use of traditional medicine, whether they use allopathic [‘Western’] medicine or not. I think that is an exaggeration, but as for what the exact figure is – I don’t think we have hard evidence.”
The latest study has a silver lining, however, in that it reports that the majority of South Africans were happy with their last healthcare encounter. Overall, 74,5% of respondents said they were very satisfied with the last health service they received, and less than 4% were very dissatisfied. Isn’t this reason for celebration? London urges caution again: “What patients express as satisfaction is a function of experience and of expectations,” he says.
London points out that a patient who is sent from the Western Cape to rural Limpopo for treatment would likely have quite different satisfaction levels than the patient who has only been in Limpopo. “Being unhappy because you have come to have high expectations is different from reacting to atrocious care with dissatisfaction.”
Nonetheless, London feels there is some reason to be upbeat: “For the vast majority of South Africans, health services have probably improved and that’s a good thing.”
What remains a concern is the inequality of treatment available to white and black people and rich and poor. “We know that the quality of care received by black people in South Africa is far worse than that received by whites,” London states. From this perspective, the study will provide grist to the mill of advocates for the National Health Insurance. Though the scheme – which aims to provide free healthcare to all South Africans – will take an estimated 14 years to roll out, it is already being implemented in its first phase.
“The information presented in this report shows that the black African population group and people residing in less privileged provinces continue to be disadvantaged in terms of the general aspects of health,” Stats SA concludes. The NHI aims at levelling the very unequal field. DM
Read more:
- National Health Insurance: The first 18 months, in the South African Medical Journal
Photo: Patients with HIV and tuberculosis (TB) wear masks while awaiting consultation at a clinic in Cape Town’s Khayelitsha township, February 23, 2010. REUTERS/Finbarr O’Reilly.
















 Become an Insider
Become an Insider